Clinical Examination in ENT - Tools & Tricks
- Head Mirror & Light: (Bull's lamp/LED) Non-dominant eye; focal length ~20-25 cm.
- Aural Speculum: Largest comfortable; pull pinna up & back (adults), down & back (children).
- Tuning Forks: (512 Hz for Rinne/Weber). 📌 Strike gently, place firmly.
- Nasal Speculum: (Thudichum's) Blades open vertically.
- Tongue Depressor: Depress anterior 2/3rds.
- Laryngeal Mirrors: Warm to prevent fogging.
- Jobson Horne Probe: Wax/foreign body.
- Siegle's Speculum: TM mobility.

⭐ Standard tuning fork frequency for clinical hearing tests (Rinne, Weber) is 512 Hz as it provides the best balance between decay time and bone conduction perception.
Clinical Examination in ENT - Sound Sleuthing
- Otoscopy: Inspect External Auditory Canal (EAC) & Tympanic Membrane (TM).
- Tuning Fork Tests (TFTs): Standard 512 Hz fork.
- Rinne Test: Compares Air Conduction (AC) & Bone Conduction (BC).
- Normal/SNHL: AC > BC (Positive).
- CHL: BC > AC (Negative).
- Weber Test: Lateralization.
- CHL: Towards diseased ear.
- SNHL: Towards better ear.
- Schwabach Test: Compares patient's BC to examiner's.
- Rinne Test: Compares Air Conduction (AC) & Bone Conduction (BC).
- Audiometry:
- Pure Tone Audiometry (PTA): Hearing thresholds.
- Impedance Audiometry: Middle ear function (Tympanometry, Stapedial reflex).
⭐ A 512 Hz tuning fork is preferred for clinical hearing tests as it balances audibility and minimizes vibratory sensation.

Clinical Examination in ENT - Sniffing Out Signs
- External Nose & Vestibule:
- Inspect: Deformities, skin (rhinophyma); vestibule (furuncles, crusting).
- Anterior Rhinoscopy (Thudichum's speculum):
- Septum: DNS, spurs, perforations; Kiesselbach's plexus (bleeding).
- Lateral Wall: Turbinates (size, color, hypertrophy); meatus (discharge, polyps).
- Posterior Rhinoscopy (Mirror):
- Visualize: Choanae, Eustachian tube (ET) openings, adenoids, Fossa of Rosenmüller.
- Sinus Examination:
- Palpate: Frontal, maxillary sinus tenderness.
- Transilluminate: Maxillary/frontal sinuses (↓ glow if sinusitis).
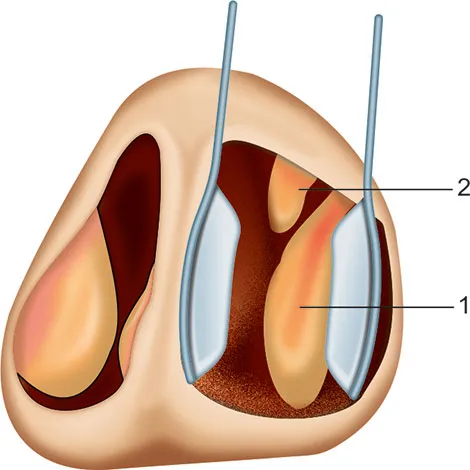
⭐ The Fossa of Rosenmüller, a common site for nasopharyngeal carcinoma, is best visualized during posterior rhinoscopy.
Clinical Examination in ENT - Oral Odyssey
- Inspection: Systematic approach.
- Lips: Symmetry, color, lesions.
- Buccal mucosa, gingiva, teeth (note caries, missing teeth).
- Tongue: Dorsum, ventral surface, lateral borders. Assess mobility (CN XII), papillae.
- Palate: Hard & soft; uvula (midline, movement on phonation).
- Tonsils: Size (Brodsky 0-4), crypts, exudate, symmetry.
- Oropharynx: Posterior wall, pillars.
- Palpation: Bimanual for floor of mouth, tongue base, and any lesions. Note tenderness, induration, fixity.
- Duct Openings: Stensen's (parotid - opposite upper 2nd molar), Wharton's (submandibular - floor of mouth).
- Tools: Bright light source, tongue depressor(s).
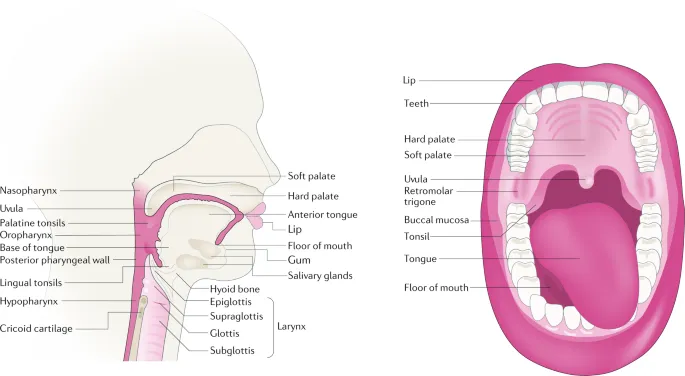
⭐ Ludwig's angina: a rapidly progressive, potentially life-threatening cellulitis of the submandibular, sublingual, and submental spaces. Often odontogenic; airway compromise is a critical concern.
Word count: 93
Clinical Examination in ENT - Voice & Vital Nodes
- Voice Assessment (GRBAS Scale):
- Grade, Roughness, Breathiness, Asthenia, Strain.
- Hoarseness: key symptom (e.g., laryngitis, palsy, nodules, malignancy).
- Stridor: Inspiratory (laryngeal), Expiratory (tracheal), Biphasic (subglottic).
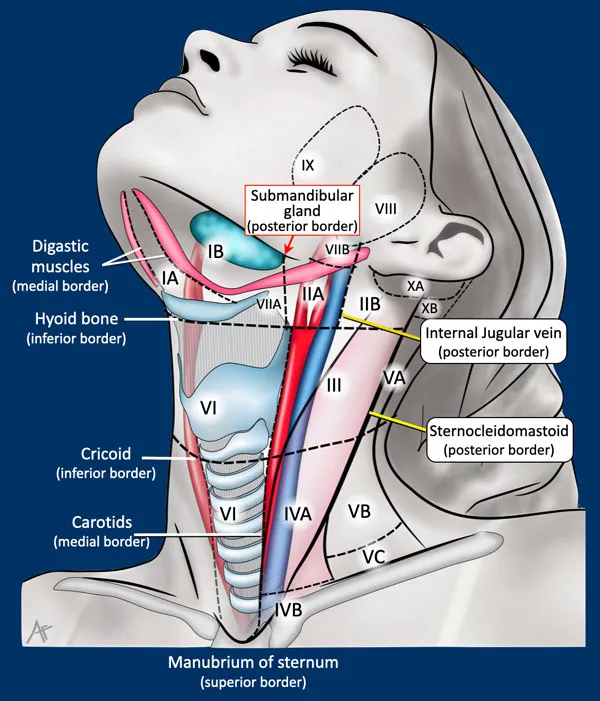
- Neck Examination (Lymph Nodes):
- Inspect: scars, sinuses, swellings, visible pulsations.
- Palpate systematically: submental, submandibular, jugulodigastric, cervical (anterior/posterior chains), supraclavicular.
- Note: 📌 Site, Size (cm), Shape, Surface, Skin changes, Consistency (e.g. matted), Tenderness, Mobility (fixed?).
⭐ Jugulodigastric node (Level II) is often called the "tonsillar node" as it's the primary drainage for the palatine tonsil.
High‑Yield Points - ⚡ Biggest Takeaways
- Tuning fork tests (Rinne, Weber) are crucial to differentiate CHL vs. SNHL.
- Otoscopy: Identify landmarks like malleus handle, umbo, and cone of light.
- Anterior rhinoscopy for nasal cavity; posterior mirror exam for nasopharynx.
- Indirect Laryngoscopy (IDL) for vocal cords; tonsil grading (Brodsky scale).
- Systematic neck palpation of lymph node levels is vital for staging.
- Assess key ENT cranial nerves (V, VII, VIII, IX, X, XI, XII) for deficits.
- Cold caloric test (COWS) evaluates vestibular function (horizontal SCC).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more