HIV-Related Dermatoses - Immune Meltdown Manifestations
- Core: Progressive ↓ CD4+ T-cell count → immune dysregulation & opportunistic conditions.
- Manifestations reflect CD4 strata:
- Early (>500/µL): Seborrheic dermatitis, xerosis.
- Intermediate (200-500/µL): Oral hairy leukoplakia (OHL), candidiasis, herpes zoster.
- Late (<200/µL): Kaposi sarcoma (KS), eosinophilic folliculitis, extensive molluscum.
- Key Groups:
- Infections (viral, fungal, bacterial)
- Inflammatory dermatoses
- Neoplasms (KS, lymphoma)
- Adverse drug reactions

⭐ Kaposi sarcoma (KS), linked to HHV-8, is an AIDS-defining illness, typically appearing when CD4 count < 200 cells/µL.
HIV-Related Dermatoses - Viral & Fungal Frenzy
- Viral Infections:
- Herpes Zoster (VZV): Often severe, multidermatomal, chronic, or disseminated. ↑ risk if CD4 < 200 cells/µL. May present as atypical, persistent lesions.
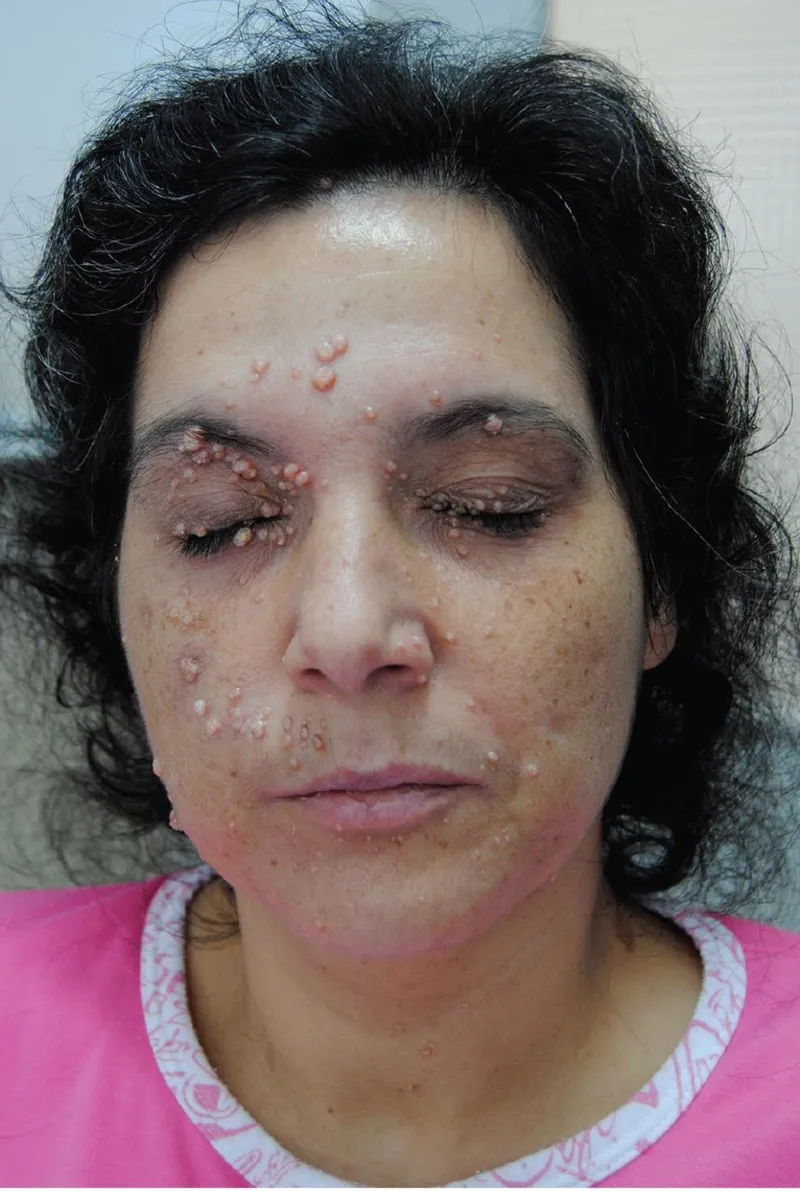
- Molluscum Contagiosum (MCV): Numerous, giant (>5mm), persistent lesions, often facial or anogenital. Common if CD4 < 100 cells/µL.
- Oral Hairy Leukoplakia (OHL): EBV-induced. White, corrugated, non-removable plaques on lateral tongue. Not premalignant.
⭐ OHL is highly specific for HIV infection and often an early sign of immunosuppression (CD4 < 400 cells/µL).
- Fungal Infections:
- Candidiasis:
- Oral thrush: White, removable plaques. Angular cheilitis.
- Esophageal: AIDS-defining. Dysphagia, odynophagia.
- Vulvovaginal: Persistent, recurrent, severe.
- Cryptococcosis (Cutaneous): Umbilicated papules/nodules (MCV-like), plaques, ulcers. Sign of dissemination. Usually CD4 < 100 cells/µL.
- Histoplasmosis (Disseminated): Varied skin lesions (papules, pustules, ulcers, molluscum-like). Usually CD4 < 150 cells/µL. 📌 Remember "Histo Hides" in macrophages!
- Candidiasis:
HIV-Related Dermatoses - Bacterial & Inflammatory Blitz
- Bacterial Infections:
- Bacillary Angiomatosis (BA): Bartonella henselae/quintana (CD4 < 200/µL). Friable vascular papules/nodules. Rx: Erythromycin or Doxycycline.

- Staphylococcal Infections: Most frequent. Folliculitis, furuncles, impetigo. ↑MRSA risk.
- Syphilis: Atypical, accelerated course (malignant syphilis). ↑Neurosyphilis.
- Bacillary Angiomatosis (BA): Bartonella henselae/quintana (CD4 < 200/µL). Friable vascular papules/nodules. Rx: Erythromycin or Doxycycline.
- Inflammatory Dermatoses:
- Seborrheic Dermatitis: Very common, often severe, widespread.
⭐ Severe or explosive-onset seborrheic dermatitis can be an early cutaneous marker of HIV infection.
- Psoriasis: New onset or exacerbation; often severe (erythrodermic, pustular).
- Eosinophilic Folliculitis: Intensely pruritic papules/pustules (face, trunk). CD4 < 250-300/µL. Peripheral eosinophilia.
- Pruritic Papular Eruption (PPE): Chronic itchy papules (extremities, trunk). CD4 < 200-300/µL.
- Drug Reactions: High incidence (TMP-SMX, NNRTIs). Morbilliform common_
- Seborrheic Dermatitis: Very common, often severe, widespread.
HIV-Related Dermatoses - Alarming Skin Changes
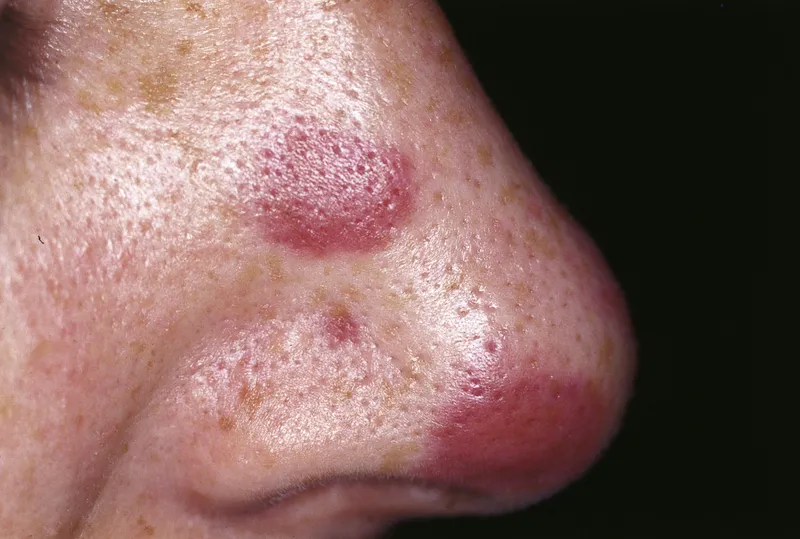
- Kaposi Sarcoma (KS)
- HHV-8 associated vascular neoplasm.
- Macules, papules, plaques, nodules; violaceous/brown.
- Oral, GI, pulmonary involvement common.
- Diagnosis: Biopsy (spindle cells, neovascularization, extravasated RBCs).
- Non-Hodgkin Lymphoma (NHL)
- ↑ risk, often extranodal (CNS, GI, skin).
- Skin: nodules, plaques, ulcers; B-cell > T-cell.
- Squamous Cell Carcinoma (SCC)
- ↑ risk, esp. anogenital (HPV-related) & sun-exposed areas.
- Aggressive course.
- Severe Cutaneous Adverse Reactions (SCARs)
- ↑ incidence with certain drugs (e.g., sulfonamides, nevirapine).
- Stevens-Johnson Syndrome (SJS) / Toxic Epidermal Necrolysis (TEN).
- Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS).
⭐ Exam Favourite: Kaposi Sarcoma is the most common malignancy in HIV-infected individuals, often presenting with characteristic violaceous skin lesions, and its incidence has significantly decreased with effective antiretroviral therapy (ART).
High‑Yield Points - ⚡ Biggest Takeaways
- Kaposi sarcoma (HHV-8): AIDS-defining violaceous lesions.
- Oral hairy leukoplakia (EBV): White, non-scrapable plaques on lateral tongue; indicates immunosuppression.
- Severe seborrheic dermatitis: Common, often atypical presentation.
- Eosinophilic folliculitis: Intensely pruritic papules, especially on trunk/face.
- Herpes zoster: Often severe, recurrent, or multidermatomal.
- Molluscum contagiosum: Can be widespread, giant, or facial.
- Bacillary angiomatosis: Bartonella infection; mimics Kaposi sarcoma, biopsy needed for differentiation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

