Facial Trauma: Assessment - Face First Aid!
- Initial Approach: Follow ATLS principles (ABCDE). Prioritize airway, C-spine, breathing, circulation.
- Airway: Critical! Assess for obstruction (blood, foreign bodies, edema). Early intubation if GCS < 8, airway compromise, or expanding hematoma.
- Hemorrhage: Control active bleeding (direct pressure, packing). Consider angiography/embolization for persistent severe bleeding.
- Examination:
- Systematic: Inspect (asymmetry, lacerations, ecchymosis), palpate (tenderness, crepitus, step-offs).
- Neurological: GCS, cranial nerves (II, III, IV, V, VI, VII).
- Ocular: Visual acuity, EOMs, diplopia, RAPD, globe integrity.
- Imaging: CT scan (non-contrast, thin-slice axial/coronal, 3D reconstruction) is gold standard.
⭐ Most common site of CSF leak in facial trauma: Cribriform plate (anterior cranial fossa).
Mandibular Fractures - Jaw Breakers United
Most common facial #2 fracture. Often multiple.
- Common Sites: 📌 Mnemonic: "Can Angry Birds Sing Melody?"
- Condyle (30-35%)
- Angle (20-25%)
- Body (20-25%)
- Symphysis/Parasymphysis (15-20%)
- Ramus (<5%)
- Coronoid process (<2%)
- Classification:
- Simple/Compound/Comminuted.
- Favorable/Unfavorable (muscle pull impact).
- Clinical Signs:
- Pain, swelling, ecchymosis.
- Malocclusion (💡 most reliable).
- Trismus, step deformity.
- Lower lip anesthesia (IAN injury).
- Bleeding from ear (condylar #).
⭐ Muscle pull dictates displacement. Elevators (masseter, temporalis, med. pterygoid) pull superiorly/medially. Depressors (mylohyoid, geniohyoid, digastric) pull inferiorly/posteriorly. Lat. pterygoid pulls condyle anteromedially.
- Management:
- Airway first.
- Closed (MMF) or Open Reduction Internal Fixation (ORIF).
Midface Fractures - Central Face Carnage
- Le Fort Fractures: Classification of complex maxillary injuries.
- 📌 Mnemonic: I = Palate floats; II = Maxilla floats (pyramidal); III = Face floats (craniofacial dysjunction).
- Le Fort I (Transverse): Horizontal; palate separation, mobile palate, malocclusion.
- Le Fort II (Pyramidal): Maxilla & nasal bones separation; mobile midface, infraorbital paresthesia, CSF rhinorrhea possible.
- Le Fort III (Craniofacial Dysjunction): Midface-cranial base separation; gross edema, 'Dish face' deformity, CSF rhinorrhea, airway compromise.
⭐ > 'Dish face' deformity is characteristic of Le Fort III fractures.
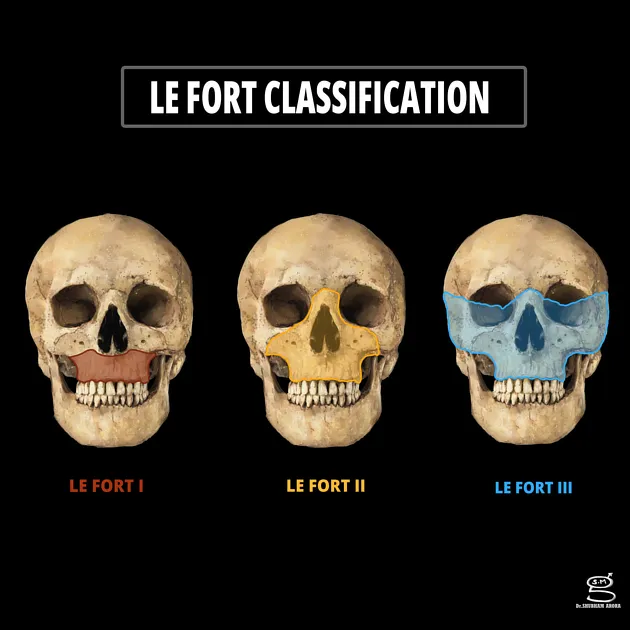
- Clinical Differentiation (Le Fort Types):
- Zygomaticomaxillary Complex (ZMC) Fracture (Tripod/Tetrapod):
- Involves: Frontozygomatic suture, zygomatic arch, infraorbital rim, zygomaticomaxillary buttress.
- Signs: Cheek flattening, diplopia, trismus, subconjunctival hemorrhage, infraorbital anesthesia.
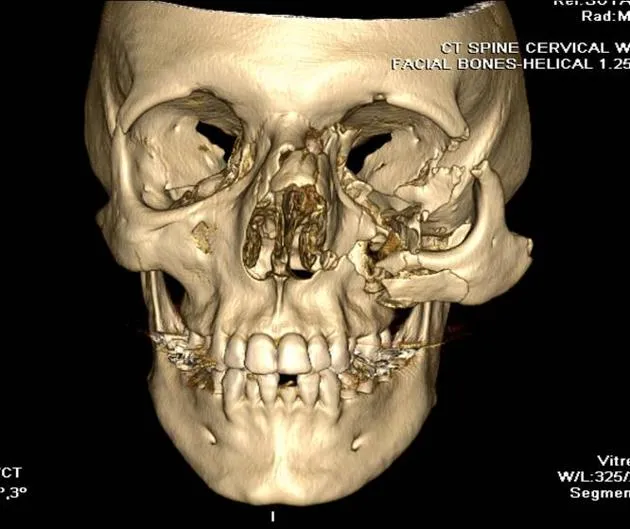 fracture components diagram)
fracture components diagram)
- Naso-Orbital-Ethmoid (NOE) Fracture:
- Signs: Traumatic telecanthus (intercanthal distance > 35mm), flattened nasal dorsum, epiphora.
- Crucial: Medial canthal tendon (MCT) integrity (Markowitz classification).
Orbito-Frontal Fractures - Eye & Brow Blows
- Orbital Fractures: Predominantly blowout or tripod types.
- Blowout Fracture: Most common; inferior wall (floor) > medial wall.
- Mechanism: Direct globe trauma → ↑intraorbital pressure.
- Signs: Diplopia (esp. upgaze), enophthalmos, infraorbital nerve anesthesia (cheek/lip numbness), restricted eye movements (muscle entrapment), periorbital ecchymosis. "Teardrop sign" on CT.
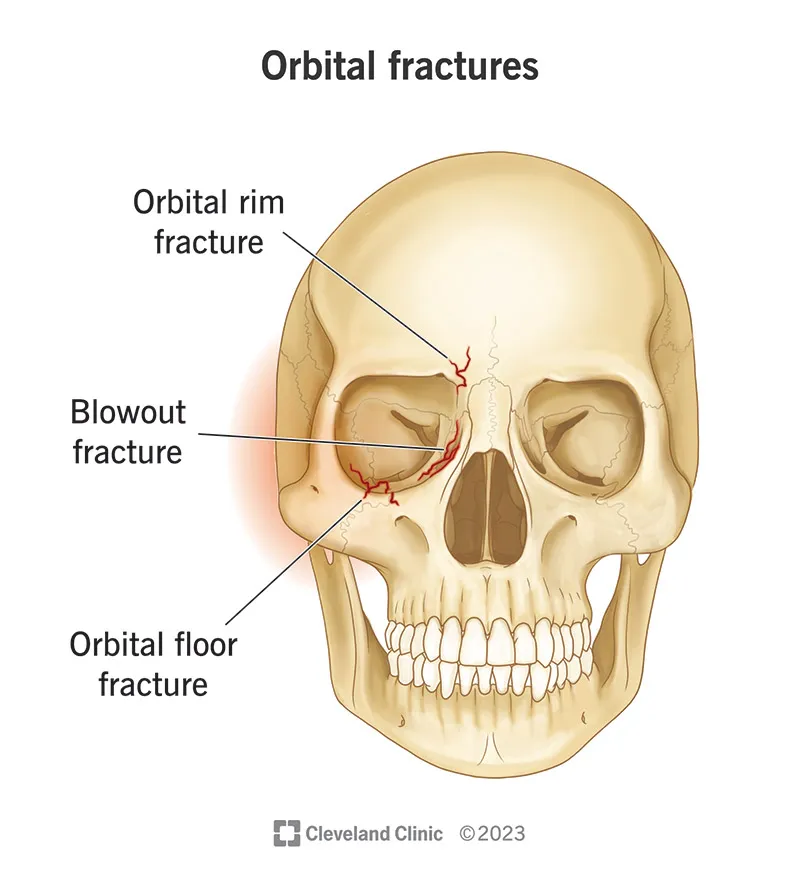
- Tripod (Zygomaticomaxillary Complex - ZMC) Fracture: Involves zygomatic arch, lateral orbital wall, inferior orbital rim, and zygomaticomaxillary buttress.
- Signs: Malar flattening, palpable step-offs, trismus, diplopia.
- Blowout Fracture: Most common; inferior wall (floor) > medial wall.
- Frontal Sinus Fractures: Classified by anterior table, posterior table, or combined involvement; nasofrontal outflow tract (NFOT) status is key.
- Anterior table: Primarily cosmetic (forehead depression).
- Posterior table: ↑Risk of CSF leak, meningitis, intracranial injury.
- NFOT injury: ↑Risk of mucocele/mucopyocele.
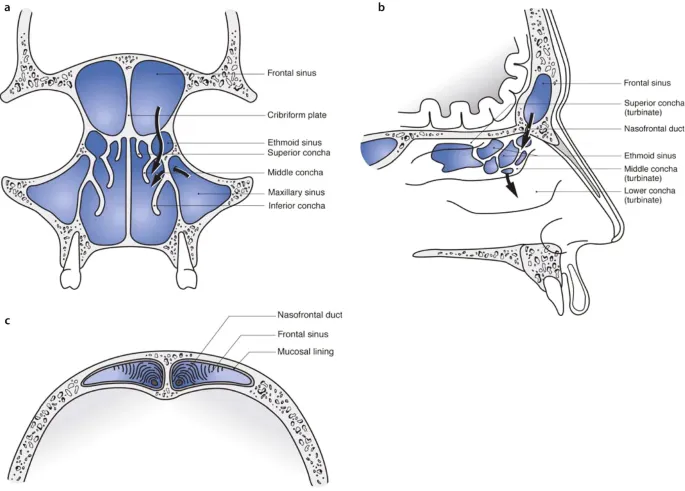
- Management: Varies by displacement, table involvement, NFOT patency, and presence of CSF leak (observation, ORIF, obliteration, cranialization).
⭐ Critical signs indicating urgent surgical intervention for orbital fractures include: persistent diplopia in primary gaze, non-resolving oculocardiac reflex (bradycardia, nausea), "white-eyed blowout" (pediatric entrapment with minimal external signs), and significant enophthalmos (>2 mm).
High‑Yield Points - ⚡ Biggest Takeaways
- Le Fort fractures: I (floating palate), II (pyramidal), III (craniofacial dysjunction); assess maxillary mobility.
- Nasal bone fractures: Most common; closed reduction within 5-7 days for best results.
- Orbital blowout fractures: Cause diplopia, enophthalmos, infraorbital anesthesia; "teardrop" sign on CT.
- Mandibular fractures: Common at condyle/angle; malocclusion is a key diagnostic sign.
- ZMC fractures (tripod): Result in cheek flattening, trismus; assess ocular motility.
- CSF rhinorrhea with skull base fractures: Confirm using β2-transferrin test.
- Airway management is the top priority in severe facial trauma.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

