External Nose & Nasal Cavity - Sniffer's Structure
-
External Nose:
- Framework: Bony (nasal bones, frontal process of maxilla) & Cartilaginous (septal, lateral, alar cartilages).
- Skin: Thin over bony part, thicker with sebaceous glands over cartilaginous part.
- Muscles: Procerus, nasalis, depressor septi.
-
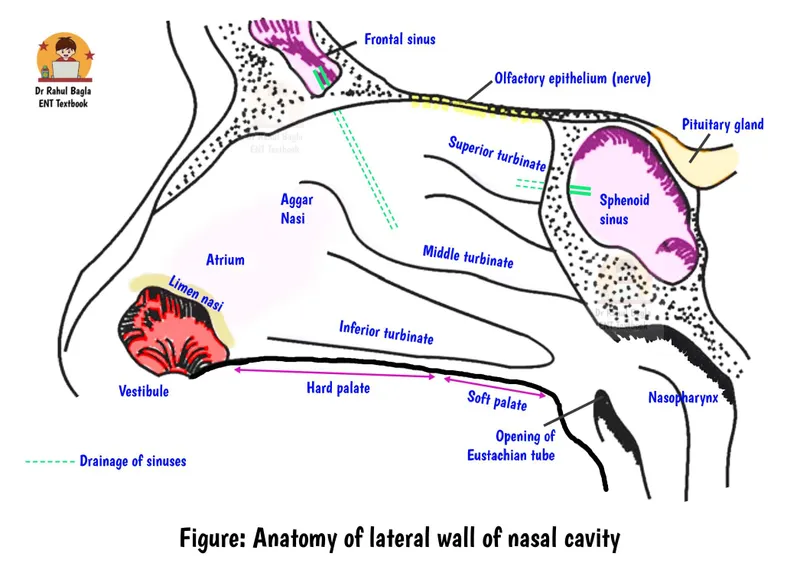
Nasal Cavity: Extends from nostrils (nares) to choanae.
- Vestibule: Lined by skin, contains vibrissae.
- Nasal Septum: Midline partition (cartilage, vomer, perpendicular plate of ethmoid).
- Lateral Wall: Features conchae (turbinates) - superior, middle, inferior; and meatuses below each.
- Inferior meatus: Nasolacrimal duct opens.
- Middle meatus: Openings for maxillary, frontal, anterior ethmoidal sinuses (osteomeatal complex).
- Superior meatus: Posterior ethmoidal sinus opening.
- Sphenoethmoidal recess: Sphenoidal sinus opening.
⭐ Kiesselbach's Plexus (Little's Area): Located in the anteroinferior part of the nasal septum, it is the most common site for epistaxis (nosebleeds).
Paranasal Sinuses - Hollow Headspaces

- Air-filled cavities in skull bones, lined by ciliated pseudostratified columnar (respiratory) mucosa. Four pairs:
- Frontal (forehead)
- Ethmoidal (between eyes; Anterior, Middle, Posterior groups)
- Maxillary (cheeks; largest, first to develop)
- Sphenoidal (deep, behind nose)
- Functions: Lighten skull, voice resonance, warm & humidify inspired air, mucus production, immune defense.
- 📌 Mnemonic (Sinuses): For Every Medical Student (Frontal, Ethmoidal, Maxillary, Sphenoidal).
⭐ The Maxillary sinus is the largest paranasal sinus, the first to develop (rudimentary at birth), and the most frequently infected (sinusitis). Its ostium is high on the medial wall, predisposing to stasis.
Drainage Pathways:
Nasal Vasculature & Innervation - Life Support Lines
- Arterial Supply: Dual origin (ECA & ICA).
- ECA branches: Sphenopalatine a. (main), Greater Palatine a., Superior Labial a.
- ICA branches: Anterior & Posterior Ethmoidal arteries (from Ophthalmic a.).
- Epistaxis Sites:
- Kiesselbach's Plexus (Little's Area): Anteroinferior septum. AEA, SPA, GPA, SLA. Commonest anterior site. 📌 Kids Love All Sweets.
- Woodruff's Plexus: Posteriorly; for posterior epistaxis.
- Innervation:
- General Sensory: CN V: V1 (Ant. Ethmoidal n.) & V2 (Nasopalatine n., SPG branches).
- Special Sense (Smell): CN I (Olfactory n.).
- Autonomic (via Vidian n. to Sphenopalatine Ganglion - SPG):
- Parasympathetic (CN VII origin): Secretomotor.
- Sympathetic (Carotid plexus origin): Vasoconstrictor.
⭐ Sphenopalatine artery (SPA) ligation is key for intractable posterior epistaxis.
Clinical Hotspots & Lymphatics - Trouble Zones & Drains
-
Epistaxis Hotspots:
- Little's Area (Kiesselbach's Plexus): Common anterior bleeds. Arteries: Ant. ethmoidal, sphenopalatine, greater palatine, sup. labial. 📌 Lazy Sheep Graze Slowly Always (Little's, Sphenopalatine, Greater palatine, Superior labial, Anterior ethmoidal).
- Woodruff's Plexus: Posterior bleeds, often severe.
-
Sinusitis Trouble Zones:
- Osteomeatal Complex (OMC): Key drainage for frontal, maxillary, ant. ethmoid sinuses. Obstruction → CRS.
- Sphenoethmoidal Recess: Drains post. ethmoid, sphenoid sinuses.
-
Danger Area:
- "Danger Triangle" of face: Infections can spread to cavernous sinus via ophthalmic veins.
-
Lymphatic Drainage:
- Anterior structures → Submandibular nodes.
- Posterior structures → Retropharyngeal & Upper deep cervical nodes.
⭐ Nasopharyngeal carcinoma (NPC) often presents early with painless, firm cervical lymphadenopathy, classically involving the Node of Rouviere (highest retropharyngeal node).
High‑Yield Points - ⚡ Biggest Takeaways
- Kiesselbach's plexus (Little's area): most common site for anterior epistaxis.
- Woodruff's plexus: important for posterior epistaxis.
- Middle meatus drains frontal, maxillary, anterior ethmoidal sinuses (via OMC).
- Superior meatus drains posterior ethmoidal sinuses; sphenoethmoidal recess drains sphenoid sinus.
- Inferior meatus receives drainage from the nasolacrimal duct.
- Sphenopalatine artery: main blood supply; CN I for smell.
- Maxillary sinus: largest, first to develop. Frontal sinus: related to anterior cranial fossa.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

