Ranula: Definition, Types & Etiopathogenesis - Frog Under Tongue
- Definition:
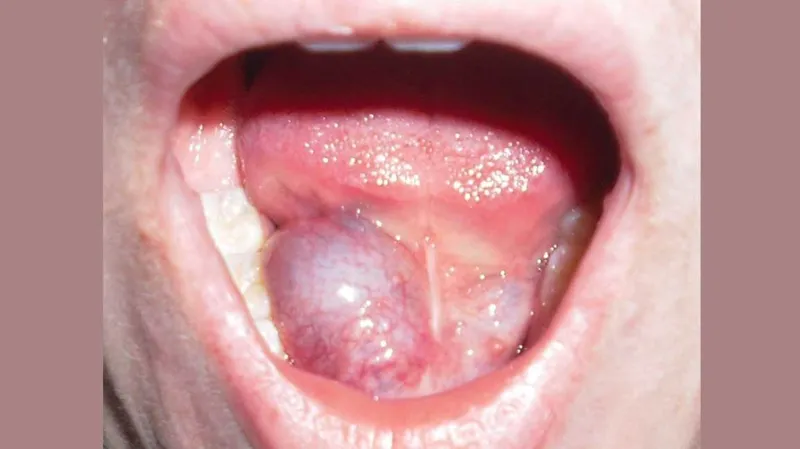
- Mucocele on floor of mouth, from sublingual gland (common) or minor salivary glands.
- Appearance: Bluish, translucent, fluctuant swelling.
- 📌 "Rana" = frog (resembles frog's belly).
- Types:
- Oral (Simple):
- Above mylohyoid muscle, confined to mouth floor. Most common.
- Plunging (Cervical):
- Extends through mylohyoid into neck (submandibular space).
- May be neck mass +/- oral swelling. "Tail sign" on imaging (CT/MRI).
- Oral (Simple):
- Etiopathogenesis:
- Extravasation (Most Common): Trauma → mucus spillage → pseudocyst (no epithelial lining).
- Retention (Rare): Duct obstruction → ductal dilation → true cyst (epithelial lining).
⭐ Most ranulas originate from the sublingual gland and are pseudocysts due to mucus extravasation following trauma.
Ranula: Clinical Features & Diagnosis - Spotting the Swell
- Clinical Presentation:
- Oral Ranula:
- Soft, fluctuant, dome-shaped, bluish, translucent swelling.
- Location: Floor of mouth, lateral to midline.
- 📌 "Frog's belly" appearance (rana = frog).
- Usually painless; large ones may cause speech/swallowing issues.
- Plunging/Cervical Ranula:
- Extends into neck via mylohyoid muscle defect/dehiscence.
- Presents as soft, painless neck mass; oral component variable.
- Oral Ranula:
- Diagnostic Approach:
- Clinical Exam: Characteristic appearance & consistency. Transillumination often positive. Bimanual palpation for plunging type.
- Imaging:
- USG: Initial assessment for cystic nature & superficial extent.
- CT/MRI: Define full extent, especially for plunging type, and relation to mylohyoid muscle.
- "Tail sign" (fluid extension from sublingual space) is a key diagnostic feature of plunging ranula.
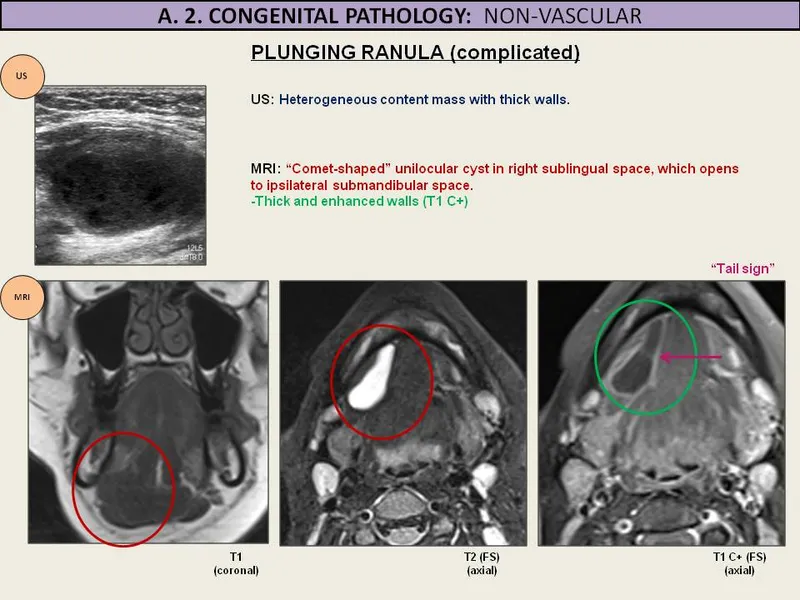
- "Tail sign" (fluid extension from sublingual space) is a key diagnostic feature of plunging ranula.
- Fine Needle Aspiration (FNA):
- Yields viscous, mucoid, straw-colored (salivary) fluid.
- Biochemistry: ↑ Amylase, ↓ protein content.
- Histopathology (post-excision): Confirms pseudocyst (lacks true epithelial lining; wall of granulation/fibrous tissue).
⭐ The "tail sign" on CT or MRI, representing the extension of the ranula from the sublingual space into the submandibular or parapharyngeal space posterior to the mylohyoid muscle, is a key diagnostic feature of plunging ranulas originating from the sublingual gland.
Ranula: Management & Differential Diagnosis - Evicting the Frog
Management
- Surgical Options:
- Marsupialization: Creates a pouch; high recurrence.
- Excision of Ranula: Removal of the cyst.
- Excision of Sublingual Gland (± Ranula): Gold standard, lowest recurrence, especially for plunging ranulas.
- Sclerotherapy: OKP-432 (Picibanil), bleomycin.
- CO2 Laser: Vaporization or excision.
Differential Diagnosis (DDx)
- Floor of Mouth Swellings:
- Dermoid cyst / Epidermoid cyst
- Sublingual abscess
- Hemangioma / Lymphangioma
- Lipoma
- Salivary gland neoplasm (rare in sublingual gland)
- Cystic hygroma (especially for plunging ranula)
- Thyroglossal duct cyst (if midline & plunging)
- Branchial cleft cyst (2nd arch, if lateral cervical)
⭐ Exam Favourite: Complete excision of the ipsilateral sublingual gland is the definitive treatment with the lowest recurrence rate for both oral and plunging ranulas.
📌 Mnemonic for DDx: "Real Doctors Hate Lame Students Crying"
- Ranula
- Dermoid/Epidermoid cyst
- Hemangioma/Lymphangioma
- Lipoma
- Sublingual abscess/Sialolithiasis
- Cystic hygroma/Neoplasm
High‑Yield Points - ⚡ Biggest Takeaways
- A ranula is a mucocele specifically from the sublingual gland, appearing as a bluish swelling in the floor of the mouth.
- Plunging ranulas dissect through the mylohyoid muscle into the neck.
- Histologically, it's a pseudocyst (lacks an epithelial lining).
- Treatment includes marsupialization, excision of the ranula, or excision of the sublingual gland.
- Often painless; may become symptomatic if large or infected.
- Consider dermoid cyst and lymphangioma in differential diagnosis_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

