TMJ Anatomy & Biomechanics - Joint Journey
- Key Structures: Mandibular condyle, glenoid fossa (temporal bone), articular disc (biconcave fibrocartilage).
- Ligaments: Temporomandibular, sphenomandibular, stylomandibular.
- Muscles of Mastication: 📌 Masseter, Temporalis, Medial pterygoid, Lateral pterygoid.
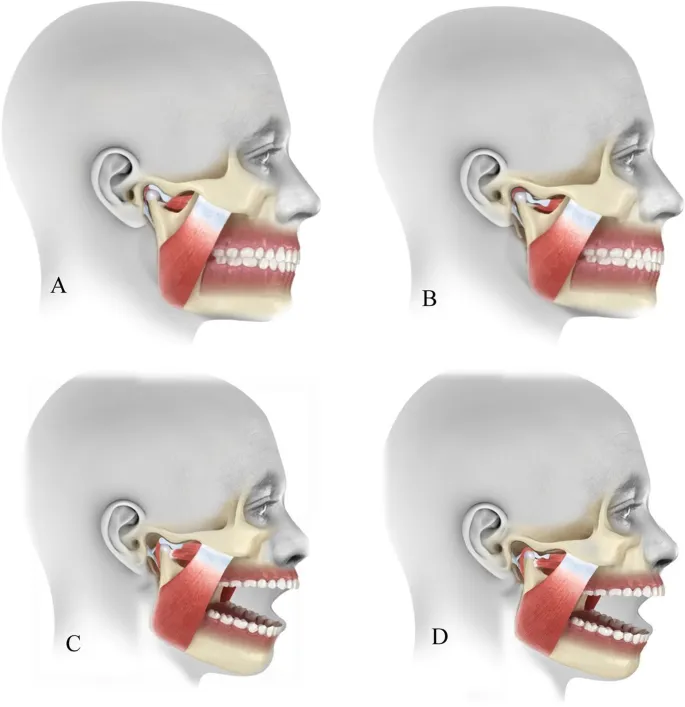
- TMJ Movements:
- Elevation (closing): Temporalis, Masseter, Medial pterygoid.
- Depression (opening): Lateral pterygoid (inf. head), suprahyoids.
- Protrusion: Lateral pterygoids (bilateral).
- Retrusion: Temporalis (post. fibers), Masseter (deep fibers).
- Lateral Excursion: Contralateral pterygoids, ipsilateral temporalis.
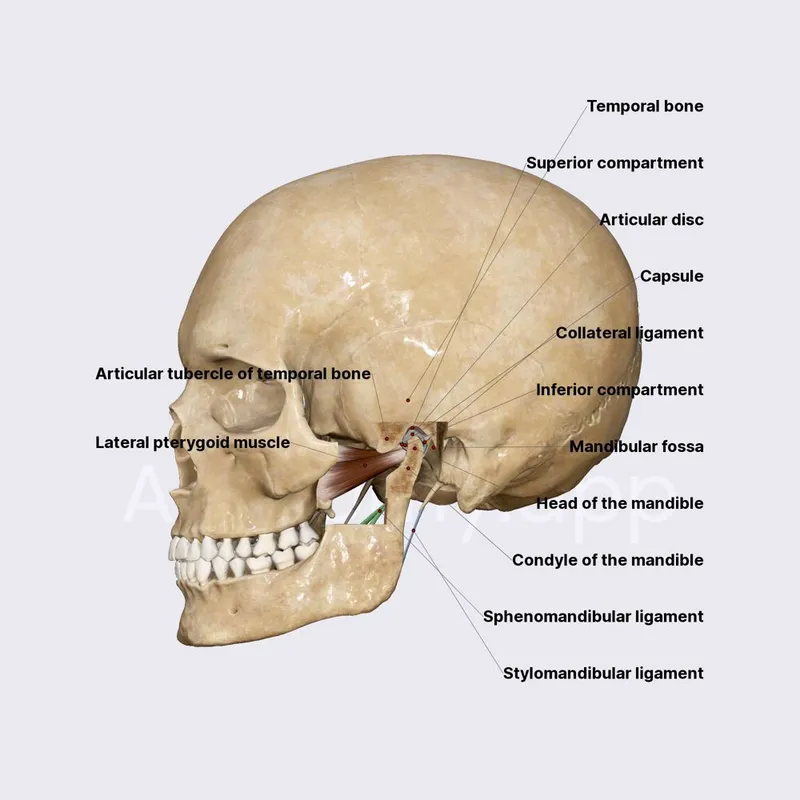
⭐ The TMJ is a ginglymoarthrodial joint, allowing both hinge (ginglymoid) and gliding (arthrodial) movements.
TMD Etiology & Classification - Jaw Pain Origins
Etiology: Multifactorial, often unclear. Key contributors:
- Trauma (e.g., whiplash, direct blow)
- Parafunctional habits (bruxism, clenching)
- Psychosocial factors (stress, anxiety)
- Systemic diseases (e.g., Rheumatoid Arthritis)
- Occlusal disharmony (role debated)
Classification:
- Myofascial Pain & Dysfunction (MPD): Most common; muscle tenderness, pain, limited motion.
⭐ Myofascial pain and dysfunction (MPD) is the most common form of TMD.
- Internal Derangements (ID): Articular disc issues; clicking, locking, pain.
- Disc displacement with reduction (DDWR)
- Disc displacement without reduction (DDWOR)
- Adhesions
- Degenerative Joint Disease (DJD): Osteoarthritis, osteoarthrosis; crepitus, pain.
- Other: Inflammatory (synovitis, capsulitis), chronic recurrent dislocation, ankylosis.
TMD Symptoms & Diagnosis - Crackle, Lock, Diagnose
Symptoms:
- Preauricular pain, pain on mastication.
- Joint sounds: Clicking, popping, crepitus.
- Limited mouth opening/locking.
- Normal: 40-50 mm; Restricted: <35 mm.
- Jaw deviation on opening.
- Headache (temporal region).
- Ear symptoms: Otalgia, tinnitus, dizziness. 📌 (Mnemonic: "Painful Clicks Lock Dizzy Heads")
Diagnosis:
- History: Symptom details (onset, nature, triggers).
- Clinical Examination:
- Palpation: TMJ & masticatory muscle tenderness.
- ROM Assessment: Measure opening, lateral, protrusive movements.
- Auscultation: Joint sounds.
- Occlusal analysis.
- Imaging:
- OPG/Panoramic X-ray: Gross bony changes.
- CT: Detailed bony anatomy (e.g., condylar erosion, ankylosis).
- MRI: ⭐ Gold standard for disc position, soft tissues, inflammation.
⭐ MRI is the gold standard imaging modality for assessing articular disc position and integrity in TMDs.

TMD Management Approaches - Unlocking Comfort
Management is phased, prioritizing least invasive options to restore jaw function & pain relief.
- Conservative (Phase 1): Initial TMD care.
- Patient education, jaw rest (e.g., avoiding wide opening), soft diet.
- Physiotherapy: Includes heat/cold application, specific jaw exercises, TENS.
- Pharmacotherapy:
- NSAIDs (e.g., Ibuprofen 400-600 mg TID) for analgesia/anti-inflammatory effects.
- Muscle relaxants for acute spasms.
- Anxiolytics/TCAs for chronic pain conditions or associated bruxism.
- Occlusal splints: Stabilization splint (provides joint stability), anterior repositioning splint (guides condyle).
⭐ Over 80% of TMD patients improve with conservative, non-surgical management.
-
Minimally Invasive (Phase 2): If Phase 1 fails.
- Arthrocentesis: Joint lavage to remove inflammatory byproducts.
- Arthroscopy: Diagnostic visualization and operative interventions (e.g., adhesiolysis).
- Botox injections: For Myofascial Pain Dysfunction (MPD).
-
Surgical (Phase 3): Reserved for severe, structurally altered, and refractory cases.
- Open joint surgery: Arthroplasty, discectomy, disc repair/repositioning, condylotomy.
- Total Joint Replacement (TJR): End-stage cases.
High‑Yield Points - ⚡ Biggest Takeaways
- TMJ pain, clicking/popping sounds, and restricted jaw movement are key symptoms.
- Myofascial Pain Dysfunction Syndrome (MPDS) is most common, often linked to bruxism and stress.
- Internal derangement involves anterior disc displacement; with reduction (click), without reduction (closed lock).
- Conservative management (soft diet, NSAIDs, physiotherapy) is the first-line treatment approach.
- MRI is the gold standard for evaluating disc position and associated soft tissues.
- Arthrocentesis can be therapeutic for acute closed lock unresponsive to conservative measures.
- Deviation on opening is towards the affected side in unilateral condylar hypomobility or disc displacement without reduction.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

