Oral Leukoplakia - White Patch Basics
- Clinically white patch/plaque; cannot be scraped off.
- WHO: Not characterized as any other definable lesion.
- Most common oral potentially malignant disorder (OPMD).
- Etiology: Tobacco (smoking/smokeless) primary; alcohol, HPV.
- Types: Homogenous (uniform, lower risk), Non-homogenous (speckled, nodular, verrucous - higher malignant potential).
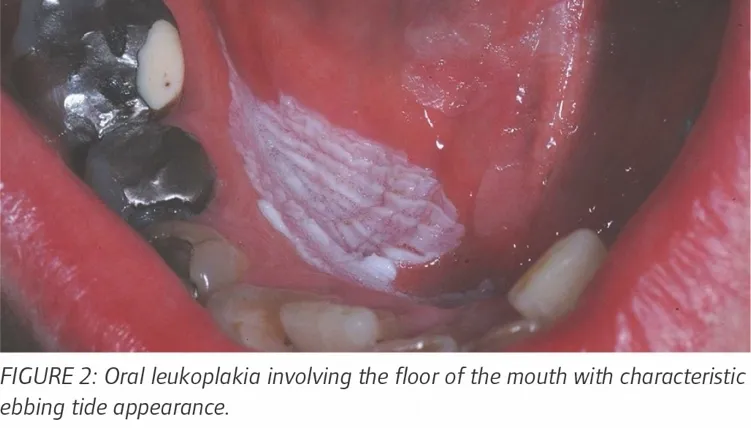
⭐ Non-homogenous leukoplakia has a significantly higher risk of malignant transformation (4-7 times greater than homogenous).
Leukoplakia Risks - Culprits & Causes
- Tobacco: Key etiological factor (smoking, smokeless forms like gutka, khaini). Dose & duration dependent.
- Alcohol: Synergistic with tobacco, ↑ risk significantly.
- Chronic Irritation: Dental factors (e.g., sharp cusps, rough restorations, ill-fitting dentures).
- Infections:
- Candida albicans (especially in non-homogenous/speckled types).
- HPV (Human Papillomavirus, notably types 16, 18).
- Nutritional Deficiencies: Vitamins A, B complex.
- Idiopathic: No known cause in ~20% of cases.
⭐ Proliferative verrucous leukoplakia (PVL) has a very high malignant transformation rate, often >70%.
Leukoplakia Looks - Spotting the Signs

- Clinical Sign: Persistent, adherent white patch/plaque; cannot be scraped off.
- Types & Malignant Potential:
- Homogeneous: Uniform, flat, thin; may be smooth/wrinkled. Lower risk.
- Non-homogeneous (Higher risk):
- Speckled (Erythroleukoplakia): Mixed red & white.
- Nodular: Small, raised granules/nodules.
- Verrucous: Warty, exophytic projections.
- High-Risk Sites:
- Floor of mouth
- Ventrolateral tongue
- Soft palate complex
- Lip vermilion
⭐ Erythroleukoplakia (speckled non-homogeneous type) has the highest malignant transformation rate.
Leukoplakia Diagnosis - Biopsy Unveiled
- Mandatory Biopsy: Confirms diagnosis; crucial for assessing dysplasia.
- Key Differentials: Lichen planus, candidiasis, frictional keratosis, squamous cell carcinoma (SCC).
- Histopathology:
- Hyperkeratosis (ortho- or parakeratosis), acanthosis.
- Epithelial Dysplasia Grading (WHO criteria):
- Mild: Changes in basal 1/3 of epithelium.
- Moderate: Changes extend to middle 1/3 (basal 2/3).
- Severe: Changes extend to superficial 1/3 (>2/3).
- Carcinoma in situ (CIS): Full-thickness atypia, intact basement membrane.
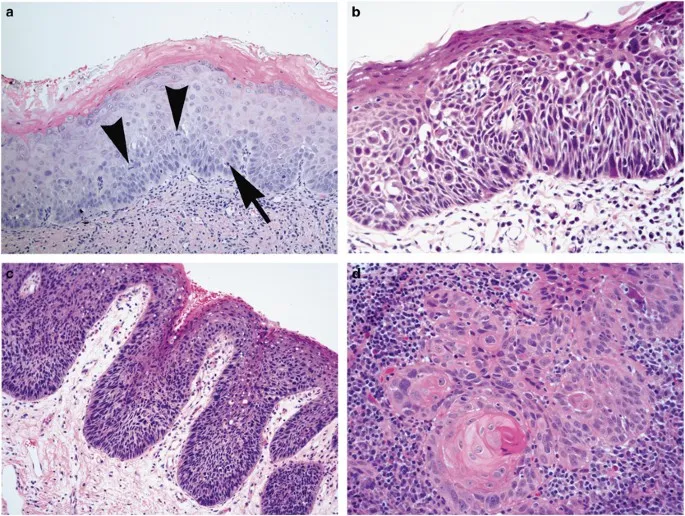
⭐ Non-homogeneous leukoplakia (e.g., speckled, nodular, verrucous) has a significantly higher malignant transformation risk (4-7 times) compared to homogeneous leukoplakia. This is a critical prognostic indicator for NEET PG.
Leukoplakia's Danger - Cancer Connection
- Most common oral premalignant lesion; risk of SCC.
- Malignant transformation rate: 1-20%; overall ~4%.
- Factors ↑ risk of malignant change:
- Lesion persistence (e.g., > 10 years).
- Female gender, non-smoker status.
- High-risk sites: floor of mouth, ventrolateral tongue, soft palate.
- Non-homogeneous appearance (speckled, nodular, verrucous).
- Presence and severity of epithelial dysplasia on biopsy.
⭐ Epithelial dysplasia is the single most important predictor of malignant transformation.
Managing Leukoplakia - Treatment Paths
- Aim: Manage dysplasia, reduce malignant transformation risk.
- Initial:
- Cease risk factors (tobacco, alcohol).
- Mandatory biopsy for grading.
- Treatment:
- No/Mild Dysplasia: Observe, control risks, review regularly.
- Mod/Severe Dysplasia: Surgical excision (scalpel, laser), cryotherapy.
- Follow-up: Lifelong surveillance critical.
⭐ High recurrence (up to 35%) post-treatment mandates vigilant, long-term follow-up for recurrence or malignant change.
High-Yield Points - ⚡ Biggest Takeaways
- Oral leukoplakia: white patch/plaque on oral mucosa, cannot be scraped off, not otherwise classifiable.
- It's a premalignant lesion; risk of transformation to squamous cell carcinoma (SCC).
- Tobacco use (smoking/smokeless) is the primary etiological factor.
- Non-homogeneous types (speckled, nodular) carry ↑ malignant risk than homogeneous type.
- Biopsy is mandatory for diagnosis and to assess for dysplasia or carcinoma.
- Management: stop risk factors (tobacco, alcohol), long-term follow-up; excision for dysplastic lesions.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

