Salivary Glands 101 - Anatomy & Adversaries
- Major Glands & Secretion Types: Parotid (Serous), Submandibular (Mixed), Sublingual (Mucous) - 📌 PSM SM M
- Parotid: Largest. Duct: Stensen's.
- Facial nerve (CN VII) traverses (no innervation).
- Submandibular: Duct: Wharton's.
- Sublingual: Smallest. Ducts: Bartholin's, Rivinus.
- Parotid: Largest. Duct: Stensen's.
- Minor Glands: Numerous, in oral mucosa (e.g., von Ebner's).
- WHO Classification (Epithelial Neoplasms):
- Benign:
- Pleomorphic Adenoma (most common overall).
- Warthin's Tumor (papillary cystadenoma lymphomatosum).
- Malignant:
- Mucoepidermoid Carcinoma (most common malignant).
- Adenoid Cystic Carcinoma (ACC) (perineural invasion).
- Acinic Cell Carcinoma.
- Carcinoma ex Pleomorphic Adenoma (Ca ex PA).
- Benign:
⭐ Frey's syndrome (gustatory sweating): post-parotidectomy complication due to auriculotemporal nerve misdirection.
Benign Beauties - Mostly Harmless Masses
-
Pleomorphic Adenoma (Benign Mixed Tumor)
- Most common salivary gland tumor overall.
- Can present as 'Dumbbell tumor' (parapharyngeal space).
- Histology: epithelial & myoepithelial cells in varied stroma (e.g., chondromyxoid).

- Slow-growing, painless mass.
- Malignant transformation risk (Carcinoma ex PA): ~1.5% up to 5 yrs, ~9.5% after 15 yrs.
⭐ Pleomorphic adenoma is the most common salivary gland tumor, accounting for about 80% of benign parotid tumors.
-
Warthin's Tumor (Papillary Cystadenoma Lymphomatosum)
- Almost exclusively in parotid gland; common in elderly males, smokers.
- Often bilateral (10%).
- Histology: papillary cystic structures lined by oncocytic epithelium with a lymphoid stroma.

- 📌 Warthin's = Warriors (lymphoid) in old Smoking Men.
Malignant Mayhem - When Glands Go Rogue
- Mucoepidermoid Carcinoma (MEC)
- Most common malignant tumor overall & in children.
- Parotid: most common site.
- Histology: mucous, epidermoid, intermediate cells.
- Graded: Low, Intermediate, High (prognostic).

- Adenoid Cystic Carcinoma (ACC)
- Notorious for perineural invasion (PNI), late distant metastases (lungs).
- Histology: cribriform ('Swiss cheese'), tubular, solid patterns.
- 📌 ACC = Always Creeps around Cranial nerves.
- 5-year survival ~75%, 15-year ~40% due to late mets.
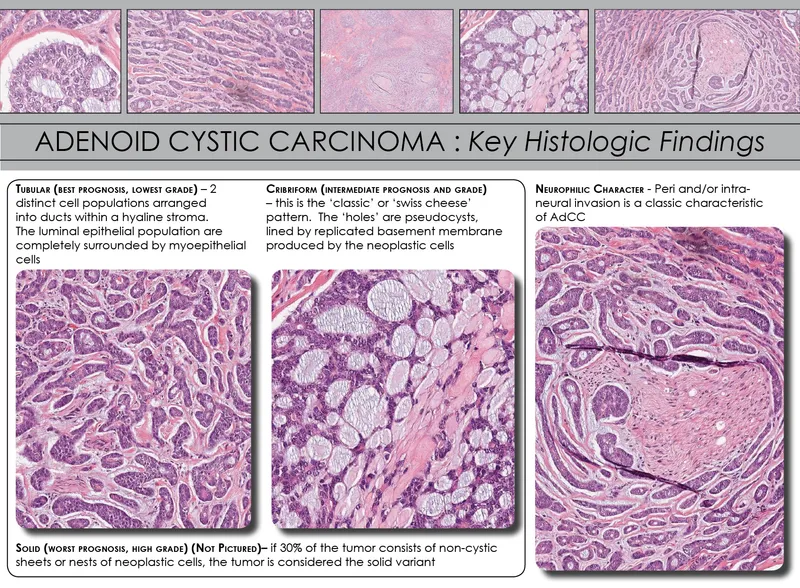
⭐ Perineural invasion is a characteristic feature of Adenoid Cystic Carcinoma, often leading to pain and poor prognosis.
- Acinic Cell Carcinoma
- Low-grade malignancy.
- Good prognosis.
- Histology: serous acinar differentiation.
- Carcinoma ex Pleomorphic Adenoma
- Malignancy arising in a pre-existing Pleomorphic Adenoma (PA).
- Often aggressive; prognosis depends on extent of invasion and grade of carcinoma component.
Clinical Clues & Cures - Spotting & Stopping
- Clinical Presentation:
- Painless swelling (most common).
- Malignancy signs: Pain, facial nerve palsy (VII), rapid growth, skin ulceration, cervical lymphadenopathy.
- 📌 Red Flags: Pain, Palsy, Puckering, Progression (Rapid).
- Investigations:
- FNAC - initial diagnostic test (Accuracy >90% malignancy).
- Imaging: USG (solid/cystic), CT/MRI (extent, PNI, bone invasion, deep lobe).
- Staging:
- TNM (AJCC) - Tumor size/extent (T), Nodal involvement (N), Metastasis (M).
- General Management Principles:
- Surgery (cornerstone).
- Radiotherapy (adjuvant for high-grade, +margins, PNI, recurrent; primary for inoperable).
- Chemotherapy (palliative/advanced).
⭐ FNAC is the investigation of choice for a palpable salivary gland mass, guiding further management.
High‑Yield Points - ⚡ Biggest Takeaways
- Pleomorphic adenoma is the most common salivary gland tumor, overwhelmingly benign.
- Mucoepidermoid carcinoma stands as the most common malignant salivary tumor.
- Parotid gland is the most frequent site; tumors here are predominantly benign (80% rule).
- Submandibular and minor salivary glands exhibit a significantly higher risk of malignancy.
- Adenoid cystic carcinoma is notorious for perineural invasion and late distant metastases.
- Facial nerve palsy accompanying a parotid mass strongly suggests malignancy.
- Warthin's tumor: Almost exclusive to parotid, strongly linked to smoking, often bilateral.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

