Neck Spaces and Fasciae - Neck's Scaffolding
- Superficial Cervical Fascia: Lies deep to skin. Contains: platysma, cutaneous nerves, vessels, lymphatics.
⭐ Platysma: key muscle in superficial fascia; innervated by cervical branch of Facial N. (CN VII).
- Deep Cervical Fascia (DCF): Compartmentalizes neck; limits infection spread. Consists of:
- Investing Layer: Encloses Sternocleidomastoid (SCM) & Trapezius.
- Pretracheal Layer: Encloses thyroid, trachea, esophagus; infrahyoid muscles.
- Prevertebral Layer: Surrounds vertebrae & deep neck muscles (e.g., scalenes).
- Carotid Sheath: Formed by all 3 layers. Contents: Common/Internal Carotid Artery, Internal Jugular Vein (IJV), Vagus N. (CN X).
- Neck Spaces: Potential infection pathways.
- Retropharyngeal space: "Danger space" allows infection spread to mediastinum.
- Other key spaces: Prevertebral, Parapharyngeal, Submandibular. 侵
Neck Spaces and Fasciae - Compartment Creators
The Deep Cervical Fascia (DCF) organizes neck structures into compartments, influencing pathways for infection spread.
- Investing Layer:
- Outermost layer; completely encircles the neck like a collar.
- Splits to enclose: Sternocleidomastoid (SCM) & Trapezius muscles.
- Also encloses: Submandibular & Parotid glands.
- Pretracheal Layer: (Anterior neck, limited to region between hyoid and thorax)
- Muscular part: Encloses infrahyoid muscles.
- Visceral part: Encloses thyroid gland, trachea, esophagus.
- Buccopharyngeal fascia: Posteriorly, covers pharynx & esophagus.
- Prevertebral Layer: (Posterior to pharynx/esophagus, anterior to vertebral column)
- Covers prevertebral muscles & vertebral column.
- Forms floor of the posterior triangle of the neck.
- Extends laterally as the axillary sheath.
- Carotid Sheath:
- Tubular fascial condensation around the major neurovascular bundle.
- Formed by contributions from investing, pretracheal, and prevertebral layers.
⭐ Contents: Common/Internal Carotid Artery (CCA/ICA - medial), Internal Jugular Vein (IJV - lateral), Vagus Nerve (CN X - posterior). (📌 Mnemonic: "VAN" - Vein, Artery, Nerve, from medial to lateral in superior part, or generally Vagus is posterior)
Neck Spaces and Fasciae - Infection Highways
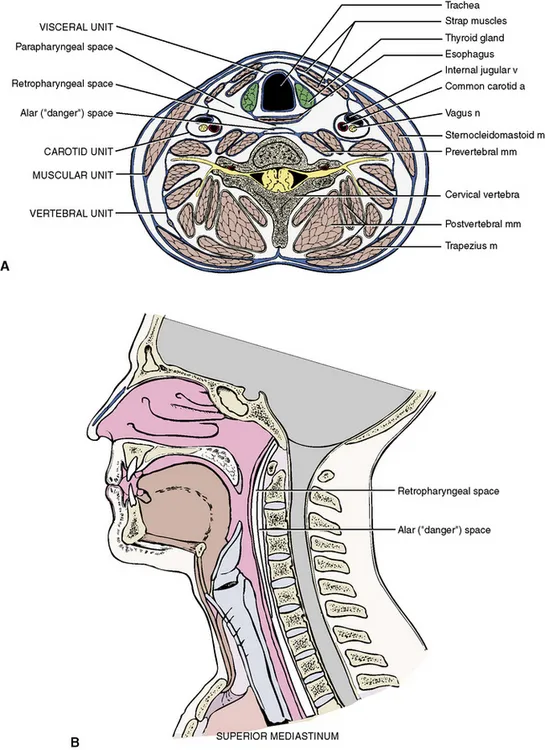
- Deep Cervical Fascia (DCF) layers (Investing, Pretracheal, Prevertebral - 📌 3 P's) delineate key potential spaces.
- Key True Neck Spaces & Infection Spread:
- Pretracheal Space: Hyoid to superior mediastinum. Infection → anterior mediastinum.
- Retropharyngeal Space (RPS): Skull base to T1-T2. Between buccopharyngeal & alar fascia. Common for pharyngeal abscess.
- Danger Space (Space 4): Between alar & prevertebral fascia.
⭐ Extends from skull base to diaphragm. Infections (e.g., from RPS) can rapidly cause life-threatening posterior mediastinitis.
- Prevertebral Space: Skull base to coccyx. Posterior to danger space. Vertebral infections (e.g., Pott's) spread here.
- Carotid Sheath: Contains carotid artery, IJV, vagus (CN X). Conduit for infection spread.

Neck Spaces and Fasciae - Clinical Hotspots

- Parapharyngeal Space (PPS):
- Lateral pharyngeal; extends from skull base to hyoid bone.
- Divisions: Prestyloid (fat, nodes, CN V3 branches) & Poststyloid (carotid artery, IJV, CN IX, X, XI, XII, sympathetic chain).
- Infection sources: dental, tonsillar, pharyngeal. Risks: airway obstruction, vascular spread (e.g., Lemierre's syndrome).
- Submandibular & Sublingual Spaces:
- Mylohyoid muscle is key divider.
- Submandibular (inferior to mylohyoid): contains submandibular gland, lymph nodes. Infection commonly from mandibular molars.
- Sublingual (superior to mylohyoid): contains sublingual gland, Wharton's duct.
- Ludwig's Angina:
- Aggressive, bilateral cellulitis of submandibular, sublingual, and submental spaces.
- Symptoms: "woody" or brawny induration of neck/floor of mouth, tongue elevation, drooling.
- ⚠️ High risk of rapid airway obstruction; requires urgent management.
⭐ Ludwig's angina most commonly arises from odontogenic infections (especially mandibular 2nd or 3rd molars) and poses a significant, rapid threat to airway patency due to posterior displacement of the tongue and laryngeal edema.
High‑Yield Points - ⚡ Biggest Takeaways
- Investing layer of deep fascia encloses SCM and Trapezius.
- Pretracheal fascia encloses thyroid, trachea, esophagus (visceral compartment).
- Prevertebral fascia covers vertebral muscles; alar fascia separates retropharyngeal from danger space.
- Carotid sheath contains CCA, IJV, and Vagus nerve (CN X).
- Retropharyngeal space infections (anterior to alar) spread to superior mediastinum.
- Danger space infections (posterior to alar) spread to posterior mediastinum (diaphragm).
- Ludwig's angina: cellulitis of submandibular, sublingual, submental spaces; critical airway risk.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

