Thyroid Cancer - Thyroid 101: Risky Business
- Definition: Malignant tumor originating from thyroid follicular or parafollicular C cells.
- Epidemiology:
-
⭐ Most common endocrine malignancy.
- India: Accounts for ~1-2% of all cancers; incidence rising.
-
- Key Risk Factors:
- Radiation exposure: Especially in childhood (< 15 yrs); dose-dependent (e.g., 5-10 Gy).
- Family history: Syndromic (e.g., MEN2, FAP, Cowden syndrome) or non-syndromic familial thyroid cancer.
- Iodine status: Deficiency (↑ follicular cancer risk); Excess (possible ↑ papillary cancer risk, debated).
- Female gender.
- Age extremes (childhood, >45 yrs).
- Pre-existing benign thyroid conditions (e.g., goiter, adenomas).
Thyroid Cancer - Cellular Rogues Gallery
- Thyroid malignancies: follicular epithelial or parafollicular C-cell origin.
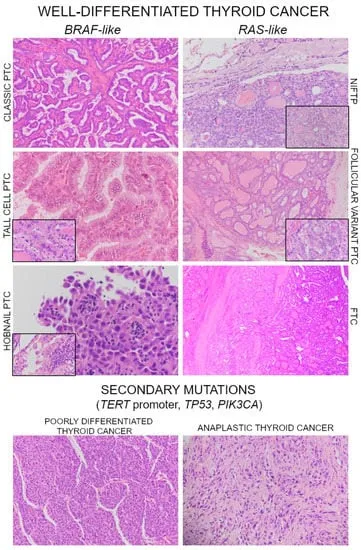
- 📌 Papillary: Popular (~80%), Psammoma bodies, Positive Prognosis.
| Feature | Papillary (PTC) | Follicular (FTC) | Medullary (MTC) | Anaplastic (ATC) |
|---|---|---|---|---|
| Origin | Follicular cells | Follicular cells | Parafollicular C-cells | Dedifferentiated cells |
| Histo Key | Orphan Annie nuclei, Psammoma bodies, nuclear grooves | Capsular/vascular invasion defines malignancy | Amyloid stroma (Congo red+), spindle cells | Marked pleomorphism, high mitoses |
| Genetics | BRAF V600E, RET/PTC | RAS, PAX8-PPARγ | RET (MEN2A/2B assoc.) | TP53, BRAF, TERT |
| Prognosis | Excellent, indolent | Good, hematogenous spread | Moderate, ↑Calcitonin | Dismal, highly aggressive |
Thyroid Cancer - Nodule CSI: Case Cracked
- Presentation: Solitary thyroid nodule (most common); hoarseness, dysphagia, stridor (compressive symptoms).
- Diagnostic Workup:
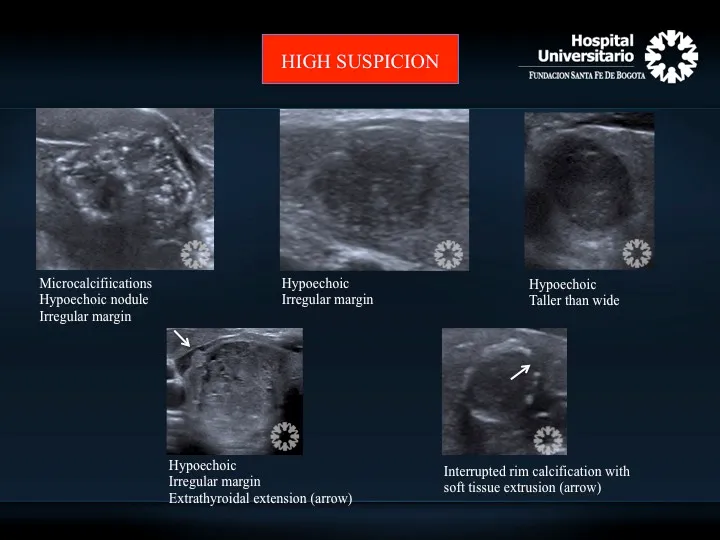
- USG: Initial. Suspicious: microcalcifications, hypoechogenicity, irregular margins, taller-than-wide, ↑vascularity.
- Serum TSH: If normal/high & USG suspicious → FNAC. If low → Radionuclide scan (cold nodule? → FNAC).
- FNAC: Bethesda System (Categories I-Nondiagnostic to VI-Malignant).

- Serum Calcitonin: If Medullary Thyroid Cancer (MTC) suspected (family Hx, USG).
- Serum Thyroglobulin (Tg): Post-op surveillance for differentiated cancers (PTC, FTC).
- USG: Initial. Suspicious: microcalcifications, hypoechogenicity, irregular margins, taller-than-wide, ↑vascularity.
⭐ FNAC is the most important initial diagnostic test for a thyroid nodule.
Thyroid Cancer - Thyroid Takedown Tactics
- Surgery: Primary treatment.
- Total Thyroidectomy (TT): Standard for most.
- Lobectomy: For small, low-risk unifocal DTC.
- Neck Dissection: Nodal disease (therapeutic); prophylactic central for MTC.
- Radioactive Iodine ($I^{131}$): Post-TT for DTC remnant/mets.
- Ablation (30-100 mCi), adjuvant, metastatic disease.
- TSH Suppression: Levothyroxine to ↓TSH, prevent recurrence.
- High-risk: <0.1 mIU/L. Low-risk: 0.1-0.5 mIU/L.
- Advanced/Refractory:
- EBRT: Unresectable, residual disease, palliative.
- Systemic: TKIs (Lenvatinib-DTC, Vandetanib-MTC), Chemo (ATC).
⭐ Differentiated thyroid cancers (papillary, follicular) are typically iodine-avid, making $I^{131}$ therapy effective.
Thyroid Cancer - Post-Op: The Long Haul
- Prognostic Factors: Age (e.g., <55 yrs better), tumor size, extrathyroidal extension, histological type, molecular markers (e.g., BRAF).
- Differentiated Thyroid Cancer (DTC) Follow-up:
- Serum Thyroglobulin (Tg) & anti-Tg antibodies (key for recurrence).
- Neck Ultrasound (USG).
- Medullary Thyroid Cancer (MTC) Follow-up:
- Serum Calcitonin & CEA levels.
- Neck USG.
⭐ Rising Thyroglobulin (Tg) levels post-thyroidectomy in DTC strongly suggest recurrence or persistent disease.
High‑Yield Points - ⚡ Biggest Takeaways
- Papillary Ca: Most common, Orphan Annie eyes, psammoma bodies, lymphatic spread, best prognosis.
- Follicular Ca: Hematogenous spread, needs capsular/vascular invasion for diagnosis (not by FNAC alone).
- Medullary Ca: From C-cells, linked to MEN2 (RET), secretes calcitonin (tumor marker).
- Anaplastic Ca: Elderly, rapid growth, aggressive, worst prognosis.
- FNAC: Best initial test for thyroid nodules.
- Treatment: Total thyroidectomy then RAI ablation for differentiated (Papillary, Follicular) cancers.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

