Pathophysiology & Basics - Inner Ear Tsunami
- Definition: Idiopathic inner ear disorder; key pathology: endolymphatic hydrops.
- Epidemiology: Peak onset 40-60 yrs. Prevalence ~190/100,000.
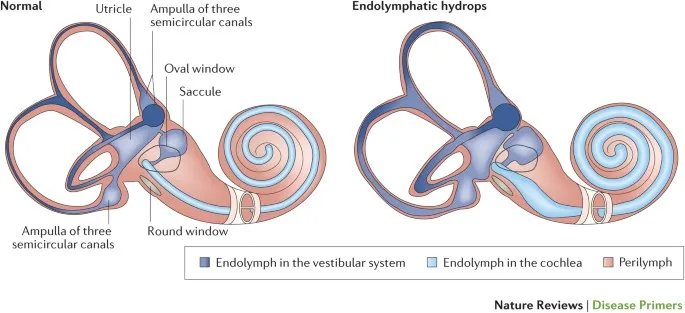
- Pathophysiology: Endolymphatic Hydrops
- ↑ endolymph volume/pressure in membranous labyrinth.
- Cause: Impaired endolymph resorption (e.g., endolymphatic sac dysfunction) or ↑ production.
- Mechanism: Distension & rupture of Reissner's membrane → K⁺-rich endolymph mixes with perilymph → hair cell dysfunction.
⭐ Rupture of Reissner's membrane is thought to cause acute vertiginous attacks.
Clinical Features & Diagnosis - Dizzying Diagnosis
-
Core Symptoms (Often Unilateral):
- Episodic vertigo: Spontaneous, rotational, lasting 20 minutes to 12 hours; often accompanied by nausea/vomiting.
- Sensorineural Hearing Loss (SNHL): Fluctuating, initially affecting low frequencies, and progressive over time.
- Tinnitus: Typically low-pitched, roaring, or hissing; intensity may worsen during or before attacks.
- Aural fullness/pressure: Sensation of blockage or pressure in the affected ear.
- Attacks often occur in clusters. Lermoyez phenomenon (rare; hearing transiently improves before vertigo) or Tumarkin otolithic crisis (drop attacks without loss of consciousness; late-stage, uncommon) can occur.
-
Diagnosis (AAO-HNS 2015 Criteria for "Definite Ménière's Disease"):
- Requires all four criteria: 1. Two or more spontaneous vertigo episodes (each 20 minutes to 12 hours), 2. Audiometrically documented low- to medium-frequency SNHL in the affected ear, 3. Fluctuating aural symptoms (hearing, tinnitus, or fullness) in the affected ear, 4. Not better accounted for by another vestibular diagnosis.
-
Key Investigations:
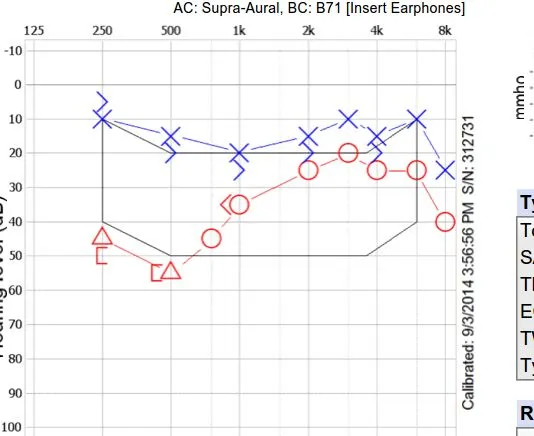
- Pure Tone Audiometry (PTA): Shows low-frequency or combined low & high-frequency SNHL, often with a rising pattern in early stages; later becomes flat.
- Electrocochleography (ECoG): May show an increased SP/AP (Summating Potential/Action Potential) ratio > 0.4, suggestive of endolymphatic hydrops.
- MRI Brain (with Gadolinium): Essential to rule out retrocochlear pathology (e.g., vestibular schwannoma, multiple sclerosis).
- Vestibular Evoked Myogenic Potentials (VEMP): Cervical VEMP (cVEMP) may show reduced amplitude or increased threshold on the affected side.
- Pure Tone Audiometry (PTA): Shows low-frequency or combined low & high-frequency SNHL, often with a rising pattern in early stages; later becomes flat.
-
⭐ > The Glycerol dehydration test, though less commonly performed now due to variability, can be positive (transient improvement in hearing or tinnitus after glycerol ingestion). Historically, this supported the diagnosis by demonstrating osmotic fluid shifts in the inner ear and is an exam favourite concept.
Treatment - Calming the Current
- Lifestyle Modifications:
- Low salt diet (target <1.5-2 g/day Na⁺)
- Avoid triggers: caffeine, alcohol, nicotine, stress
- Acute Attack Management:
- Vestibular suppressants: Antihistamines (e.g., promethazine), Benzodiazepines (e.g., diazepam - short-term)
- Antiemetics (e.g., ondansetron)
- Prophylactic Medical Therapy:
- Diuretics (e.g., Hydrochlorothiazide + Triamterene)
- Betahistine (16-48 mg TID)
- Oral corticosteroids (short course for severe flares)
- Intratympanic Therapy (for refractory vertigo):
- IT Gentamicin: Chemical labyrinthectomy (ablative). Concentration ~30-40 mg/mL, low dose, titrated. ⚠️ Risk of hearing loss.
- IT Steroids (e.g., Dexamethasone): Non-ablative, anti-inflammatory.
- Surgical Interventions (disabling vertigo, failed prior therapies):
- Hearing Preservation Attempt (Non-Destructive):
- Endolymphatic Sac Surgery (ELS) - variable efficacy.
- Ablative (Destructive):
- Labyrinthectomy (results in anacusis in treated ear).
- Vestibular Nerve Section (VNS) - aims for vertigo control, potential hearing preservation.
- Hearing Preservation Attempt (Non-Destructive):
⭐ Intratympanic gentamicin is an effective ablative therapy for refractory Ménière's disease, but carries a significant risk of iatrogenic sensorineural hearing loss.
High‑Yield Points - ⚡ Biggest Takeaways
- Triad: episodic vertigo (20 min - 12 hr), tinnitus, fluctuating low-frequency SNHL.
- Pathophysiology: endolymphatic hydrops (excess endolymph in inner ear).
- Hearing loss: initially low-frequency SNHL, can become permanent, affecting all frequencies.
- Aural fullness or pressure in the affected ear is characteristic.
- Diagnosis: clinical (AAO-HNS criteria); ECoG (SP/AP > 0.4) supports.
- Acute attacks: vestibular suppressants (diazepam), antiemetics.
- Long-term: low-salt diet, diuretics, betahistine; intratympanic gentamicin for refractory vertigo_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more