ENT Oncology

On this page
🎯 ENT Oncology: The Head and Neck Cancer Command Center
Head and neck cancers present a unique clinical challenge where millimeters matter-tumors arise in anatomically complex regions that govern speech, swallowing, breathing, and identity itself. You'll master the staging systems that predict outcomes, develop a systematic diagnostic approach from physical exam to molecular profiling, and learn how multidisciplinary teams orchestrate surgery, radiation, and emerging immunotherapies to maximize both survival and quality of life. This lesson builds your command of ENT oncology from anatomical foundations through cutting-edge precision medicine, equipping you to navigate these consequential diagnoses with clinical confidence and compassionate expertise.

Head and neck cancers represent a complex constellation of malignancies affecting the upper aerodigestive tract, demanding mastery of intricate anatomical relationships, sophisticated staging systems, and multimodal treatment approaches. These cancers account for 4% of all malignancies globally, with 90% being squamous cell carcinomas arising from mucosal surfaces exposed to carcinogenic insults.
📌 Remember: SCALP for major head and neck cancer sites - Sinonasal, Cavity (oral), Aerodigestive (larynx/hypopharynx), Lymphoid (nasopharynx), Pharynx (oropharynx). Each site has distinct epidemiology, with oral cavity showing male predominance 2:1, oropharyngeal cancer increasingly HPV-positive (70% in developed countries), and nasopharyngeal cancer endemic in Southeast Asia (25-50 cases per 100,000).
The anatomical complexity of head and neck regions creates unique challenges in oncological management. The proximity of critical structures - cranial nerves, major vessels, and functional organs - demands precise understanding of fascial planes, lymphatic drainage patterns, and neurovascular territories.
- Primary Sites Distribution:
- Oral cavity: 40% of head and neck cancers
- Larynx: 25% with glottic (60%), supraglottic (35%), subglottic (5%)
- Oropharynx: 20% with increasing HPV association
- Hypopharynx: 10% with poorest prognosis
- Nasopharynx: 5% with EBV association
| Cancer Site | 5-Year Survival | HPV Association | Smoking Risk | Alcohol Risk | Peak Age |
|---|---|---|---|---|---|
| Oral Cavity | 65% | <5% | RR 5-25x | RR 6x | 60-70 |
| Oropharynx | 75% (HPV+) | 70% | RR 10x | RR 8x | 55-65 |
| Larynx | 60% | <5% | RR 20x | RR 4x | 65-75 |
| Hypopharynx | 35% | <10% | RR 15x | RR 10x | 60-70 |
| Nasopharynx | 70% | Rare | RR 2x | RR 2x | 45-55 |
The staging revolution in head and neck oncology reflects our evolving understanding of tumor biology. The AJCC 8th edition introduced separate staging systems for HPV-positive oropharyngeal cancers, recognizing their distinct biological behavior and superior outcomes.
💡 Master This: TNM staging forms the foundation of treatment planning, but HPV status, smoking history, and performance status create the complete prognostic picture. Never stage without biology - a T3N2M0 HPV-positive oropharyngeal cancer has better prognosis than T2N1M0 HPV-negative disease.
Understanding the field cancerization concept proves crucial for surveillance strategies. Tobacco and alcohol exposure creates widespread mucosal changes, leading to synchronous primary rates of 5-10% and metachronous primary rates of 3-7% annually.
📌 Remember: SPADE for high-risk synchronous sites - Supraglottic larynx, Pyriform sinus, Aryepiglottic fold, Dorsal tongue, Esophagus. These sites share common carcinogen exposure patterns and require systematic evaluation during staging workup.
The treatment paradigm emphasizes function preservation while maintaining oncological outcomes. Organ preservation protocols achieve larynx preservation rates of 60-70% in advanced laryngeal cancer, though functional outcomes may not always correlate with anatomical preservation.
Connect this foundational understanding through anatomical mastery to understand how precise knowledge of subsites and staging systems enables optimal treatment selection and outcome prediction.
🎯 ENT Oncology: The Head and Neck Cancer Command Center
🗺️ Anatomical Architecture: The Structural Foundation
📌 Remember: ORAL LIPS for oral cavity subsites - Oral tongue, Retromolar trigone, Alveolar ridges, Lips, Lower gum, Inner cheek, Palate (hard), Superior gum. Each subsite demonstrates distinct lymphatic drainage patterns with Level I-III predominance for anterior sites and Level II-IV involvement for posterior locations.
The fascial plane system creates natural barriers and pathways for tumor spread. The superficial layer of deep cervical fascia encases the sternocleidomastoid muscle and trapezius, while the middle layer surrounds the strap muscles and thyroid gland. The deep layer encompasses the prevertebral muscles and forms the danger space posteriorly.
- Critical Fascial Boundaries:
- Superficial fascia: Contains platysma muscle and facial nerve branches
- Deep cervical fascia layers:
- Investing layer: Encases neck muscles and parotid glands
- Carotid sheath: Contains carotid artery, jugular vein, vagus nerve
- Prevertebral fascia: Covers vertebral column and paraspinal muscles
- Buccopharyngeal fascia: Separates pharynx from prevertebral space

The lymphatic drainage system follows predictable patterns that guide staging and treatment decisions. Level-based classification provides systematic approach to neck dissection planning and radiation field design.
| Lymph Node Level | Anatomical Boundaries | Primary Drainage | Risk Sites | Dissection Type |
|---|---|---|---|---|
| Level I | Mandible to hyoid | Oral cavity | Lip, tongue, floor | Selective |
| Level II | Skull base to hyoid | Oropharynx, oral | Tonsil, tongue base | Modified radical |
| Level III | Hyoid to cricoid | Hypopharynx, larynx | Pyriform, vocal cord | Selective |
| Level IV | Cricoid to clavicle | Larynx, hypopharynx | Subglottic, esophagus | Extended |
| Level V | Posterior triangle | Nasopharynx, thyroid | Posterior scalp | Selective |
The laryngeal framework demonstrates complex three-dimensional relationships crucial for voice preservation strategies. The paraglottic space serves as a critical staging landmark, with involvement upgrading T1 to T3 disease and significantly impacting treatment selection.
💡 Master This: Paraglottic space invasion cannot be reliably detected by direct laryngoscopy alone. CT imaging demonstrates >90% accuracy for paraglottic space assessment, while MRI provides superior soft tissue contrast for cartilage invasion evaluation with 85% sensitivity and 95% specificity.
The sinonasal anatomy presents unique challenges due to proximity to critical structures. The cribriform plate thickness averages 0.05-0.15mm, creating high risk for intracranial extension. The sphenoid sinus relationships to carotid arteries and optic nerves demand millimeter-precise surgical planning.
- High-Risk Anatomical Relationships:
- Ethmoid roof: Fovea ethmoidalis weakness points
- Sphenoid sinus: Carotid prominence in 85% of patients
- Maxillary sinus: Infraorbital nerve and dental roots
- Frontal sinus: Frontal recess drainage pathway
📌 Remember: CLOSE for critical sinonasal relationships - Cribriform (intracranial), Lamina papyracea (orbital), Optic nerve (vision), Sphenoid (carotid), Ethmoid (olfactory). Preoperative imaging must identify anatomical variants present in 30-40% of patients.
The thyroid gland anatomy requires understanding of recurrent laryngeal nerve relationships and parathyroid gland locations. Non-recurrent laryngeal nerves occur in 0.5-1% of patients, typically associated with aberrant subclavian arteries.
Understanding tumor growth patterns within anatomical constraints guides margin assessment and reconstruction planning. Perineural invasion follows predictable nerve pathways, while lymphovascular invasion correlates with regional metastatic risk.
Connect this anatomical mastery through staging systems to understand how precise subsite knowledge enables accurate TNM classification and optimal treatment selection.
🗺️ Anatomical Architecture: The Structural Foundation
🎯 Staging Mastery: The Prognostic Precision System
📌 Remember: HPV WINS for oropharyngeal staging changes - HPV-positive gets Whole new system, Improved outcomes, Nodal downstaging, Separate classification. HPV-positive T4N3 disease now stages as Stage II, reflecting 85% 5-year survival compared to 45% for HPV-negative equivalent.
The T-classification system varies significantly across anatomical sites, requiring site-specific expertise for accurate staging. Depth of invasion (DOI) now influences oral cavity T-staging, while laryngeal staging emphasizes vocal cord mobility and cartilage invasion.
- Critical T-Stage Determinants by Site:
- Oral Cavity: Size + DOI (T1: ≤2cm + ≤5mm DOI)
- Oropharynx: Size + extension (T1: ≤2cm, T2: 2-4cm)
- Larynx: Mobility + extension (T1: limited to subsite)
- Hypopharynx: Size + extension (T1: ≤2cm + single subsite)
- Nasopharynx: Extension pattern (T1: nasopharynx only)
The nodal staging revolution reflects improved understanding of metastatic burden and extranodal extension (ENE) significance. Clinical ENE upstages any N-category to N3, while pathological ENE influences adjuvant treatment decisions.
| Site | N1 Criteria | N2 Criteria | N3 Criteria | ENE Impact |
|---|---|---|---|---|
| HPV-Negative | Single ≤3cm | Single 3-6cm or multiple | >6cm or ENE | Upstages to N3 |
| HPV-Positive | ≤4 nodes | >4 nodes | >6cm or ENE | Upstages to N3 |
| Nasopharynx | Unilateral ≤6cm | Bilateral ≤6cm | >6cm or infraclavicular | Upstages to N3 |
| Thyroid | Central compartment | Unilateral lateral | Bilateral or mediastinal | Not applicable |
The M-classification has evolved to include separate categories for distant metastases. M1a designates distant lymph nodes (retropharyngeal, parapharyngeal, or contralateral neck), while M1b indicates true distant metastases to organs.
💡 Master This: Stage migration occurs when improved imaging detects previously occult metastases. PET-CT identifies distant disease in 8-12% of locally advanced cases, changing stage IV classification and treatment intent from curative to palliative.

Prognostic factors beyond TNM staging significantly influence outcomes and treatment decisions. Performance status, smoking history, comorbidity burden, and nutritional status create the complete prognostic picture.
- Key Prognostic Factors:
- HPV Status: Most significant for oropharyngeal cancer
- Smoking History: >10 pack-years worsens HPV-positive prognosis
- Performance Status: ECOG 0-1 vs 2-3 shows 40% survival difference
- Comorbidity: ACE-27 severe reduces 5-year survival by 25%
- Nutritional Status: >10% weight loss indicates poor prognosis
📌 Remember: SMOKE KILLS even HPV-positive tumors - Smoking history >10 pack-years, Mortality increases 2-fold, Outcomes worsen significantly, Keep assessing tobacco use, Educate on cessation benefits. Smoking cessation even during treatment improves survival outcomes.
The staging workup requires systematic approach to ensure accurate classification. Cross-sectional imaging, endoscopic evaluation, and tissue sampling form the diagnostic triad.
Restaging after induction chemotherapy or during surveillance requires understanding of treatment-related changes. Post-radiation fibrosis can mimic residual disease, while pseudoprogression may occur in immunotherapy patients.
Molecular staging represents the future of personalized oncology. Circulating tumor DNA (ctDNA) shows promise for minimal residual disease detection with sensitivity >90% in advanced stage disease.
Connect this staging expertise through treatment algorithms to understand how accurate classification enables optimal therapy selection and outcome prediction.
🎯 Staging Mastery: The Prognostic Precision System
🔬 Diagnostic Excellence: The Clinical Detective Framework
📌 Remember: RED FLAGS for head and neck cancer - Recurrent ulcers >3 weeks, Ear pain (referred otalgia), Dysphagia or odynophagia, Fixed neck mass, Leukoplakia/erythroplakia, Asymmetric tonsillar enlargement, Growth or bleeding lesions, Sore throat >6 weeks. Any symptom >3 weeks in high-risk patients warrants urgent evaluation.
Physical examination requires systematic approach covering all potential primary sites and regional lymph nodes. Bimanual palpation of the oral cavity and indirect laryngoscopy remain fundamental skills, though flexible endoscopy provides superior visualization.
- Systematic Examination Protocol:
- Visual inspection: Lips, oral cavity, oropharynx with adequate lighting
- Palpation: Bimanual examination of tongue, floor of mouth, neck
- Indirect laryngoscopy: Mirror examination or flexible scope
- Cranial nerve assessment: Especially CN V, VII, IX-XII
- Lymph node evaluation: Systematic palpation of all levels
Imaging selection depends on primary site, clinical stage, and treatment planning requirements. Contrast-enhanced CT provides excellent bony detail and nodal assessment, while MRI offers superior soft tissue contrast for skull base and intracranial extension.
| Imaging Modality | Primary Indication | Sensitivity | Specificity | Key Advantages |
|---|---|---|---|---|
| CT with contrast | Initial staging | 85-90% | 80-85% | Bony detail, nodal assessment |
| MRI | Soft tissue detail | 90-95% | 85-90% | Cartilage invasion, perineural spread |
| PET-CT | Distant staging | 95% | 90% | Metabolic activity, unknown primary |
| Ultrasound | Nodal assessment | 80-85% | 95% | Real-time, biopsy guidance |
Tissue diagnosis remains the gold standard for definitive diagnosis. Fine needle aspiration (FNA) provides rapid diagnosis for accessible lesions, while core biopsy offers architectural information and immunohistochemistry options.
💡 Master This: FNA adequacy requires >6 clusters of >10 cells each for reliable interpretation. On-site cytopathology increases adequacy rates from 70% to >95%, reducing repeat procedures and diagnostic delays.

Endoscopic evaluation enables direct visualization, biopsy sampling, and staging assessment. Flexible laryngoscopy should be routine for any voice change, while panendoscopy under anesthesia allows comprehensive evaluation of all mucosal surfaces.
Molecular diagnostics increasingly influence treatment decisions. HPV testing for oropharyngeal cancers uses p16 immunohistochemistry as surrogate marker, while direct HPV testing provides definitive confirmation.
- Essential Molecular Tests:
- p16 IHC: Surrogate for HPV in oropharyngeal cancer
- HPV DNA/RNA: Confirmatory testing when p16 equivocal
- EBV testing: Nasopharyngeal carcinoma association
- Microsatellite instability: Rare but targetable subset
- PD-L1 expression: Immunotherapy selection marker
📌 Remember: p16 POSITIVE doesn't always mean HPV-positive - p16 overexpression occurs in 95% of HPV-positive oropharyngeal cancers but also in 20% of HPV-negative tumors. Confirmatory HPV testing recommended when clinical picture doesn't match p16 status.

Unknown primary workup requires systematic approach when cervical metastases present without obvious primary site. PET-CT identifies primary site in 25-30% of cases, while panendoscopy with directed biopsies finds additional 15-20%.
Staging accuracy directly impacts treatment selection and prognosis. Clinical staging underestimates pathological stage in 20-30% of cases, particularly for nodal disease and depth of invasion.
Multidisciplinary evaluation ensures comprehensive assessment and optimal treatment planning. Tumor boards should include surgical oncology, radiation oncology, medical oncology, pathology, radiology, and supportive care specialists.
Connect this diagnostic mastery through treatment selection to understand how accurate staging and molecular characterization enable personalized therapy approaches and optimal outcomes.
🔬 Diagnostic Excellence: The Clinical Detective Framework
⚔️ Treatment Strategies: The Therapeutic Arsenal
Treatment selection depends on anatomical site, stage, performance status, functional considerations, and patient preferences. The goal remains cure whenever possible, with function preservation as a secondary but critical objective.
📌 Remember: CURE FIRST principle - Complete resection priority, Understand staging completely, Radiation for close margins, Evaluate function preservation, Follow evidence-based protocols, Integrate supportive care, Recognize patient preferences, Systemic therapy when indicated, Team-based decisions.
Surgical approaches vary dramatically by anatomical site and tumor extent. Transoral robotic surgery (TORS) revolutionized oropharyngeal cancer treatment, achieving equivalent oncological outcomes with reduced morbidity compared to open approaches.
- Surgical Options by Site:
- Oral Cavity: Wide local excision with 2cm margins when possible
- Oropharynx: TORS preferred for T1-T2 disease, open for advanced
- Larynx: Partial laryngectomy vs total laryngectomy based on extent
- Hypopharynx: Often requires total laryngectomy with reconstruction
- Thyroid: Lobectomy vs total thyroidectomy based on risk factors

Neck dissection follows evidence-based principles with selective approaches preferred when oncologically appropriate. Sentinel lymph node biopsy shows promise for early oral cavity cancers with negative predictive value >95%.
| Neck Dissection Type | Indications | Levels Removed | Structures Preserved | Morbidity |
|---|---|---|---|---|
| Selective (I-III) | cN0 oral cavity | I, II, III | All non-lymphatic | Minimal |
| Selective (II-IV) | cN0 larynx/hypopharynx | II, III, IV | All non-lymphatic | Low |
| Modified Radical | cN+ disease | I-V | CN XI, IJV, SCM | Moderate |
| Radical | Extensive disease | I-V | None | High |
Radiation therapy serves as definitive treatment for early-stage disease or adjuvant therapy after surgery. Intensity-modulated radiation therapy (IMRT) reduces xerostomia from 90% to 30% compared to conventional techniques.
💡 Master This: Radiation dose follows established protocols - 70 Gy for gross disease, 60 Gy for high-risk areas, 54 Gy for elective nodal regions. Altered fractionation may improve outcomes in selected patients but increases acute toxicity.

Systemic therapy integration continues evolving with immunotherapy showing significant promise. Pembrolizumab demonstrates superior survival compared to standard chemotherapy in recurrent/metastatic disease with PD-L1 expression ≥1%.
Organ preservation strategies aim to maintain function while achieving cure. Larynx preservation protocols achieve organ preservation in 60-70% of advanced laryngeal cancers, though functional outcomes vary significantly.
- Organ Preservation Criteria:
- Adequate performance status (ECOG 0-1)
- Absence of cartilage invasion on imaging
- No significant aspiration at baseline
- Patient motivation for intensive treatment
- Multidisciplinary team agreement
📌 Remember: PRESERVE carefully - Performance status adequate, Response to induction, Evaluate function regularly, Salvage surgery available, Experienced team required, Recognize failure early, Voice outcomes variable, Educate patient thoroughly.
Reconstruction options range from primary closure to complex free flaps. Microvascular reconstruction achieves success rates >95% in experienced centers, enabling aggressive resections with acceptable functional outcomes.

Adjuvant treatment decisions follow evidence-based criteria. Positive margins, extranodal extension, multiple positive nodes, and perineural invasion indicate high-risk features requiring additional therapy.
Treatment toxicity management requires proactive approach. Mucositis, xerostomia, dysphagia, and dermatitis significantly impact quality of life and treatment completion rates.
Immunotherapy represents the most significant advance in systemic therapy for head and neck cancers. Checkpoint inhibitors show activity in both treatment-naive and previously treated patients.
Connect this treatment mastery through outcomes monitoring to understand how systematic follow-up and toxicity management optimize long-term survival and functional outcomes.
⚔️ Treatment Strategies: The Therapeutic Arsenal
🔄 Integration Mastery: The Multidisciplinary Orchestration
Multidisciplinary care improves survival outcomes by 15-20% compared to single-specialty management, while reducing treatment delays and improving patient satisfaction. Tumor boards should meet weekly with mandatory attendance from core specialties.
📌 Remember: TEAM WINS in head and neck oncology - Tumor board essential, Early supportive care, All specialties represented, Multiple treatment options discussed, Weekly meetings scheduled, Integrated care pathways, Nutrition support prioritized, Speech therapy involvement.
Treatment sequencing requires sophisticated understanding of interaction effects between modalities. Surgery-first approaches allow pathological staging to guide adjuvant decisions, while induction chemotherapy may downstage disease and preserve organs.
- Sequencing Considerations:
- Surgery first: Pathological staging guides adjuvant therapy
- Induction chemotherapy: Response assessment predicts organ preservation
- Concurrent chemoradiation: Standard for unresectable disease
- Immunotherapy: Emerging role in neoadjuvant and adjuvant settings
Supportive care integration begins at diagnosis and continues through survivorship. Nutritional support prevents treatment delays in 40% of patients, while speech therapy improves functional outcomes significantly.
| Supportive Care Service | Timing | Key Interventions | Outcome Impact |
|---|---|---|---|
| Nutrition | Pre-treatment | PEG tube placement | Reduces delays 40% |
| Speech Therapy | Pre/post treatment | Swallow assessment | Improves function 60% |
| Social Work | At diagnosis | Resource coordination | Reduces anxiety 50% |
| Palliative Care | Advanced disease | Symptom management | Improves QOL 70% |
Quality metrics guide program development and outcome improvement. Time to treatment initiation should be <30 days from diagnosis, while multidisciplinary evaluation should occur within 2 weeks.
💡 Master This: Treatment delays >60 days from diagnosis increase mortality risk by 10-15% for locally advanced disease. Navigation programs reduce time to treatment by average 12 days while improving patient satisfaction scores.
Molecular integration increasingly influences treatment decisions. HPV status determines staging system, treatment intensity, and surveillance strategies for oropharyngeal cancers.
Survivorship care addresses long-term sequelae affecting >80% of head and neck cancer survivors. Xerostomia, dysphagia, hearing loss, and dental complications require ongoing management.
- Long-term Complications:
- Xerostomia: 90% of radiation patients, permanent in 60%
- Dysphagia: 70% of chemoradiation patients, severe in 25%
- Hearing loss: 40% with cisplatin-based therapy
- Dental complications: 80% require ongoing dental care
- Hypothyroidism: 50% after neck radiation
📌 Remember: SURVIVE WELL requires comprehensive planning - Surveillance protocols, Understand late effects, Rehabilitation services, Vaccination updates, Integrated dental care, Vitamin D monitoring, Endocrine assessment, Weight management, Emotional support, Lifestyle modifications, Long-term follow-up.
Recurrence detection requires systematic surveillance with physical examination every 3-4 months for first 2 years, then every 6 months until year 5. Imaging should be symptom-directed rather than routine.
Second primary prevention involves tobacco cessation, alcohol moderation, and HPV vaccination for appropriate candidates. Annual chest imaging detects lung primaries in high-risk patients.
Emerging therapies continue expanding treatment options. CAR-T cell therapy, oncolytic viruses, and novel immunotherapy combinations show promising early results in refractory disease.
Patient-reported outcomes increasingly guide treatment decisions and quality improvement. Functional assessment tools help optimize treatment selection and supportive care interventions.
Connect this integration mastery through advanced concepts to understand how cutting-edge research and personalized medicine approaches continue revolutionizing head and neck cancer care.
🔄 Integration Mastery: The Multidisciplinary Orchestration
🚀 Advanced Frontiers: The Precision Medicine Revolution
Precision medicine in head and neck oncology extends far beyond HPV status, incorporating comprehensive genomic profiling, tumor microenvironment analysis, and host factors to guide treatment selection. Next-generation sequencing identifies actionable mutations in 15-20% of head and neck cancers.
📌 Remember: PRECISION CARE transforms outcomes - Profiling tumor genetics, Recognize actionable targets, Evaluate tumor microenvironment, Circulating biomarkers, Immune checkpoint status, Select optimal therapy, Individualize treatment plans, Ongoing monitoring, New trial opportunities.
Immunotherapy represents the most significant therapeutic advance in decades. Pembrolizumab demonstrates superior survival compared to standard chemotherapy in recurrent/metastatic disease, with median overall survival improving from 10.1 months to 14.9 months.
- Immunotherapy Landscape:
- PD-1 inhibitors: Pembrolizumab, Nivolumab - first-line and recurrent disease
- PD-L1 inhibitors: Durvalumab, Atezolizumab - combination strategies
- CTLA-4 inhibitors: Ipilimumab - combination with PD-1
- Novel targets: LAG-3, TIM-3, TIGIT - under investigation
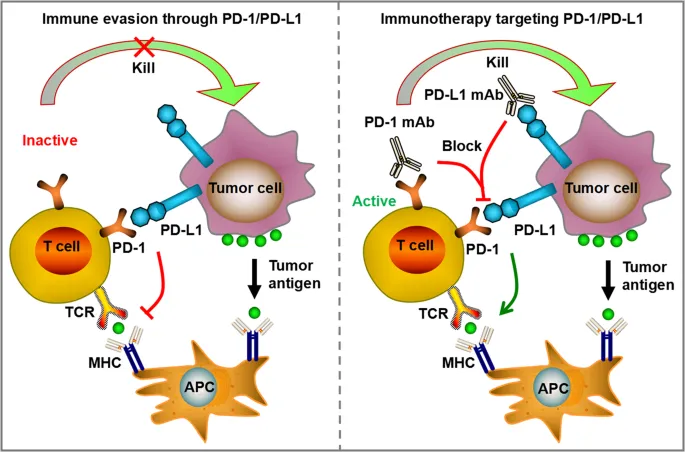
Biomarker development guides treatment selection with increasing precision. PD-L1 expression, tumor mutational burden (TMB), microsatellite instability (MSI), and immune signatures predict immunotherapy response.
| Biomarker | Predictive Value | Testing Method | Clinical Application |
|---|---|---|---|
| PD-L1 CPS ≥1 | Response rate 19% vs 14% | IHC 22C3 | Pembrolizumab selection |
| TMB-High | Response rate 35% vs 16% | NGS panel | Investigational |
| MSI-High | Response rate 60% | IHC/PCR | Pembrolizumab approved |
| HPV Status | De-escalation trials | p16 IHC | Treatment modification |
Liquid biopsies using circulating tumor DNA (ctDNA) enable real-time monitoring of treatment response and minimal residual disease. ctDNA detection after curative treatment predicts recurrence with lead time of 2-6 months before imaging detection.
💡 Master This: ctDNA kinetics during treatment predict outcomes better than static measurements. Rapid clearance within 4 weeks correlates with complete response, while persistent elevation suggests treatment resistance requiring strategy modification.

Artificial intelligence applications span diagnosis, treatment planning, and outcome prediction. Deep learning algorithms achieve >95% accuracy for lymph node metastasis detection on imaging, while radiomics predicts treatment response with 85% accuracy.
Novel therapeutic targets continue emerging from genomic studies. FGFR inhibitors show activity in FGFR-altered tumors (10-15% of cases), while CDK4/6 inhibitors demonstrate synergy with immunotherapy.
- Emerging Targets:
- FGFR1-3 amplifications: Pemigatinib, Erdafitinib
- PIK3CA mutations: Alpelisib combinations
- NOTCH1 mutations: Gamma-secretase inhibitors
- DNA repair defects: PARP inhibitors
- Angiogenesis: Bevacizumab combinations
📌 Remember: TARGET SMART for precision therapy - Tumor profiling essential, Actionable mutations identified, Resistance mechanisms understood, Guideline-based selection, Emerging targets evaluated, Trial opportunities considered, Sequencing strategies optimized, Monitoring response closely, Adaptive treatment plans, Resistance profiling, Team-based decisions.
Combination strategies maximize therapeutic benefit while managing toxicity. Immunotherapy plus chemotherapy shows superior outcomes compared to chemotherapy alone in first-line treatment of recurrent/metastatic disease.
Treatment de-escalation trials aim to reduce toxicity while maintaining efficacy in favorable-risk patients. HPV-positive oropharyngeal cancers with excellent prognosis may benefit from reduced-intensity treatment.
Radiotherapy innovations include proton therapy, stereotactic body radiation, and MR-guided radiation. Proton therapy reduces integral dose by 30-50%, potentially decreasing long-term toxicity.
Surgical innovations continue improving outcomes and reducing morbidity. Transoral laser microsurgery, robotic surgery, and image-guided surgery enable precise resections with better functional preservation.
Regenerative medicine approaches address treatment-related toxicity. Stem cell therapy for radiation-induced xerostomia and tissue engineering for reconstruction show promising early results.
Patient stratification using multi-omics approaches enables personalized treatment selection. Integration of genomics, proteomics, metabolomics, and clinical factors creates comprehensive risk models.
This advanced understanding positions head and neck oncology at the forefront of precision medicine, where molecular insights drive individualized treatment strategies and dramatically improve patient outcomes.
🚀 Advanced Frontiers: The Precision Medicine Revolution
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app












