Radiobiology & Goals - Zap Zone Science
- Mechanism: DNA damage primarily via indirect action (water radiolysis producing free radicals like OH•) and direct action on DNA.
- Cell Cycle Sensitivity: Most sensitive phases are M & G2; most resistant is late S phase.
- The 4 R's of Radiobiology:
- Repair: Of sublethal cellular damage.
- Repopulation: Proliferation of cells between fractions.
- Redistribution: Cells progress through cell cycle, potentially into more sensitive phases.
- Reoxygenation: Hypoxic tumor cells become oxygenated and more radiosensitive.
- Goals: Curative (e.g., eradicate localized tumor); Palliative (e.g., relieve pain, bleeding).
- Therapeutic Ratio: Aim to maximize Tumor Control Probability (TCP) while minimizing Normal Tissue Complication Probability (NTCP). $TR = TCP / NTCP$.

⭐ Oxygen Enhancement Ratio (OER) is the ratio of radiation doses required to produce the same biological effect under hypoxic versus aerated conditions; for X-rays, OER is typically 2.5-3.5.
Radiation Types & Tech - Beam Team Tactics
- Radiation Types:
- Photons: X-rays (from Linear Accelerators - Linacs), Gamma rays (from Cobalt-60, radioactive isotopes like $^{192}\text{Ir}$, $^{137}\text{Cs}$, $^{125}\text{I}$).
- Particles: Electrons (Linacs), Protons, Carbon ions (hadron therapy).
- External Beam Radiotherapy (EBRT): Source distant.
- Techniques:
- 3D Conformal RT (3D-CRT): Beams match tumor shape.
- Intensity Modulated RT (IMRT): Varying beam intensity; spares organs at risk (OARs).
- Volumetric Modulated Arc Therapy (VMAT): Rapid IMRT delivery.
- Image-Guided RT (IGRT): Ensures accurate targeting.
- Stereotactic Radiosurgery (SRS): Single high dose (e.g., Gamma Knife for brain mets).
- Stereotactic Body RT (SBRT/SABR): 1-5 high-dose fractions for extracranial sites.
- Techniques:
- Brachytherapy: Radioactive source placed in/near tumor.
- Types: Intracavitary, Interstitial, Surface.
- Dose Rates: LDR (Low), HDR (High), PDR (Pulsed).
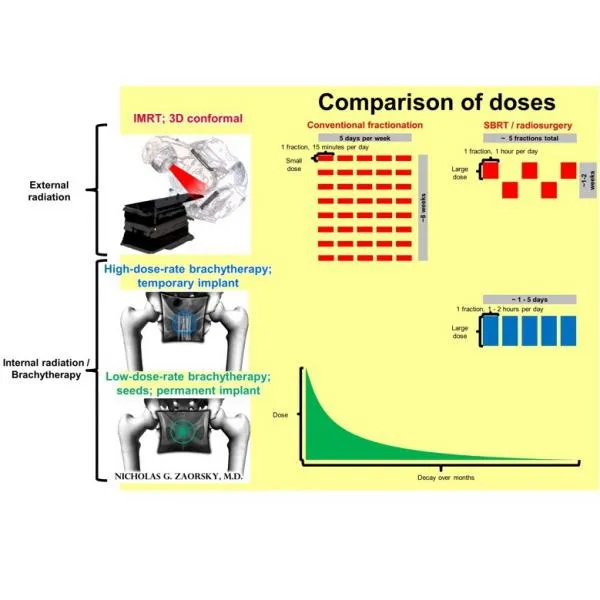
⭐ IMRT significantly reduces xerostomia in head & neck cancers by sparing parotid glands.
Planning & Precision - Target Lock Strategy
- Goal: Maximize tumor dose; minimize normal tissue (OAR) toxicity. Precision is key.
- Planning Workflow:
- Target Volumes (ICRU):
- GTV (Gross Tumor Volume): Visible tumor extent.
- CTV (Clinical Target Volume): GTV + microscopic disease.
- PTV (Planning Target Volume): CTV + margin for setup errors & organ motion. $PTV = CTV + IM + SM$.
- 📌 Mnemonic: Go Catch Patients.
⭐ PTV ensures the CTV receives the prescribed dose despite uncertainties. Its size directly impacts toxicity.

H&N Toxicities & Care - Damage Control Duty
- Acute (≤90 days)
- Mucositis: Pain, dysphagia. WHO/RTOG grades. Rx: Analgesia, hygiene, sucralfate.
- Dermatitis: Erythema, dry/moist desquamation. Rx: Emollients, topical steroids.
- Xerostomia: Salivary gland damage. Rx: Pilocarpine, saliva substitutes.
- Dysgeusia/Ageusia: Altered/lost taste.
- Laryngeal edema: Hoarseness.
- Late (>90 days)
- Xerostomia (often permanent).
- Osteoradionecrosis (ORN): Mandible common. Risk: Dose >60 Gy, post-RT extraction. 📌 PENTOCLO (Pentoxifylline, Tocopherol, Clodronate).
- Soft tissue fibrosis: Trismus, neck stiffness.
- Hypothyroidism: Monitor TSH.
- Laryngeal chondronecrosis/stenosis.
- Radiation-induced secondary malignancy (RISM).
- General Care
- Nutritional support (PEG/Ryles).
- Pre-RT dental assessment & prophylaxis.
- Speech & swallowing rehabilitation.
- Regular, long-term follow-up.
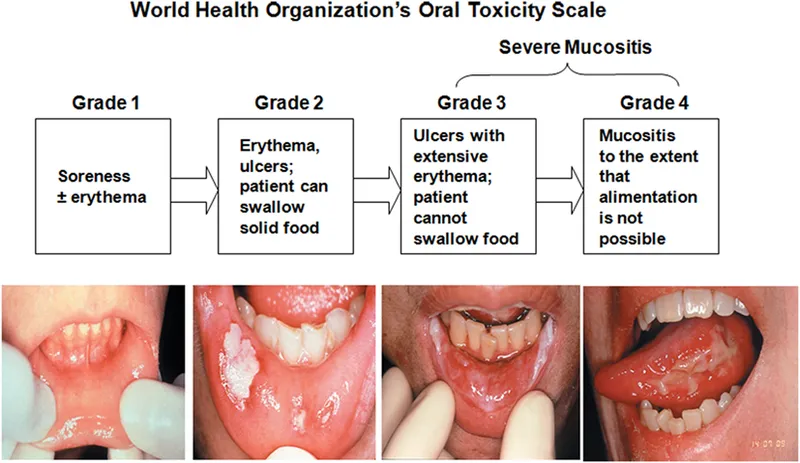
⭐ Osteoradionecrosis (ORN) risk significantly increases with radiation doses >60 Gy to the bone, especially mandible. Dental prophylaxis pre-radiotherapy is crucial for prevention.
High‑Yield Points - ⚡ Biggest Takeaways
- Fractionation is key: spares normal tissue, ↑ tumor kill.
- Teletherapy (External Beam RT) most common; Brachytherapy for localized boosts.
- Radiosensitivity varies: Squamous cell carcinomas are generally radiosensitive.
- IMRT enables precise dose delivery, sparing critical structures like salivary glands.
- Acute effects: Mucositis, dermatitis, xerostomia.
- Late effects: Osteoradionecrosis (ORN), fibrosis, hypothyroidism.
- Concurrent Chemoradiation (CCRT) is standard for advanced H&N cancers, improving outcomes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

