Oral Cancers - The Mouth's Malignancy
- Malignant neoplasms of oral cavity; >90% are Squamous Cell Carcinoma (SCC).
- India: High burden due to tobacco, areca nut, alcohol.
- Risks (📌 Mnemonic: TAB-H): Tobacco, Alcohol, Betel quid, HPV (16, 18), chronic irritation.
- Signs: Non-healing ulcer, growth, pain, trismus, red/white patches (leukoplakia/erythroplakia).
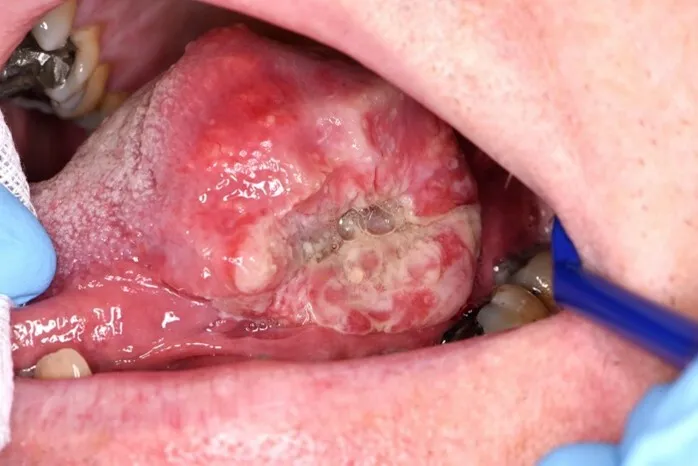
⭐ In India, buccal mucosa is the most common site for oral SCC, strongly linked to betel quid chewing practices.
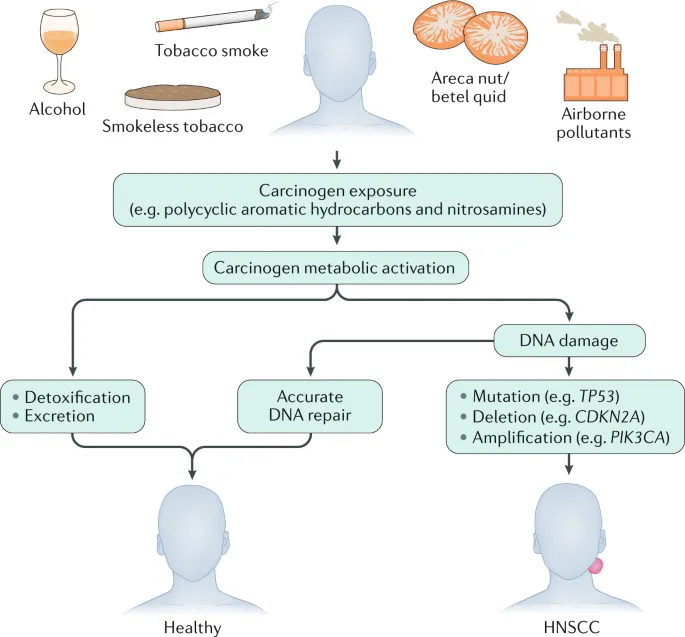
Culprits & Causes - Risky Business
- Tobacco: Dominant factor; single most important cause.
- Smoking (cigarettes, bidis, hookah).
- Smokeless (khaini, gutkha, pan masala, zarda).
- Alcohol: Potent co-carcinogen, especially with tobacco.
⭐ Tobacco + Alcohol = Synergistic effect, dramatically ↑ risk (multiplicative, not additive).
- Areca Nut (Supari): Key independent carcinogen; common in betel quid/pan.
- Human Papillomavirus (HPV): Primarily types 16 & 18; more common in oropharyngeal cancers but also oral.
- Chronic Irritation: Sharp teeth, ill-fitting dentures, poor oral hygiene.
- Dietary Deficiencies: Low intake of fruits/vegetables (↓ Vitamins A, C, E, iron).
- Genetic Predisposition: e.g., Plummer-Vinson syndrome, Fanconi anemia.
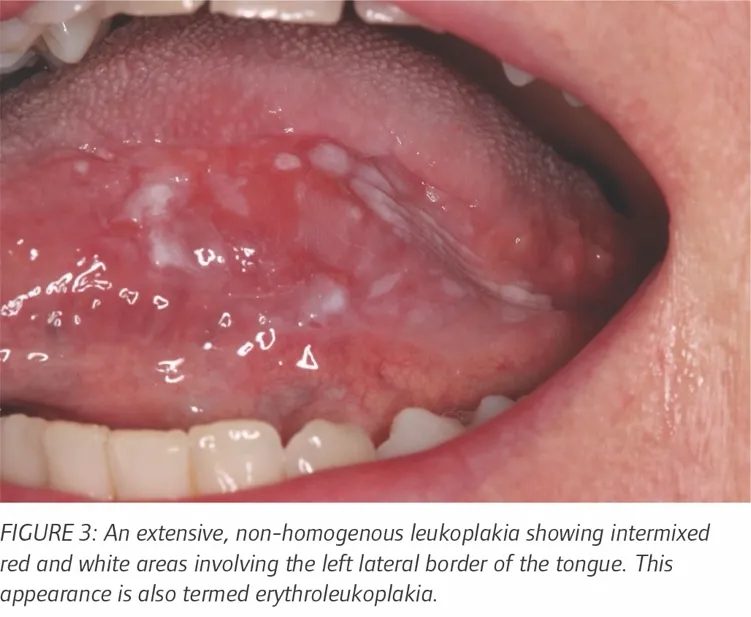
Spotting the Signs - Lesion Location Logic
- High-Risk Zones: Tongue (posterolateral), floor of mouth (FOM), retromolar trigone.
- Tongue: Lateral border (most common), ventral. Base of tongue often advanced at diagnosis.
- Floor of Mouth: Anteriorly; common site for midline spread.
- Buccal Mucosa: Along occlusal line; strong tobacco/betel quid association.
- Lip: Lower lip vermilion (sun exposure); generally best prognosis.
- Gingiva: May mimic periodontitis or epulis; check for underlying bone invasion.
- Palate: Hard palate (often minor salivary gland tumors), soft palate.
⭐ Squamous Cell Carcinoma (SCC) of the lower lip vermilion typically carries the best prognosis among oral cavity cancers due to early detection and less aggressive behavior.
Diagnosis & Staging - Sizing Up the Foe
- Biopsy: Gold standard. Incisional (lesion edge); excisional (small lesions <1 cm).
- FNAC: For neck nodes.
- Imaging:
- CT (Contrast): Bone, neck nodes.
- MRI: Soft tissue, perineural spread.
- PET-CT: Distant mets, recurrence.
- Staging: AJCC TNM (8th ed.).
- T: Size & Depth of Invasion (DOI).
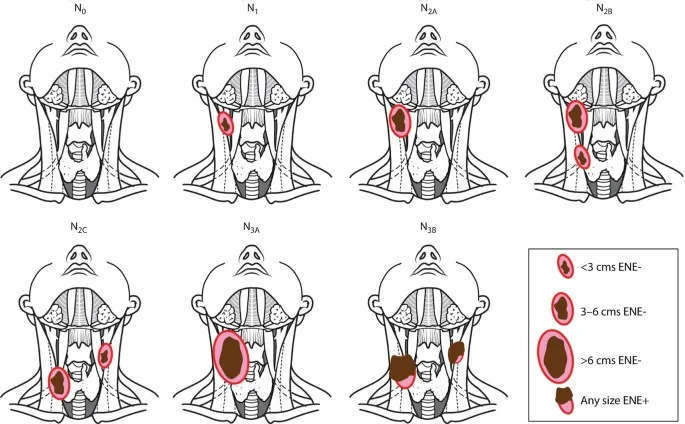
- N: Nodes (size, number, ENE+).
- M: Metastasis.
⭐ Depth of Invasion (DOI) critically impacts T-stage & prognosis in oral SCC.
 oka
oka
Treatment Tactics - Battling the Blaze
- Primary Goal: Cure; preserve function & QoL.
- Core Modalities: Surgery (Sx), Radiotherapy (RT), Chemotherapy (CT), Immunotherapy.
- Strategy: Stage-dependent.
- Neck: Elective Neck Dissection (END) if cN0 & >20% occult mets risk.
⭐ Adjuvant RT: 60-66 Gy. CTRT for high-risk (positive margins, ENE).
Prevention & Prognosis - Outlook & Ounce of Prevention
- Prevention:
- Primary: Avoid tobacco (all forms), betel quid, excessive alcohol.
- Secondary: Early detection via dental exams, oral self-awareness.
- Consider HPV vaccination for high-risk groups.
- Prognosis:
- Strongly linked to TNM stage at diagnosis.
- 5-year survival rates:
- Stage I/II: ~70-90%
- Stage III/IV: ~20-50%
- Overall 5-year survival: ~60-65%.
⭐ Cervical node involvement: most critical adverse prognostic factor.
High‑Yield Points - ⚡ Biggest Takeaways
- Squamous Cell Carcinoma (SCC) is the most common oral cancer, accounting for over 90% of cases.
- Primary risk factors include tobacco (smoked and smokeless), areca nut (betel quid), and alcohol.
- Commonest sites are the lateral border of the tongue and buccal mucosa (especially in India due to chewing habits).
- Key premalignant lesions: leukoplakia, erythroplakia (highest malignant potential), and Oral Submucous Fibrosis (OSMF).
- A non-healing ulcer or an unexplained red/white patch are the most common early symptoms.
- Biopsy is essential for diagnosis; treatment is typically multimodal involving surgery, radiotherapy, and/or chemotherapy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

