Anatomy & Etiology - Nerve Nuances
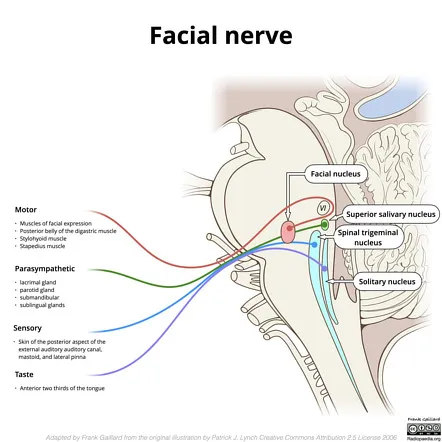
- Facial Nerve (CN VII): Motor, parasympathetic, sensory.
- Segments: Intracranial, Meatal, Labyrinthine, Tympanic, Mastoid, Extratemporal.
- Branches: GSPN, N. to Stapedius, Chorda Tympani. Extratemporal: Temporal, Zygomatic, Buccal, Marginal Mandibular, Cervical (📌 To Zanzibar By Motor Car).
- Etiology:
- Bell's Palsy (most common).
- Trauma (Temporal bone #).
- Infections (Ramsay Hunt, Lyme).
- Tumors (Acoustic neuroma, Parotid).
⭐ Bell's Palsy is the most common cause of unilateral facial paralysis, accounting for ~70% of cases.
Clinical Evaluation - Face Facts First
- History: Onset (sudden/gradual), duration, progression. Associated: otalgia, vesicles (Zoster), hearing loss, tinnitus, vertigo, dry eyes/mouth (sicca), taste changes (dysgeusia), trauma, prior episodes.
- Examination:
- Systemic: Parotid masses, skin lesions.
- Cranial Nerves: Focus on V, VIII; also VII, IX, X, XI, XII.
- Facial Nerve Detail:
- Symmetry: At rest (e.g., nasolabial fold) and with movement (forehead wrinkle, eye closure, smile, pucker).
- Bell's phenomenon: Eye rolls up/out on attempted closure.
- Synkinesis, hemifacial spasm, contractures, crocodile tears (gustatory lacrimation).
- Grading: Quantify severity.
- House-Brackmann Scale: Standard.
⭐ House-Brackmann Grade III signifies moderately severe dysfunction with obvious, disfiguring weakness but some movement; Grade VI is total paralysis.
Investigations - Nerve Navigators
- Topodiagnostic Tests (Conceptual):
- Schirmer's, Stapedial reflex, Taste, Salivary flow.
- Electrophysiological Tests:
- ENoG (Electroneurography):
- Compares Compound Muscle Action Potential (CMAP): affected vs. normal side.
-
90% degeneration by 3 weeks (ideally ~14 days) → poor prognosis; consider surgery.
- EMG (Electromyography):
- Fibrillation potentials (denervation): after 10-21 days.
- Polyphasic potentials: reinnervation signs.
- ENoG (Electroneurography):
- Imaging: CT/MRI for suspected tumor, trauma, central cause.

⭐ ENoG showing > 90% degeneration of nerve fibres vs. normal side by 3 weeks (ideally ~14 days) post-onset is a key indicator for surgical intervention in complete paralysis (e.g., Bell's Palsy, trauma).
Management Options - Fixes & Functions
- Medical (Acute Phase):
- Eye Care: Essential! Lubricants, patching, taping. Temporary tarsorrhaphy for corneal protection.
- Steroids: Prednisolone ($1mg/kg/day$) for Bell's Palsy, start within 72h.
- Antivirals: For Ramsay Hunt; +/- severe Bell's with steroids.
- Surgical (Timing is CRUCIAL):
- Early Interventions (<3 mo, nerve viable):
- Facial Nerve Decompression (selected cases: trauma, Bell's >90% ENOG degeneration).
- Direct Neurorrhaphy (end-to-end).
- Interpositional Cable Grafts (e.g., Great Auricular, Sural for gaps).
- Nerve Transfers (Neurotization, 3-18 mo for muscle reinnervation):
- Hypoglossal-Facial (XII-VII) 📌 "Lick & Smile!"
- Masseteric-Facial (V3-VII).
- Cross-Facial Nerve Graft (CFNG).
- Late Reanimation (>1.5-2 yrs or significant muscle atrophy):
- Dynamic: Temporalis/Masseter regional muscle transfer; Gracilis free flap (smile).
- Static: Slings (fascia lata), brow lift, eyelid procedures for symmetry.
- Early Interventions (<3 mo, nerve viable):
- Synkinesis Management:
- Botulinum toxin, physiotherapy, selective neurectomy/myectomy.
⭐ Early corticosteroids (Prednisolone, within 72h) are key for Bell's Palsy recovery.

High‑Yield Points - ⚡ Biggest Takeaways
- Nerve repair/grafting is optimal within 12-18 months post-injury for functional recovery.
- House-Brackmann scale is the standard for grading facial nerve deficit severity.
- Bell's Palsy: Treat promptly with corticosteroids; prioritize corneal protection and eye care.
- Traumatic nerve transection: Demands urgent surgical exploration and microneural repair/grafting.
- Dynamic reanimation (e.g., temporalis transfer, gracilis flap) restores active facial movement.
- Static procedures (e.g., slings, tarsorrhaphy) provide support and improve resting symmetry.
- Botulinum toxin effectively manages synkinesis and reduces contralateral facial muscle overactivity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

