Thyroid Nodule Basics - Lump Sum Assessment
- Solitary Thyroid Nodule (STN): Common; prevalence ↑ with age. Most are benign.
- Malignancy Risk Factors:
- Age < 30 or > 60 yrs
- Childhood head/neck radiation
- Family Hx (thyroid Ca, MEN2)
- Rapid growth, hoarseness
- Initial Workup:
- History & Physical Exam: Note size, consistency, mobility, lymph nodes.
- Serum TSH: Initial biochemical test.
⭐ Most thyroid nodules are benign, but all require systematic evaluation.
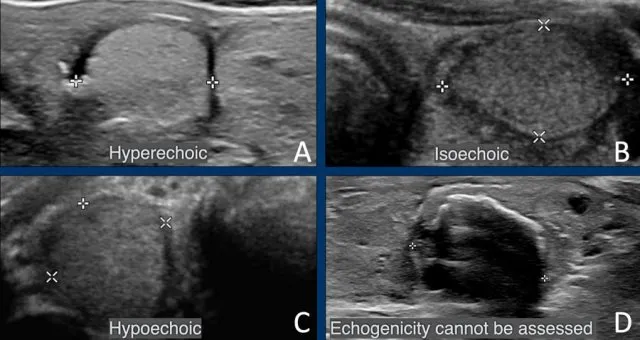
Nodule Sonography & Cytology - Pixel & Prick Pointers
Thyroid USG: Risk stratifies nodules. High-risk features: microcalcifications, marked hypoechogenicity, irregular margins, taller-than-wide, extrathyroidal extension, suspicious nodes. ACR TI-RADS (TR1-TR5) score guides FNAC.
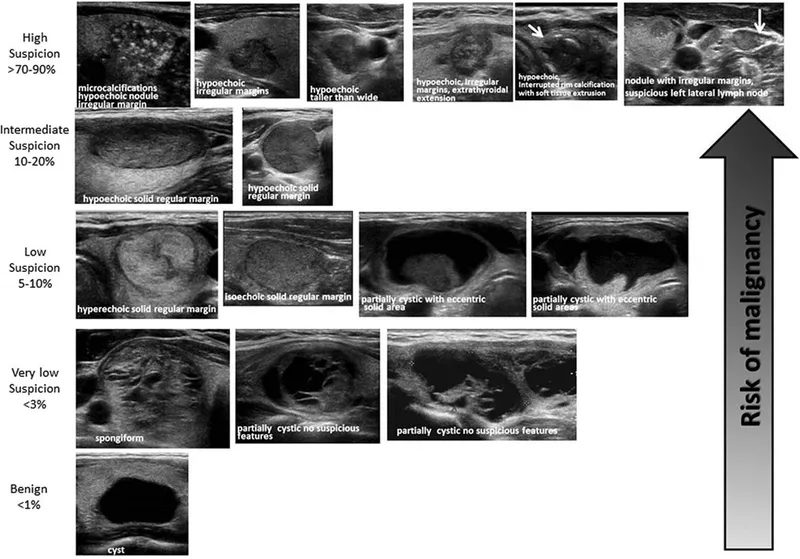
Fine Needle Aspiration Cytology (FNAC):
- Indicated for suspicious nodules (e.g., TI-RADS ≥TR3 or high-risk USG features).
- Usually USG-guided biopsy.
⭐ FNAC is the gold standard for pre-operative differentiation of benign vs. malignant thyroid nodules.
Bethesda System for Reporting Thyroid Cytopathology (BSRTC): Reports cytopathology, Risk of Malignancy (ROM) & guides management.
- I: Non-diagnostic (ROM ~10%)
- II: Benign (ROM <3%)
- III: AUS/FLUS (ROM ~20%)
- IV: Follicular Neoplasm/Suspicious (ROM ~30%)
- V: Suspicious for Malignancy (ROM ~65%)
- VI: Malignant (ROM ~99%)
Benign Nodule Management - Watchful Waiting Wins
- Follow-up (Bethesda II): USG surveillance; repeat 6-24 months, then less frequently if stable.
- Surgery indications:
- Compressive symptoms.
- Cosmetic concerns.
- Patient preference.
- Suspicious growth (>20% 2D / >50% vol).
- Substernal extension.
- TSH Suppression: Limited role, not routine.
⭐ Asymptomatic, cytologically benign thyroid nodules (Bethesda II) are typically managed with serial ultrasound surveillance.
Thyroid Cancers Unmasked - Malignancy Map
- Differentiated Thyroid Cancers (DTC):
- Papillary (PTC): Most common (~80%). Psammoma bodies, Orphan Annie eye nuclei. BRAF, RET/PTC. Lymphatic spread.
- Follicular (FTC): ~10-15%. Capsular/vascular invasion defines malignancy. Hematogenous spread. RAS, PAX8-PPARγ.
- Hürthle Cell: FTC variant, more aggressive.
- Medullary (MTC): ~5%. From C-cells. ↑ Calcitonin, ↑ CEA. MEN2A/2B (RET mutations).
- Anaplastic (ATC): <2%. Aggressive, elderly, dismal prognosis. TP53.
- Lymphoma: Rare, associated with Hashimoto’s thyroiditis.
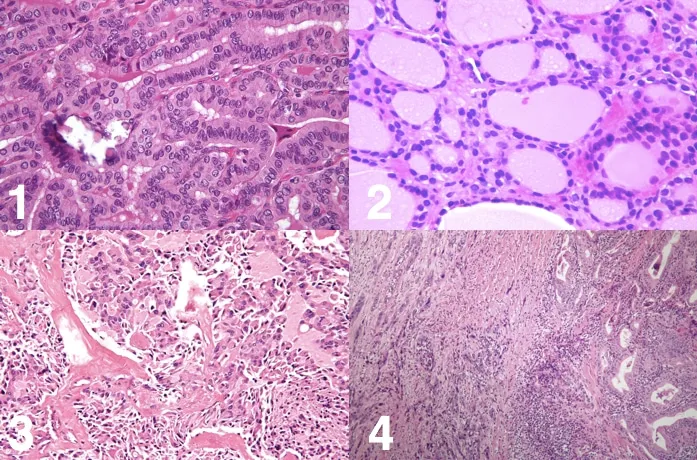
- TNM Staging (AJCC 8th Ed - DTC): Key: T, N, M. Age (<55 yrs better prognosis) crucial.
⭐ Papillary thyroid carcinoma is the most common endocrine malignancy and often presents with cervical lymph node metastasis (📌 'Popular' cancer spreads to 'Popular' places - lymph nodes).
Cancer Combat Strategies - Treatment Tactics
- Surgery: Lobectomy or Total Thyroidectomy. Prophylactic CND (high-risk). Therapeutic Neck Dissection (nodal mets).
- Radioactive Iodine (RAI): For remnant ablation, adjuvant, or metastatic disease.
- TSH Suppression: Levothyroxine; target TSH usually <0.1-0.5 mU/L.
- EBRT/TKIs: For advanced, unresectable, or RAI-refractory (Lenvatinib, Sorafenib).
- Follow-up: Tg, Anti-Tg Ab, Neck USG, diagnostic RAI scan.
⭐ Serum Thyroglobulin (Tg) and anti-Tg antibodies are essential for monitoring recurrence in differentiated thyroid cancer post-thyroidectomy and RAI ablation.
High‑Yield Points - ⚡ Biggest Takeaways
- Papillary Thyroid Carcinoma (PTC) is the most common type; look for Orphan Annie eye nuclei and psammoma bodies.
- Medullary Thyroid Carcinoma (MTC) from C-cells secretes calcitonin; associated with MEN2/RET.
- Anaplastic carcinoma is highly aggressive, typically in the elderly with a dismal prognosis.
- Follicular carcinoma spreads hematogenously; capsular/vascular invasion is key for diagnosis.
- Fine Needle Aspiration (FNA) biopsy is the gold standard for evaluating suspicious thyroid nodules.
- Initial nodule workup includes TSH and thyroid ultrasound; cold nodules on scintigraphy are more suspicious for malignancy.
- Bethesda system is crucial for reporting thyroid cytopathology results from FNA.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

