Poxviruses Overview - Brick-Shaped Invaders
- General: Largest DNA viruses; brick-shaped with complex internal structure.
- Cytoplasmic Replication:
⭐ Poxviruses are the only DNA viruses that replicate entirely within the cytoplasm, a unique trait.
- Inclusions: Produce characteristic intracytoplasmic inclusion bodies.
- Key Genera (Chordopoxvirinae):
- Orthopoxvirus: Variola (smallpox), vaccinia, cowpox, mpox.
- Parapoxvirus: Orf, milker's nodules.
- Molluscipoxvirus: Molluscum contagiosum.
- Yatapoxvirus: Tanapox, Yaba monkey tumor virus.

Molluscum Contagiosum - Pearly Pimple Parade
- Etiology: Molluscum Contagiosum Virus (MCV), a Molluscipoxvirus (MCV-1 most common).
- Transmission: Direct skin-to-skin contact, fomites, autoinoculation. Sexual transmission common in adults.
- Clinical Features:
- Firm, pearly, flesh-colored to pink, dome-shaped papules (2-5 mm) with central umbilication.
- Henderson-Paterson bodies: Intracytoplasmic eosinophilic inclusion bodies containing virions.
- Common Sites:
- Children: Trunk, extremities, face.
- Adults: Genitals, lower abdomen, inner thighs.
- Immunocompromised (e.g., HIV): Numerous, larger, persistent, atypical lesions (giant molluscum, facial involvement).

- Diagnosis: Primarily clinical. Biopsy/smear shows Henderson-Paterson bodies.
- Treatment: Often self-limiting. Options: Curettage, cryotherapy, cantharidin, podophyllotoxin, imiquimod, salicylic acid. Treat underlying immunosuppression.
⭐ Henderson-Paterson bodies are pathognomonic intracytoplasmic inclusions seen in Molluscum Contagiosum.
Orf & Milker's Nodule - Farmyard Pox Pals
⭐ Orf: 6 clinical stages; targetoid/iris lesion common in acute phase.

| Feature | Orf (Contagious Ecthyma) | Milker's Nodule (Pseudocowpox) |
|---|---|---|
| Virus | Parapoxvirus | Parapoxvirus |
| Animal Reservoir | Sheep, goats | Cattle (cow udders) |
| Transmission | Direct contact (animals, fomites) | Direct contact (animals, fomites) |
| Clinical Lesion | Single/few; hands/fingers. 6 stages (maculopapular → targetoid → weeping → nodular → papillomatous → regressive). | 1-5 firm, reddish-blue, non-umbilicated papules/nodules; hands. |
| Systemic Symptoms | Usually mild/absent; low-grade fever, malaise. | Usually mild/absent; low-grade fever, malaise. |
| Complications | Secondary infection, Erythema Multiforme (esp. Orf), lymphangitis. | Secondary infection, Erythema Multiforme, lymphangitis. |
| Diagnosis | Clinical, history. EM (ovoid virions, criss-cross). PCR. | Clinical, history. EM (ovoid virions, criss-cross). PCR. |
| Management | Self-limiting (4-6 wks). Symptomatic, wound care. | Self-limiting (4-6 wks). Symptomatic, wound care. |
Mpox (Monkeypox) - Global Alert Pox
- Etiology: Mpox virus (MPXV), Orthopoxvirus. Clades: I (severe), II (milder, 2022+ global outbreak).
- Transmission: Zoonotic (rodents, primates). Human-to-human: direct contact (lesions, fluids), respiratory (prolonged), fomites. Vertical possible.
- Clinical Features:
- Incubation: 5-21 days. Prodrome (1-5 days): fever, headache, lymphadenopathy (key vs smallpox), myalgia.
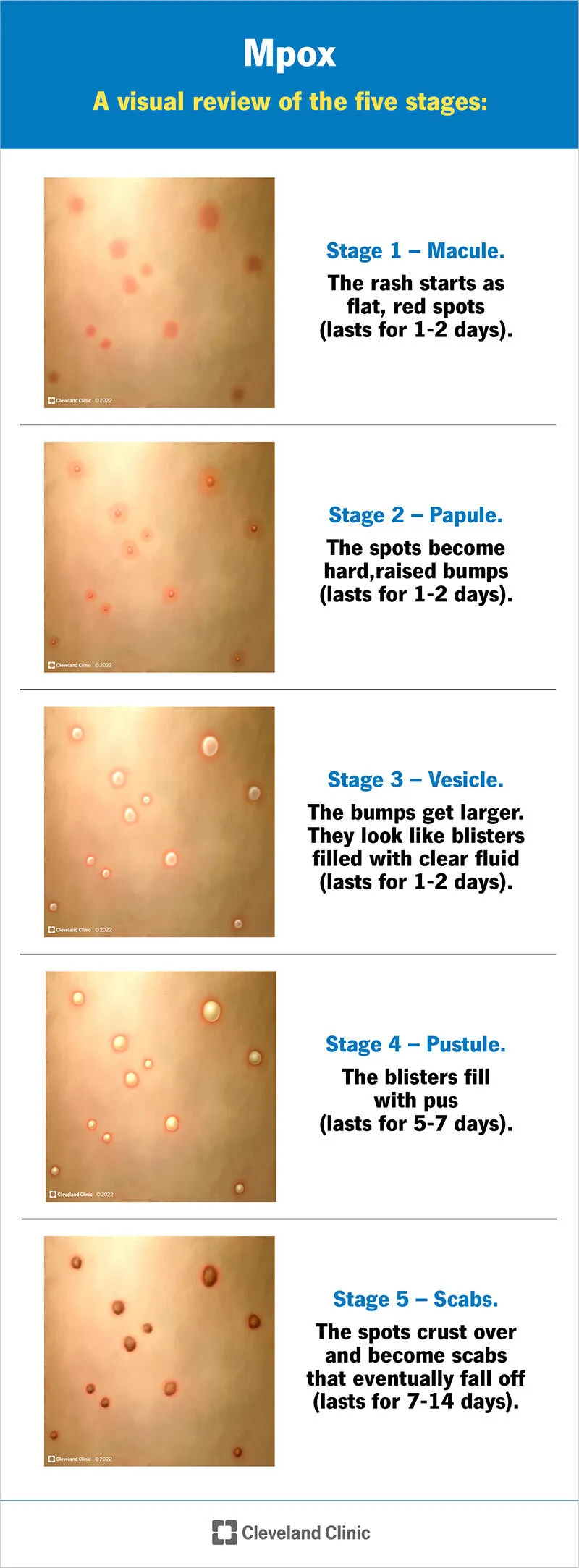
- Rash (1-3 days post-fever): Evolves: macules → papules → vesicles → pustules → crusts. Centrifugal or genital/perianal/localized. Painful.
- Diagnosis: PCR of lesion material.
- Management: Supportive care. Tecovirimat for severe cases/immunocompromised. Vaccinia Immune Globulin (VIGIV).
- Prevention: Smallpox vaccines (e.g., JYNNEOS) for Pre-Exposure Prophylaxis (PrEP)/Post-Exposure Prophylaxis (PEP). Avoid contact.
⭐ Prominent lymphadenopathy is a characteristic feature of Mpox, helping distinguish it from smallpox where it is typically absent.
Smallpox & Vaccinia - Eradicated & Engineered
- Smallpox (Variola Virus - Orthopoxvirus)
- Eradicated 1980 (WHO).
- Highly contagious; Variola major ~30% mortality.
- Clinical: Synchronous, centrifugal rash (macules → papules → vesicles → pustules → scabs); no significant lymphadenopathy.
- Guarnieri bodies: Intracytoplasmic eosinophilic inclusions.

- Bioterrorism concern.
- Vaccinia Virus (Orthopoxvirus)
- Smallpox vaccine virus.
- Localized 'take' at site.
- Complications: Eczema vaccinatum (atopic dermatitis), progressive vaccinia (immunocompromised), generalized vaccinia, postvaccinial encephalitis.
⭐ Smallpox, caused by Variola virus, was declared eradicated in 1980, a monumental achievement of global vaccination efforts using the Vaccinia virus.
High‑Yield Points - ⚡ Biggest Takeaways
- Molluscum Contagiosum (MCV): Features umbilicated pearly papules, Henderson-Paterson bodies. Extensive in HIV/immunodeficiency.
- Orf: Parapoxvirus from sheep/goats. Presents targetoid lesions on hands; self-limiting. Occupational hazard.
- Milker's Nodule: Parapoxvirus from cattle. Similar to Orf, forms nodules on hands; self-limiting.
- Poxviruses: Are the largest DNA viruses, with unique cytoplasmic replication.
- Cowpox: Orthopoxvirus. Rodent reservoir, cat vector. Historically significant for smallpox vaccine.
- Smallpox (Variola): Eradicated Orthopoxvirus. Known for synchronous centrifugal rash, Guarnieri bodies.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

