Oral Cavity Cancer - Mouth's Malignant Mayhem
- Malignancy of oral cavity structures: lips, tongue, buccal mucosa, floor of mouth, gingiva, palate, retromolar trigone.
- High incidence in India, primarily due to widespread tobacco and areca nut use.
- Key Risk Factors:
- Tobacco (smoking, smokeless e.g., khaini, gutka).
- Alcohol (synergistic with tobacco).
- Betel quid (areca nut).
- HPV (esp. HPV-16).
- Chronic irritation, poor oral hygiene.
- Predominant Histology: >90% Squamous Cell Carcinoma (SCC).
⭐ Buccal mucosa & tongue are commonest Indian sites (betel quid link).
Oral Cavity Cancer - Mouth Map & Nodes
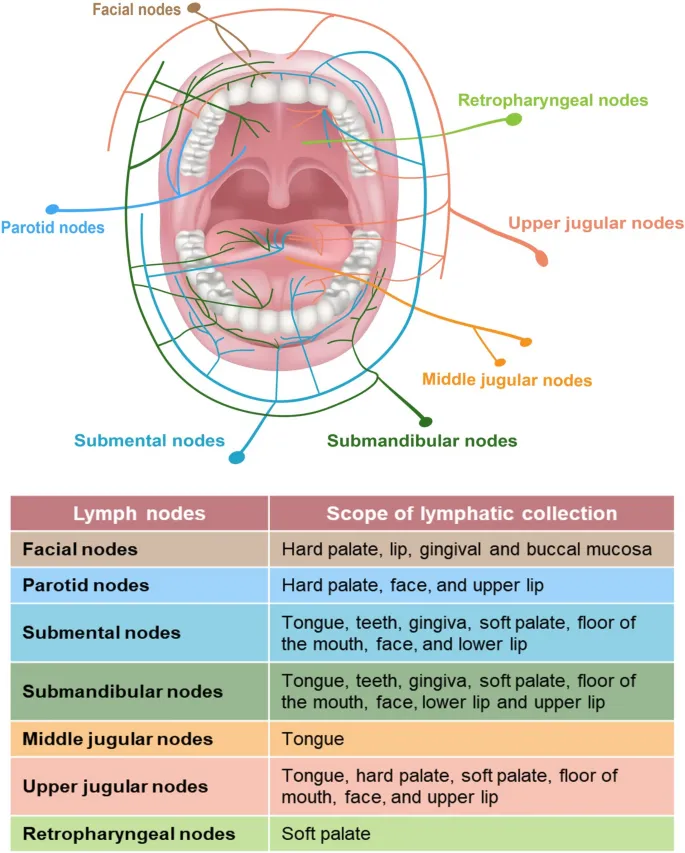
- Key Subsites: Lip, anterior 2/3 tongue (oral tongue), floor of mouth (FOM), buccal mucosa, gingiva (upper/lower), retromolar trigone, hard palate.
- Lymphatic Drainage (Primarily Levels I-III):
- Level I (Submental/Submandibular): FOM, anterior tongue, lip, buccal mucosa.
- Level II (Upper Jugular): All subsites, esp. posterior oral cavity.
- Level III (Mid Jugular): Tongue, FOM.
- Midline lesions → bilateral nodal risk.
⭐ Retromolar trigone cancers often invade mandible early due to close proximity and direct spread through the pterygomandibular raphe and surrounding spaces, impacting staging and resectability assessment significantly. This area is a common site for occult nodal metastases, even in clinically N0 necks, often necessitating elective neck dissection (END).
Oral Cavity Cancer - Clinical Red Flags
- Persistent Symptoms (Suspect if > 3 weeks):
- Non-healing ulcer or sore
- Pain: oral, odynophagia, referred otalgia
- Unexplained bleeding, numbness, or loose teeth
- Trismus (difficulty opening mouth)
- Neck mass/swelling (lymphadenopathy)
- Dysphagia, weight loss (late signs)
- High-Risk Oral Lesions & Signs:
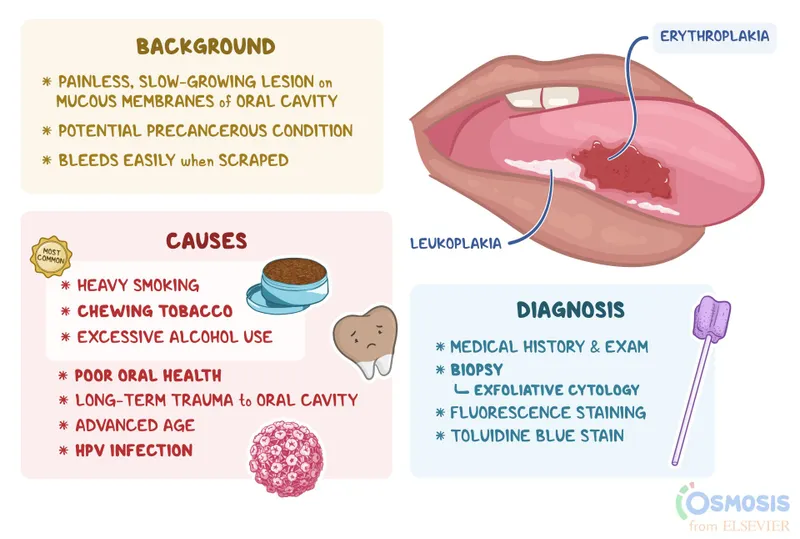
- Leukoplakia (white patch, cannot be wiped off)
- Erythroplakia (velvety red patch) ⚠️
- Erythroleukoplakia (speckled, mixed red/white)
- Palpable induration, fixation, or exophytic growth
- Restricted tongue mobility
- Crucial Diagnostic Step:
- Biopsy (incisional) of any suspicious lesion is mandatory.
- Biopsy (incisional) of any suspicious lesion is mandatory.
⭐ Erythroplakia carries the highest malignant transformation potential among premalignant oral lesions.
Oral Cavity Cancer - Staging the Spread
Staging (AJCC 8th Ed.) considers: Tumor size, Depth of Invasion (DOI), Nodal status (incl. Extranodal Extension - ENE), Metastasis.
- T (Tumor): Assessed by size & critical DOI (Depth of Invasion) thresholds (e.g., 5mm, 10mm).
- N (Nodes): Evaluates site, size, number. 📌 ENE (Extranodal Extension) is a key prognostic factor.
- M (Metastasis): M0 (no distant metastasis) vs M1 (distant metastasis present).
⭐ Depth of Invasion (DOI) significantly impacts T-staging and prognosis, even for small tumors. DOI >5mm can upstage a T1 tumor.
Oral Cavity Cancer - Treatment Blueprints
- Primary Goal: Curative intent with surgery as cornerstone for resectable disease.
- Early Stage (T1-T2, N0):
- Wide local excision.
- Consider Elective Neck Dissection (END) if Depth of Invasion (DOI) > 3-4 mm.
- Locally Advanced (T3-T4, or N+):
- Comprehensive surgery (primary tumor resection + neck dissection).
- Adjuvant Therapy (Post-Sx):
- Radiotherapy (RT): For most pN+ (pathologically positive nodes), close/positive margins, Perineural Invasion (PNI), Lymphovascular Invasion (LVI).
- Concurrent Chemoradiotherapy (CCRT): For Extranodal Extension (ENE) or positive margins.
- Unresectable/Metastatic Disease:
- Palliative chemotherapy and/or radiotherapy; targeted therapy; immunotherapy.
- Reconstruction: Essential for function (speech, swallowing) and quality of life post-resection.
⭐ Extranodal Extension (ENE) in cervical lymph nodes is a powerful adverse prognostic factor and a key indication for adjuvant concurrent chemoradiotherapy (CCRT) rather than RT alone.
High‑Yield Points - ⚡ Biggest Takeaways
- Squamous Cell Carcinoma (SCC) is the dominant histology (>90%).
- Key risk factors: tobacco (smoked/smokeless), alcohol, betel quid (India).
- Tongue (lateral border) is the most common site, followed by floor of mouth.
- Watch for premalignant lesions: leukoplakia, erythroplakia (high malignant potential).
- Cervical lymph node status is a critical prognostic factor.
- Surgery is the primary treatment for early stages; radiotherapy/chemotherapy for advanced.
- Persistent non-healing ulcers or oral pain are common presentations.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

