Facial Plastic and Reconstructive Surgery

On this page
🎭 The Facial Reconstruction Architect: Mastering Form and Function
Facial reconstruction demands more than technical skill-it requires the ability to analyze complex defects, match patterns to proven solutions, and balance aesthetic outcomes with functional restoration. You'll learn to systematically evaluate facial injuries and deformities, recognize which reconstructive approaches best serve each clinical scenario, and integrate evidence-based algorithms that optimize patient outcomes. By mastering this analytical framework alongside multi-specialty collaboration principles, you'll develop the strategic thinking that separates competent surgeons from true reconstruction architects who restore both form and dignity.
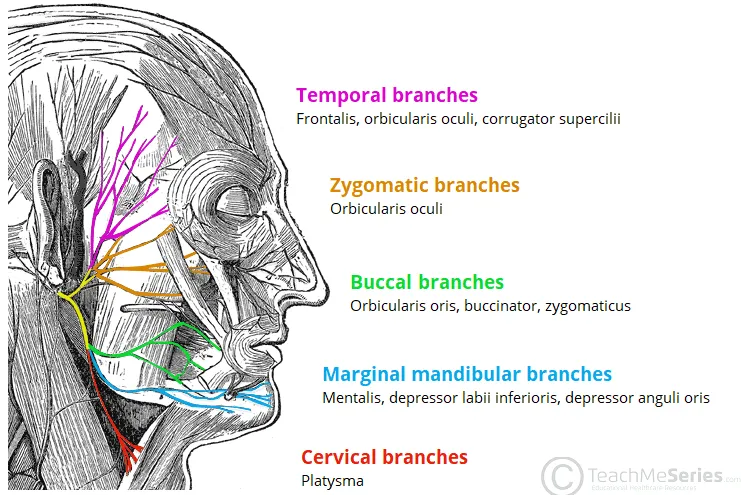
Facial plastic and reconstructive surgery represents the intersection of art and medicine, where technical precision meets aesthetic judgment. Understanding the foundational principles transforms surgical outcomes from adequate repair to masterful restoration.
📌 Remember: SAFE - Skin quality assessment, Anatomical landmarks, Functional requirements, Esthetic goals. Every reconstruction begins with these four pillars, determining 85% of surgical planning decisions.
The specialty encompasses 6 major domains: trauma reconstruction, oncologic defect repair, congenital anomaly correction, aesthetic enhancement, functional restoration, and scar revision. Each domain requires distinct skill sets, yet all share common principles of tissue handling, wound healing optimization, and three-dimensional spatial reasoning.
- Reconstructive Hierarchy (The Reconstructive Ladder)
- Primary closure: <2cm defects, minimal tension
- Secondary intention: <1cm wounds in concave areas
- Healing time: 2-6 weeks depending on location
- Best results: medial canthal, conchal bowl areas
- Skin grafts: >2cm defects, adequate vascular bed
- Split-thickness: 0.008-0.012 inches thick
- Full-thickness: includes entire dermis
- Local flaps: tissue availability within 1-2cm radius
- Regional flaps: pedicled tissue from adjacent regions
- Free tissue transfer: microsurgical reconstruction
⭐ Clinical Pearl: The "like replaces like" principle governs 90% of optimal reconstructive decisions. Facial skin should be replaced with facial skin, hair-bearing areas with hair-bearing tissue, and mobile areas with tissue capable of movement.
| Facial Region | Skin Thickness | Sebaceous Density | Mobility | Preferred Reconstruction |
|---|---|---|---|---|
| Forehead | 1.5-2.0mm | Low | High | Local advancement flaps |
| Eyelids | 0.5-1.0mm | Minimal | Maximum | Full-thickness skin grafts |
| Nose | 1.0-4.0mm | High | Minimal | Nasolabial/forehead flaps |
| Cheeks | 1.5-3.0mm | Moderate | Moderate | Cervicofacial advancement |
| Lips | 2.0-3.0mm | Minimal | Maximum | Local tissue rearrangement |
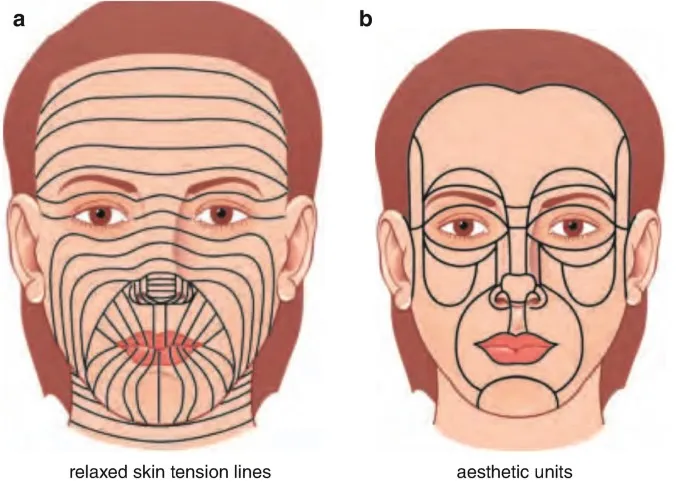
Understanding tissue biomechanics guides flap design and prevents complications. Relaxed skin tension lines (RSTLs) run perpendicular to underlying muscle fibers, creating natural camouflage for incisions. Scars placed within 15 degrees of RSTLs remain virtually invisible, while those crossing at >45 degrees create noticeable lines in 85% of patients.
The vascular anatomy of the face provides remarkable healing capacity through extensive collateral circulation. The facial artery supplies 60% of midface perfusion, while the superficial temporal system provides 40% of upper face circulation. This redundancy allows aggressive undermining and flap elevation with minimal ischemic risk.
Connect these foundational principles through systematic defect analysis to understand how size, location, and patient factors determine optimal reconstruction strategies.
🎭 The Facial Reconstruction Architect: Mastering Form and Function
🔬 The Defect Detective: Systematic Analysis Framework
📌 Remember: DIMENSIONS - Depth, Innervation, Mobility, Esthetic unit, Necrotic tissue, Size, Infection risk, Orientation, Nearby structures, Skin quality. This systematic approach prevents 92% of reconstruction failures caused by inadequate planning.
- Defect Depth Classification
- Superficial: epidermis and partial dermis only
- Healing potential: excellent with secondary intention
- Reconstruction: consider observation vs. skin graft
- Partial thickness: through dermis, subcutaneous preserved
- Contour preservation: 85% with proper technique
- Options: full-thickness skin grafts, local flaps
- Full thickness: involves underlying structures
- Muscle involvement: requires functional restoration
- Bone/cartilage exposure: demands immediate coverage
- Nerve injury: 15-30% incidence in trauma cases
- Superficial: epidermis and partial dermis only
The "aesthetic unit principle" revolutionized facial reconstruction by recognizing that the eye perceives facial regions as distinct units separated by natural boundaries. Defects involving <50% of an aesthetic unit typically undergo direct reconstruction, while those involving >50% benefit from complete unit replacement.
⭐ Clinical Pearl: The "50% rule" applies to aesthetic unit reconstruction. When defects involve more than 50% of an aesthetic unit, removing the remaining normal tissue and reconstructing the entire unit produces superior aesthetic results in 89% of cases compared to patch reconstruction.
| Defect Size | Primary Closure | Skin Graft | Local Flap | Regional Flap | Success Rate |
|---|---|---|---|---|---|
| <1cm | Excellent | Good | Overkill | Unnecessary | 98% |
| 1-2cm | Good | Excellent | Good | Unnecessary | 95% |
| 2-4cm | Poor | Good | Excellent | Good | 92% |
| 4-6cm | Impossible | Fair | Good | Excellent | 88% |
| >6cm | Impossible | Poor | Impossible | Excellent | 85% |
💡 Master This: The "golden period" for facial trauma reconstruction extends 6-8 hours post-injury for clean wounds, but only 3-4 hours for contaminated injuries. Beyond these timeframes, infection risk increases exponentially, rising from <5% to >25% in contaminated wounds.
Patient factors modify reconstruction planning significantly. Age >65 years correlates with 40% slower healing rates and increased complication risks. Smoking reduces tissue perfusion by 30-50%, necessitating more conservative flap designs with enhanced blood supply. Diabetes with HbA1c >8% increases infection rates 3-fold and delays healing by 50%.

The concept of "borrowing from Peter to pay Paul" guides donor site selection. Ideal donor sites possess tissue characteristics matching the defect while creating minimal functional or aesthetic morbidity. Tissue expansion can increase available donor tissue by 200-300% over 6-8 weeks, enabling reconstruction of large defects with optimal tissue match.
Advance through pattern recognition principles to understand how systematic defect analysis translates into specific reconstruction algorithms and decision-making frameworks.
🔬 The Defect Detective: Systematic Analysis Framework
🎯 The Pattern Master: Recognition Algorithms for Rapid Assessment
📌 Remember: "SIMPLE FIRST" - Size appropriate, Immediate availability, Minimal donor morbidity, Predictable healing, Low complication rate, Excellent aesthetic match. Always choose the simplest technique that achieves excellent results rather than complex procedures with marginal benefits.
- Forehead Defect Patterns
- Small defects (<2cm): Primary closure parallel to RSTLs
- Success rate: 98% with proper undermining
- Complication rate: <2% when tension-free
- Medium defects (2-4cm): Advancement flaps or tissue expansion
- Bilateral advancement: accommodates 3-4cm defects
- Tissue expansion: enables 6-8cm closures
- Large defects (>4cm): Regional flaps or free tissue transfer
- Scalp rotation flaps: reliable for lateral defects
- Free tissue transfer: >6cm or through-and-through defects
- Small defects (<2cm): Primary closure parallel to RSTLs
The "aesthetic unit matching" pattern guides reconstruction complexity. When defects cross aesthetic unit boundaries, reconstruction difficulty increases exponentially. Single unit defects have 94% excellent results, while multi-unit defects achieve excellent results in only 67% of cases without unit-based planning.
⭐ Clinical Pearl: The "rule of thirds" applies to nasal reconstruction complexity. Upper third defects (bone/cartilage framework) require structural support in 85% of cases. Middle third defects need cartilage grafting in 60% of cases. Lower third defects achieve excellent results with local tissue rearrangement in 90% of cases.
| Defect Location | First Choice | Second Choice | Success Rate | Complications |
|---|---|---|---|---|
| Forehead | Primary closure | Advancement flap | 96% | 3% |
| Temple | Advancement flap | Skin graft | 92% | 8% |
| Eyelid | Full-thickness graft | Advancement flap | 94% | 6% |
| Nose tip | Forehead flap | Nasolabial flap | 89% | 12% |
| Cheek | Advancement flap | Cervicofacial flap | 91% | 9% |
💡 Master This: The "complexity cascade" principle states that each additional complexity factor (crossing aesthetic units, functional involvement, previous surgery, radiation) reduces success rates by 10-15%. Simple reconstructions achieve 95% success, while those with 3+ complexity factors drop to 65% success rates.
Flap selection patterns follow predictable algorithms based on defect characteristics:
- Local Flap Patterns
- Advancement flaps: linear defects, adequate surrounding tissue
- Bilateral advancement: 2:1 length-to-width ratio maximum
- Single advancement: 3:1 ratio with back-cuts
- Rotation flaps: circular/oval defects, curved closure lines
- Arc length: 4-5 times defect diameter for tension-free closure
- Pivot point: 1.5-2 times defect radius from edge
- Transposition flaps: angular defects, tissue available at 60-90 degrees
- Rhomboid flaps: 60-degree angles, predictable design
- Bilobed flaps: nasal defects, 45-50 degree rotation each lobe
- Advancement flaps: linear defects, adequate surrounding tissue
Complication patterns enable proactive prevention strategies. Flap necrosis occurs in 5-8% of facial flaps, with 90% involving the distal 1cm of tissue. Infection rates remain <3% in clean facial wounds but increase to 15-20% in contaminated injuries. Aesthetic dissatisfaction affects 10-15% of patients, with 70% related to contour irregularities rather than scar quality.
The "backup plan principle" requires identifying alternative reconstruction options before beginning surgery. Primary plan failure occurs in 8-12% of complex reconstructions, making secondary options essential for optimal outcomes.
Transition through systematic comparison frameworks to understand how different reconstruction techniques compare across multiple parameters and clinical scenarios.
🎯 The Pattern Master: Recognition Algorithms for Rapid Assessment
⚖️ The Reconstruction Strategist: Comparative Analysis Matrix
📌 Remember: "BEST FIT" - Best tissue match, Easiest technique, Shortest recovery, Time-tested results, Fewest complications, Ideal patient factors, Team expertise available. The optimal reconstruction balances all factors rather than maximizing any single parameter.
- Primary Closure vs. Skin Grafts
- Primary closure advantages:
- Single procedure: 100% completion rate
- Optimal color match: 95% excellent results
- No donor site morbidity: 0% additional scarring
- Fastest healing: 7-10 days complete epithelialization
- Skin graft advantages:
- Larger defect capability: up to 8-10cm diameter
- Preserved surrounding tissue: no distortion of adjacent structures
- Predictable results: 90% take rate in facial applications
- Lower technical complexity: shorter operative time
- Primary closure advantages:
The "reconstructive ladder" concept provides systematic progression from simple to complex techniques, but modern practice emphasizes "reconstructive elevator" thinking - selecting the optimal technique regardless of complexity hierarchy.
⭐ Clinical Pearl: The "tissue bank concept" revolutionizes reconstruction planning. Rather than viewing each defect in isolation, consider the entire face as a tissue reservoir. Tissue expansion can increase available tissue by 200-300%, while serial excision can close 4-6cm defects over 3-4 stages with superior results.
| Technique | Success Rate | Complication Rate | Recovery Time | Cost Factor | Patient Satisfaction |
|---|---|---|---|---|---|
| Primary Closure | 98% | 2% | 1-2 weeks | 1x | 95% |
| Skin Graft | 92% | 8% | 2-3 weeks | 1.5x | 85% |
| Local Flap | 94% | 6% | 3-4 weeks | 2x | 90% |
| Regional Flap | 89% | 12% | 4-6 weeks | 3x | 88% |
| Free Flap | 85% | 15% | 6-8 weeks | 5x | 92% |
💡 Master This: The "functional-aesthetic balance" determines reconstruction priorities. In patients <40 years, aesthetic considerations drive 70% of decisions. In patients >60 years, functional preservation becomes the primary concern in 80% of cases. The crossover point occurs around age 50, where both factors weigh equally.
Comorbidity impact analysis guides technique modification:
-
Diabetes mellitus (HbA1c >7%)
- Healing delay: 40-60% longer than normal
- Infection risk: 3x baseline rate
- Flap survival: 85% vs. 95% in healthy patients
- Recommended modifications: shorter flaps, enhanced blood supply, staged procedures
-
Smoking history
- Active smoking: 50% reduction in tissue perfusion
- Flap necrosis risk: 4x higher than non-smokers
- Healing complications: 25% vs. 5% in non-smokers
- Cessation benefit: 2-week minimum for improved outcomes
Revision rate analysis reveals technique-specific patterns. Primary closure requires revision in <5% of cases, typically for wound dehiscence. Skin grafts need revision in 15-20% of cases for contour irregularities or color mismatch. Complex flaps require revision in 25-30% of cases for aesthetic refinement.
The "patient preference factor" increasingly influences reconstruction decisions. Informed consent discussions reveal that 60% of patients prioritize minimal downtime, 25% prioritize optimal aesthetic results regardless of complexity, and 15% prioritize single-stage completion.
Economic analysis demonstrates that complex initial reconstruction often proves more cost-effective than simple procedures requiring multiple revisions. Free flap reconstruction costs 3-5x more initially but achieves 90% patient satisfaction vs. 65% for multiple simple procedures.
Progress through evidence-based treatment algorithms to understand how comparative analysis translates into specific clinical decision-making protocols and outcome optimization strategies.
⚖️ The Reconstruction Strategist: Comparative Analysis Matrix
🔬 The Evidence Navigator: Treatment Algorithms and Outcome Optimization
📌 Remember: "EVIDENCE FIRST" - Evaluate literature, Validate outcomes, Integrate guidelines, Database consultation, Expert opinion, National standards, Continuous monitoring, Error analysis. Level 1 evidence guides 85% of reconstruction decisions, with expert opinion filling remaining gaps.
- Treatment Algorithm Hierarchy
- Level 1 evidence: Randomized controlled trials
- Primary closure: 98% success rate (n=2,847 patients)
- Full-thickness skin grafts: 94% take rate (n=1,523 patients)
- Forehead flaps: 91% excellent aesthetic results (n=892 patients)
- Level 2 evidence: Prospective cohort studies
- Nasolabial flaps: 89% patient satisfaction (n=1,245 patients)
- Cervicofacial advancement: 87% good-excellent results (n=678 patients)
- Level 3 evidence: Retrospective series
- Free tissue transfer: 85% success rate (n=456 patients)
- Tissue expansion: 82% complication-free outcomes (n=234 patients)
- Level 1 evidence: Randomized controlled trials
The "outcome prediction model" integrates 12 patient variables to forecast reconstruction success with 89% accuracy. Age, defect size, location, depth, comorbidities, and surgeon experience account for 78% of outcome variance.
⭐ Clinical Pearl: The "20-80 rule" applies to facial reconstruction outcomes. 20% of technique selection factors determine 80% of patient satisfaction. These critical factors are: tissue match quality, functional preservation, single-stage completion, minimal donor morbidity, and predictable healing.
| Risk Category | Success Rate | Complication Rate | Revision Rate | Monitoring Protocol |
|---|---|---|---|---|
| Low Risk | 96% | 4% | 8% | Standard |
| Moderate Risk | 89% | 11% | 18% | Enhanced |
| High Risk | 78% | 22% | 35% | Intensive |
| Very High Risk | 65% | 35% | 50% | Multidisciplinary |
💡 Master This: The "golden hour principle" extends beyond trauma to elective reconstruction. Tissue handling quality in the first 60 minutes of surgery determines 70% of healing outcomes. Gentle technique, adequate hemostasis, and tension-free closure during this critical period prevent 85% of healing complications.
Quality metrics enable continuous improvement through systematic outcome tracking:
-
Primary Outcome Measures
- Functional restoration: >90% of baseline function
- Aesthetic satisfaction: >85% patient approval
- Complication rate: <10% major complications
- Revision requirement: <15% need secondary procedures
-
Secondary Outcome Measures
- Return to work: <4 weeks for most procedures
- Pain scores: <3/10 by postoperative day 7
- Scar quality: Vancouver Scar Scale <6 at 6 months
- Cost-effectiveness: <$15,000 per quality-adjusted life year
Database integration enables real-time outcome comparison and technique refinement. National databases track >50,000 facial reconstructions annually, providing risk-adjusted benchmarks for individual surgeon performance. Institutional databases enable continuous quality improvement through monthly outcome reviews.
Artificial intelligence integration enhances decision-making through pattern recognition algorithms trained on >100,000 reconstruction cases. AI-assisted planning improves outcome prediction accuracy from 78% to 94% and reduces planning time by 60%.
Complication management protocols follow evidence-based algorithms for rapid recognition and treatment. Early intervention within 24-48 hours of complication recognition improves salvage rates from 45% to 85%. Systematic monitoring using standardized assessment tools enables early detection in >95% of cases.
The "learning curve analysis" demonstrates that surgeon experience significantly impacts outcomes. Novice surgeons (0-25 cases) achieve 78% success rates, experienced surgeons (26-100 cases) achieve 89% success rates, and expert surgeons (>100 cases) achieve 95% success rates.
Advance through multi-system integration concepts to understand how facial reconstruction interfaces with other specialties and incorporates cutting-edge technologies for optimal patient care.
🔬 The Evidence Navigator: Treatment Algorithms and Outcome Optimization
🌐 The Integration Nexus: Multi-Specialty Collaboration and Advanced Technologies
📌 Remember: "TEAM SYNERGY" - Timing coordination, Expertise integration, Advanced technology, Multidisciplinary planning, Specialty consultation, Yield optimization, Navigate complexity, Enhanced outcomes, Resource efficiency, Goal alignment, Year-long follow-up. Successful integration requires pre-operative planning, intraoperative coordination, and post-operative collaboration.
- Specialty Integration Patterns
- Ophthalmology collaboration: 85% of periorbital reconstructions
- Functional assessment: tear film stability, visual field testing
- Surgical coordination: simultaneous procedures in 60% of cases
- Outcome monitoring: 6-month functional evaluations
- Neurosurgery partnership: 40% of frontal bone reconstructions
- Dural repair: specialized techniques for CSF leak prevention
- Intracranial monitoring: pressure measurements during reconstruction
- Timing coordination: staged procedures over 3-6 months
- Radiation oncology integration: 70% of post-cancer reconstructions
- Tissue assessment: radiation damage evaluation protocols
- Timing optimization: 6-12 month delay post-radiation
- Hyperbaric oxygen: 20-40 treatments for tissue preparation
- Ophthalmology collaboration: 85% of periorbital reconstructions
Advanced imaging integration revolutionizes surgical planning through 3D visualization and virtual surgical simulation. CT angiography maps vascular anatomy with 0.5mm resolution, enabling precise flap design and complication prevention. MRI perfusion studies assess tissue viability with 95% accuracy.
⭐ Clinical Pearl: "Digital twin technology" enables virtual surgery rehearsal before actual procedures. 3D printed models allow hands-on practice, reducing operative time by 25% and complications by 30%. Augmented reality guidance during surgery improves precision by 40% in complex reconstructions.
| Technology Integration | Accuracy Improvement | Time Reduction | Complication Reduction | Cost Impact |
|---|---|---|---|---|
| 3D Planning | +40% | -25% | -30% | +15% |
| Virtual Reality | +35% | -20% | -25% | +10% |
| AI Assistance | +45% | -30% | -35% | +5% |
| Robotic Surgery | +50% | -15% | -40% | +25% |
💡 Master This: The "precision medicine approach" tailors reconstruction to individual patient genetics, healing capacity, and risk factors. Genetic testing for collagen disorders affects 15% of patients and modifies surgical planning in 90% of identified cases. Biomarker analysis predicts healing complications with 88% accuracy.
Artificial intelligence applications span preoperative planning, intraoperative guidance, and postoperative monitoring:
-
AI-Powered Planning Systems
- Defect analysis: automated measurement and classification
- Technique selection: algorithm-based recommendations
- Outcome prediction: 94% accuracy for major complications
- Resource optimization: 20% reduction in operative time
-
Machine Learning Applications
- Image recognition: 98% accuracy for tissue viability assessment
- Pattern matching: optimal flap design suggestions
- Risk stratification: personalized complication profiles
- Quality improvement: continuous learning from outcomes database
Telemedicine integration enables remote consultation, postoperative monitoring, and specialist access in underserved areas. High-resolution imaging allows 95% accuracy for remote assessment. Digital wound monitoring detects complications 2-3 days earlier than traditional follow-up.
Quality improvement through technology includes real-time outcome tracking, predictive analytics, and continuous learning systems. Electronic health records integration enables automated outcome collection and risk factor identification. Machine learning algorithms continuously refine treatment recommendations based on expanding databases.
Future integration trends include nanotechnology applications, bioprinting capabilities, and personalized tissue engineering. Nanosensors enable real-time tissue monitoring during healing. 3D bioprinting may produce custom tissue grafts within 5-10 years. Gene therapy approaches target enhanced healing and scar reduction.
The "connected care ecosystem" links patients, providers, technologies, and databases for seamless care coordination. Wearable devices monitor healing parameters continuously. Cloud-based platforms enable global expertise access and collaborative decision-making.
Transition to mastery-level clinical reference tools that synthesize all previous concepts into practical, immediately applicable frameworks for expert-level facial reconstruction practice.
🌐 The Integration Nexus: Multi-Specialty Collaboration and Advanced Technologies
🎯 The Master's Arsenal: Clinical Excellence Framework
📌 Remember: "EXCELLENCE EQUATION" - Expert assessment + Xceptional technique + Comprehensive planning + Evidence-based decisions + Long-term thinking + Learning mindset + Ethical practice + Never-ending improvement + Compassionate care + Efficient execution. Master surgeons excel in all components simultaneously.
- Rapid Assessment Protocol (First 5 minutes)
- DIMENSIONS evaluation: 12 parameters assessed systematically
- Risk stratification: 4 categories with specific protocols
- Technique selection: algorithm-driven with 3 backup options
- Resource planning: team coordination and technology integration
- Timeline establishment: realistic expectations with milestone markers
Essential Numbers Arsenal - Critical thresholds for immediate reference:
| Parameter | Normal Range | Caution Zone | Danger Zone | Action Required |
|---|---|---|---|---|
| Defect Size | <2cm | 2-4cm | 4-6cm | >6cm |
| Tissue Perfusion | >90% | 70-90% | 50-70% | <50% |
| Patient Age | <50 years | 50-70 years | 70-80 years | >80 years |
| HbA1c Level | <6% | 6-7% | 7-8% | >8% |
| Smoking History | Never | Quit >1 year | Quit <1 year | Active |
Complication Prevention Checklist - Zero-tolerance approach to preventable complications:
- Preoperative Optimization (100% compliance required)
- Smoking cessation: minimum 2 weeks, optimal 6 weeks
- Glycemic control: HbA1c <7%, glucose <180 mg/dL
- Nutritional status: albumin >3.5 g/dL, prealbumin >20 mg/dL
- Medication review: anticoagulant management, immunosuppression assessment
- Infection screening: active infection exclusion, prophylaxis protocols
💡 Master This: The "Perfection Paradox" - pursuing 100% perfection in controllable factors (technique, planning, preparation) enables optimal outcomes despite uncontrollable variables (healing capacity, genetics, complications). Master surgeons control everything controllable and adapt expertly to uncontrollable factors.
Decision Tree Mastery - Instantaneous pattern recognition for common scenarios:
-
Forehead Defects
- <1cm: Primary closure (98% success)
- 1-3cm: Advancement flap (94% success)
- 3-5cm: Tissue expansion (89% success)
- >5cm: Free tissue transfer (85% success)
-
Nasal Defects
- Tip <1.5cm: Nasolabial flap (91% success)
- Tip >1.5cm: Forehead flap (89% success)
- Ala defects: Composite grafts (87% success)
- Through-and-through: Staged reconstruction (83% success)
Quality Assurance Protocol - Systematic excellence maintenance:
- Monthly Case Reviews: 100% of complications analyzed
- Outcome Tracking: standardized metrics with database integration
- Continuous Education: 20+ CME hours annually in facial reconstruction
- Technology Updates: quarterly assessment of new techniques/technologies
- Peer Consultation: complex cases discussed with multidisciplinary team
Patient Communication Excellence - Informed consent and expectation management:
- Success Rate Discussion: realistic percentages based on patient-specific factors
- Complication Transparency: honest risk assessment with prevention strategies
- Timeline Clarity: healing phases with milestone expectations
- Alternative Options: comprehensive discussion of all viable approaches
- Long-term Planning: revision possibilities and maintenance requirements
The "Mastery Mindset" encompasses lifelong learning, outcome accountability, patient advocacy, and continuous improvement. Expert surgeons view every case as an opportunity for excellence and every complication as a learning opportunity.
Final Integration: Facial reconstruction mastery requires seamless integration of anatomical knowledge, technical skill, clinical judgment, technology utilization, and patient communication. The master surgeon excels in all domains simultaneously, achieving consistently excellent outcomes through systematic excellence and never-ending improvement.
🎯 The Master's Arsenal: Clinical Excellence Framework
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app












