Basics & Goals - Skin Deep Strategy
- Common Facial Skin Cancers:
- Basal Cell Carcinoma (BCC): Most prevalent, slow-growing.
- Squamous Cell Carcinoma (SCC): Higher metastatic potential than BCC.
- Melanoma: Most aggressive, highest mortality.
- Core Reconstructive Goals:
- Restore normal form and preserve function (e.g., eyelid, lip competence).
- Achieve optimal aesthetic outcome; minimize visible scarring.
- Protect vital underlying structures.
- Strategic Principles: 📌 R-A-L-T (RSTL, Aesthetic subunits, Like-with-like, Tension-free)
- Incisions along Relaxed Skin Tension Lines (RSTL).
- Reconstruct within facial aesthetic subunits.
- "Like replaces like": Use tissue similar in color/texture.
- Tension-free wound closure.
- Timing Considerations:
- Immediate reconstruction: Preferred for most defects post-excision.
- Delayed reconstruction: Considered for extensive tumors or after Mohs surgery to ensure clear margins.
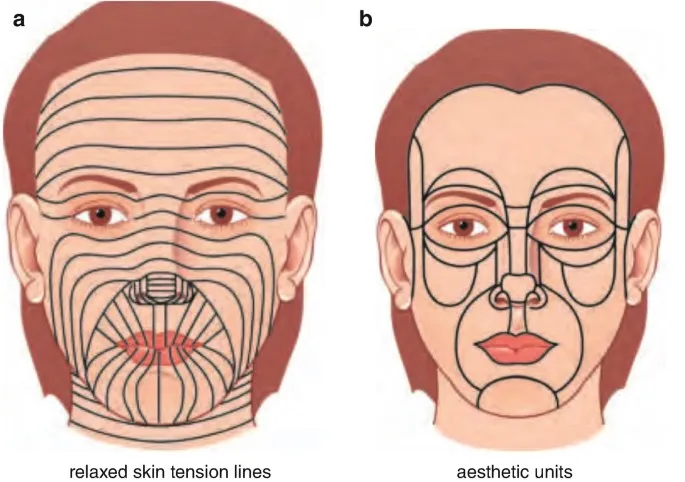
⭐ Respecting Relaxed Skin Tension Lines (RSTL) is crucial for minimizing scar visibility and achieving optimal cosmetic outcomes in facial reconstruction.
Defect Assessment & Ladder - Sizing Up Solutions
-
Defect Analysis (5 S's):
- Site: Location, aesthetic subunits (e.g., nasal ala), risk zones (H/M/L).
- Size & Shape: Dimensions (cm), geometry.
- Structures (Depth): Skin, subcutaneous, muscle, cartilage, bone.
- Surrounding Skin: Laxity, vascularity, scars, XRT changes.
- Special Factors: Functional (eyelid, lip) & cosmetic impact.
-
Reconstructive Ladder: Simple to complex.
- **Options:** Secondary intention → Primary closure → Grafts → Local flaps → Regional/Free flaps.
⭐ High-Yield: Prioritize "like-with-like" tissue replacement & respect aesthetic subunit boundaries for best facial reconstruction.
Local Flaps - Facial Fixer-Uppers
Local flaps use adjacent skin (best color/texture match) for repair. Classified by movement:
- Advancement: Slides forward (e.g., V-Y, rectangular). For small defects.
- Rotation: Pivots around a point (e.g., semicircular). For scalp, cheek.
- Transposition: Lifted over skin into defect.
- Rhomboid (Limberg): For 60°/120° defects. 📌 "Lazy S".
- Bilobed: Two lobes, often 90° apart.
- Z-plasty: Lengthens/reorients scars.
- Interpolation: Pivoted on pedicle (staged).
- Paramedian Forehead Flap (PMMF): Supratrochlear a.; for large nasal defects.
- Nasolabial: Cheek to nose/lip.
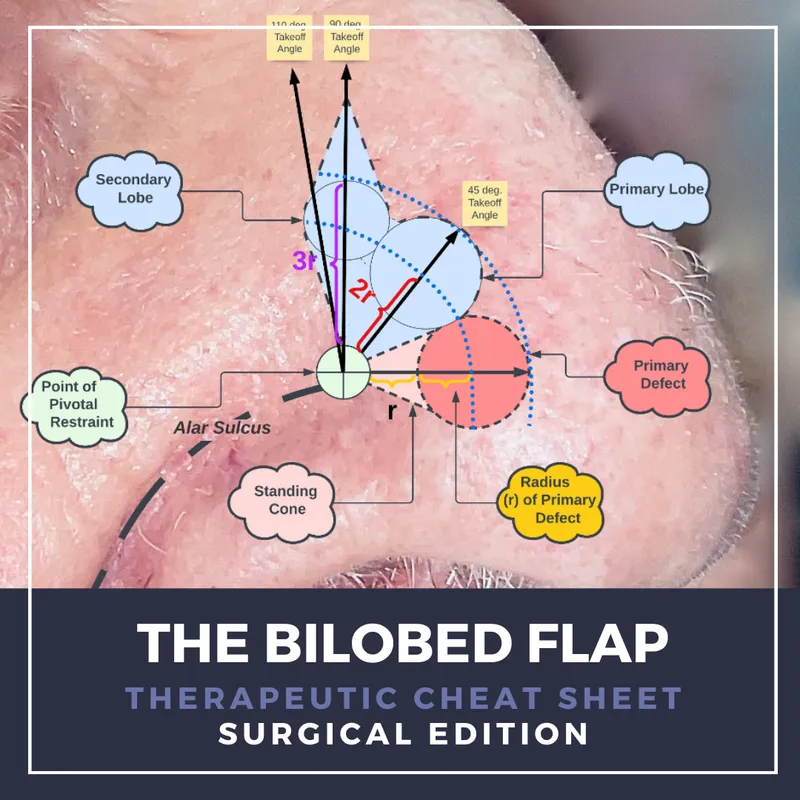
⭐ Paramedian Forehead Flap (PMMF): Axial flap (supratrochlear a.), workhorse for major nasal reconstruction (tip/ala).
Skin Grafts - Patch & Proceed
- Autologous transfer of epidermis & variable dermis; for defects unsuitable for local flaps.
- Types:
- FTSG (Full-Thickness): Epidermis + entire dermis.
- Donors: Postauricular, supraclavicular.
- Pros: ↓Contraction, better cosmesis.
- Cons: Needs good bed, limited size.
- STSG (Split-Thickness): Epidermis + partial dermis.
- Donors: Thigh, buttock (dermatome).
- Pros: Large areas, ↑take rate.
- Cons: ↑Contraction, ↓cosmesis.
- FTSG (Full-Thickness): Epidermis + entire dermis.
- Graft "Take" (Survival) Stages:
- Imbibition (Plasmatic): 0-48 hrs (adherence, nutrients).
- Inosculation: 48-72 hrs (vessel anastomosis).
- Revascularization: >72 hrs (new vessel growth).
- Failure Causes: Poor bed vascularity, infection, hematoma, shear.
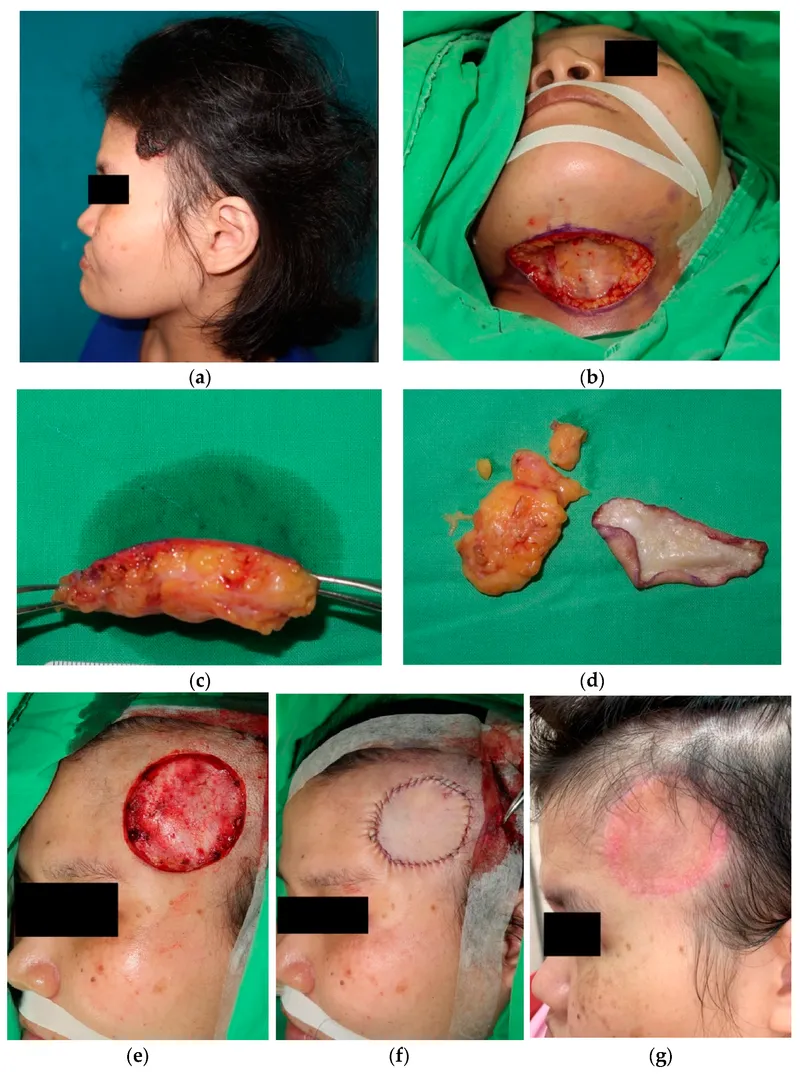
⭐ STSG donor sites heal by re-epithelialization from remaining dermal adnexal structures (hair follicles, sweat glands).
High‑Yield Points - ⚡ Biggest Takeaways
- BCC is most common; Mohs surgery for highest cure rate & tissue preservation.
- SCC has higher metastatic risk, especially in immunosuppressed or Marjolin's ulcers.
- Melanoma needs wide excision & SLNB for lesions > 0.8 mm or adverse features.
- Reconstruction uses the reconstructive ladder: direct closure, grafts, local/regional/free flaps.
- Local flaps (e.g., nasolabial, forehead) offer excellent color/texture match.
- Flap choice depends on defect size/location, tissue availability, & patient factors.
- Respecting facial aesthetic subunits is key for optimal cosmesis and scar camouflage.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

