Oral Cavity - Entry Essentials
- Definition: Extends from lips (cutaneous-vermilion junction) to palatoglossal arches.
- Boundaries:
- Anterior: Lips (orbicularis oris m.).
- Posterior: Palatoglossal arches (anterior tonsillar pillars).
- Superior: Hard palate (bony anterior 2/3), Soft palate (muscular posterior 1/3).
- Inferior: Floor of mouth (mylohyoid m.), tongue.
- Lateral: Cheeks (buccinator m.).
- Subdivisions:
- Vestibule: Between lips/cheeks and teeth/gingivae.
- Parotid (Stensen's) duct opens opposite upper 2nd molar.
- Oral Cavity Proper: Space internal to dental arches.
- Contents: Tongue, teeth, gingivae.
- Ducts: Wharton's (submandibular) at sublingual caruncle; Rivinus' (sublingual) on sublingual fold.
- Vestibule: Between lips/cheeks and teeth/gingivae.
- Lining: Stratified squamous epithelium (non-keratinized; keratinized on hard palate, tongue dorsum, gingiva).

⭐ Stensen's duct (parotid) opens into vestibule opposite maxillary 2nd molar; a key landmark.
Tongue & Salivary Glands - Taste & Moisten
- Tongue: Muscular organ for taste, speech, mastication, deglutition.
- Parts: Oral (ant. 2/3), Pharyngeal (post. 1/3); separated by sulcus terminalis.
- Muscles:
- Intrinsic: Alter shape.
- Extrinsic: Alter position (Genioglossus, Hyoglossus, Styloglossus, Palatoglossus). 📌 Mnemonic: Good Hygienic Students Practice.
- Innervation (Motor): CN XII (Hypoglossal) to all except Palatoglossus (CN X - Vagus).
- Innervation (Sensory):
- Ant. 2/3: General - Lingual (V3); Taste - Chorda Tympani (VII).
- Post. 1/3: General & Taste - CN IX (Glossopharyngeal).
- Root/Epiglottis: CN X (Vagus).
- Papillae: Filiform (touch, no taste), Fungiform (taste), Foliate (taste), Circumvallate (taste, Von Ebner's glands).

- Salivary Glands: Produce saliva (~1-1.5 L/day).
- Major Glands:
- Parotid: Serous. Stensen's duct. CN IX (parasymp).
- Submandibular: Mixed (serous > mucous). Wharton's duct. CN VII (parasymp).
- Sublingual: Mixed (mucous > serous). Ducts of Rivinus/Bartholin's. CN VII (parasymp).
- Minor Glands: Scattered, mainly mucous. Von Ebner's (serous, associated with circumvallate papillae).
- Functions: Lubrication, digestion (amylase), immunity (IgA), taste.
- Major Glands:
⭐ Frey's Syndrome: Post-parotidectomy gustatory sweating/flushing due to aberrant CN IX nerve regeneration to sweat glands over the parotid area.
Pharynx - The Crossroads
- Location & Extent: Musculomembranous tube (12-14 cm); base of skull to C6 (inferior border of cricoid).
- Subdivisions:
- Nasopharynx: Skull base to soft palate.
- Contents: Adenoids (pharyngeal tonsil), Eustachian tube opening, Fossa of Rosenmüller.
- Epithelium: Ciliated columnar.
- Oropharynx: Soft palate to hyoid/epiglottis.
- Contents: Palatine tonsils, lingual tonsil.
- Waldeyer's Lymphatic Ring: Pharyngeal (adenoids), tubal, palatine, & lingual tonsils. 📌 (P.T.P.L.)
- Epithelium: Non-keratinized stratified squamous.
- Laryngopharynx (Hypopharynx): Hyoid/epiglottis to C6.
- Contents: Piriform fossae, postcricoid region.
- Epithelium: Non-keratinized stratified squamous.
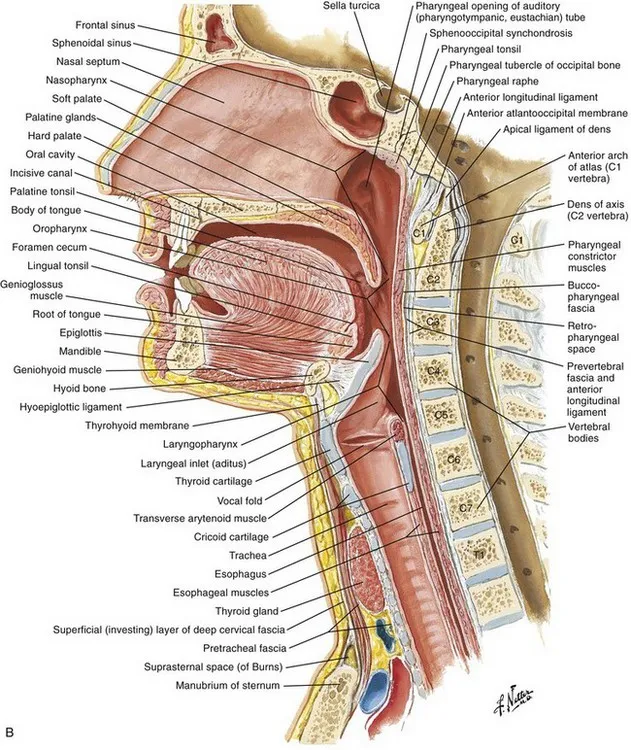
- Nasopharynx: Skull base to soft palate.
- Muscles:
- Outer Circular (Constrictors): Superior, Middle, Inferior. Propel bolus.
- Killian's Dehiscence: Weakness between thyropharyngeus & cricopharyngeus (inferior constrictor); site of Zenker's diverticulum.
- Inner Longitudinal: Stylopharyngeus, Salpingopharyngeus, Palatopharyngeus. Elevate pharynx/larynx.
- Outer Circular (Constrictors): Superior, Middle, Inferior. Propel bolus.
- Innervation:
- Motor:
- Most muscles: Pharyngeal plexus (CN X, cranial root of CN XI).
- Stylopharyngeus: Exclusively CN IX.
- Sensory: Nasopharynx (CN V2), Oropharynx (CN IX), Laryngopharynx (CN X - internal laryngeal n.).
⭐ The stylopharyngeus is the only muscle innervated by the glossopharyngeal nerve (CN IX).
- Motor:
- Oral cavity proper: Bounded by teeth/alveolar arches, palate, floor of mouth muscles.
- Waldeyer's ring: Lymphoid tissue: pharyngeal, tubal, palatine, lingual tonsils.
- Tongue motor: CN XII (not palatoglossus: CN X). Sensory: Ant 2/3rd Lingual (V3), Chorda tympani (VII); Post 1/3rd CN IX.
- Pharynx: Nasopharynx (Eustachian tube), Oropharynx (palatine tonsils), Laryngopharynx (to cricoid).
- Killian's dehiscence: Inferior constrictor weak spot for Zenker's diverticulum.
- Palatine tonsil artery: Mainly tonsillar branch of facial artery.
- Retropharyngeal space: Infection can spread to mediastinum.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

