Anatomy - Nerve Navigator
- Origin: Motor nucleus (Pons).
- Course & Segments:
- Intracranial → IAC (Meatal) → Geniculate ganglion (Labyrinthine) → Tympanic → Mastoid (second genu) → Stylomastoid foramen (Exit).
- Extratemporal Branches (Pes Anserinus in Parotid):
- Temporal (Frontalis, Orbicularis Oculi)
- Zygomatic (Orbicularis Oculi)
- Buccal (Buccinator, Orbicularis Oris)
- Marginal Mandibular (Depressor Anguli Oris)
- Cervical (Platysma)
- 📌 To Zanzibar By Motor Car
- Surgical Pointers: Tragal pointer, tympanomastoid suture.
⭐ The marginal mandibular branch is vulnerable during submandibular surgery; injury causes drooling and asymmetric smile.

Etiology & Evaluation - Droop Detectives
- Etiology:
- Most Common: Bell's Palsy (idiopathic, ?HSV)
- Infections: Ramsay Hunt (VZV), Lyme, Otitis Media (OM)
- Trauma: Temporal bone #, iatrogenic (parotid/mastoid surgery)
- Neoplasms: CPA tumors (e.g., acoustic neuroma), parotid Ca
- Congenital: Moebius syndrome
- Evaluation Protocol:
- History: Onset (sudden/gradual), associated symptoms (otalgia, vesicles, hearing).
- Exam:
- Facial Nerve Grading: House-Brackmann (HB) I-VI.
- Topodiagnostic tests (Schirmer, stapedial reflex, taste) - conceptual.
- Key Investigations:
- ENoG: If paralysis complete; >90% degeneration by 3 wks = poor prognosis (Bell's).
- EMG: Monitors reinnervation.
- Imaging (CT/MRI): For trauma, tumors, or atypical cases.

⭐ Bell's Palsy: Most frequent cause. ENoG showing >90% degeneration of facial nerve fibers compared to the normal side within 14-21 days of onset suggests a poorer prognosis and may warrant discussion of facial nerve decompression in select cases.
Timing & Goals - Timing is Key
Timing dictates reanimation strategy. Goals: restore symmetry (static/dynamic), function (smile, eye closure), corneal protection.
⭐ Denervation >2 years: motor end plates usually non-viable. Muscle transfers (temporalis, gracilis) preferred over nerve repairs.
Dynamic Techniques - Motion Makers
- Nerve Transfers (Neurotization): Restore neural input to facial muscles.
- Hypoglossal-Facial (XII-VII): Strong; risk of tongue morbidity.
- Masseteric-Facial (V3-VII): Smile with clenching.
- Cross-Facial Nerve Graft (CFNG): Sural nerve graft from normal side; often for two-stage procedures.
- Regional Muscle Transfers: Transpose local masticatory muscles.
- Temporalis Muscle Transfer: For smile, eye closure.
- Masseter Muscle Transfer: For smile.
- Free Muscle Flap: Vascularized muscle transfer.
- Gracilis Muscle: Common for smile; innervated by CFNG or masseteric nerve.
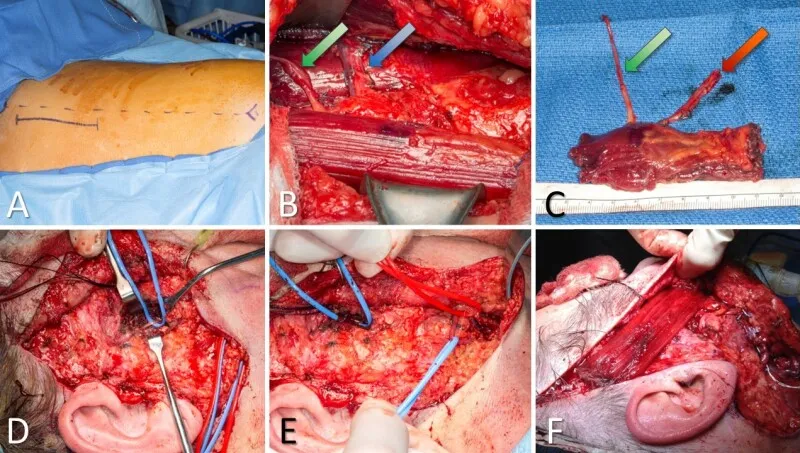
⭐ The gracilis free muscle flap, often innervated by a cross-facial nerve graft (CFNG) or masseteric nerve, is a gold standard for achieving spontaneous smile in long-standing facial paralysis.
Static & Adjunctive - Support Systems
- Static Procedures (Support at Rest)
- Goal: Facial symmetry, no active movement.
- Slings: Fascia lata (autograft), allografts, synthetic (e.g., Gore-Tex) for nasolabial fold, oral commissure.
- Ocular Care:
- Tarsorrhaphy (lateral/medial): Reduces palpebral fissure.
- Gold/platinum eyelid weights: Aid closure.
- Lower lid tightening (canthopexy/plasty).
- Other: Brow lift, facelift, cheiloplasty.
- Adjunctive Therapies (Manage Sequelae/Complement)
- Botulinum Toxin (BoNT):
- Reduces contralateral hyperactivity.
- Manages synkinesis (e.g., oral-ocular).
⭐ BoNT is first-line for post-paralytic facial synkinesis.
- Selective Denervation: Neurolysis/myectomy for persistent synkinesis or hyperkinesis.
- Rehabilitation: Facial neuromuscular retraining, physiotherapy.
- Botulinum Toxin (BoNT):

High‑Yield Points - ⚡ Biggest Takeaways
- House-Brackmann scale is pivotal for facial palsy grading.
- Dynamic reanimation aims for movement; static procedures provide support.
- Common nerve grafts: sural and great auricular.
- Key nerve transfers: hypoglossal-facial (XII-VII) and masseteric-facial.
- Muscle transfers (e.g., temporalis, gracilis) are used for irreversible muscle atrophy.
- Gracilis free flap + masseteric nerve is a common "smile surgery" technique.
- Botulinum toxin manages synkinesis and contralateral hyperactivity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

