Tropical Ulcers - Jungle Sores Saga
- Definition: Acute, painful, rapidly destructive, necrotizing skin lesions, often on lower extremities. Endemic in hot, humid tropical/subtropical areas (e.g., Africa, SE Asia, Central/South America).
- Etiology: Polymicrobial; key anaerobes Fusobacterium ulcerans, Treponema vincentii, Bacteroides spp. Often a synergistic infection.
- Predisposing Factors: Minor trauma, insect bites, malnutrition, poor hygiene, rural settings, immunodeficiency.
⭐ Diagnosis is primarily clinical, but Gram stain/dark-field microscopy can identify spirochetes and fusiform bacilli (Vincent's organisms).
Tropical Ulcers - Lesion Lineup
- Site: Predominantly lower limbs (legs, ankles, feet).
- Progression:
- Starts as a papule.
- Evolves to vesicle/bulla.
- Breaks down into a painful ulcer.
- Ulcer characteristics: necrotic base, raised, edematous, violaceous, undermined edges.
- Systemic Symptoms: Fever, malaise (less common unless severe or extensive).
- Discharge: Characteristic foul-smelling seropurulent discharge.
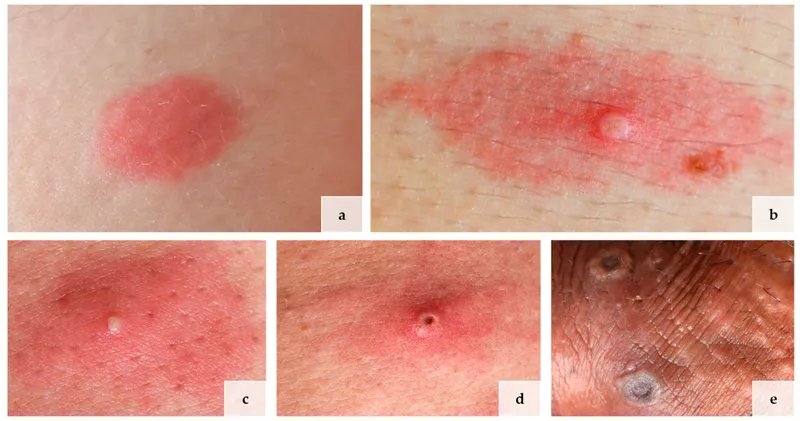
⭐ Exam Favourite: Tropical ulcers are often polymicrobial, commonly involving Fusobacterium ulcerans and spirochetes like Treponema vincentii (Vincent's organisms).
Tropical Ulcers - Ulcer Unmasking
- Investigations:
- Gram stain, Culture: Identify polymicrobial nature (fusiform bacilli, spirochetes); anaerobes often difficult to culture.
- Biopsy (advancing edge): Histopathology reveals acute & chronic inflammation, coagulative necrosis, numerous mixed organisms.
- Dark-field microscopy: Essential for detecting motile spirochetes.
- Differential Diagnosis:
Condition Key Feature Buruli Ulcer Painless, undermined edges Yaws Mother yaw, raspberry lesions Leishmaniasis Raised border, satellite lesions Pyoderma Gangrenosum Violaceous border, pathergy SCC Rolled, indurated edge
⭐ Biopsy from the ulcer's advancing edge is crucial for identifying causative organisms in tropical ulcers.
Tropical Ulcers - Healing Hurdle
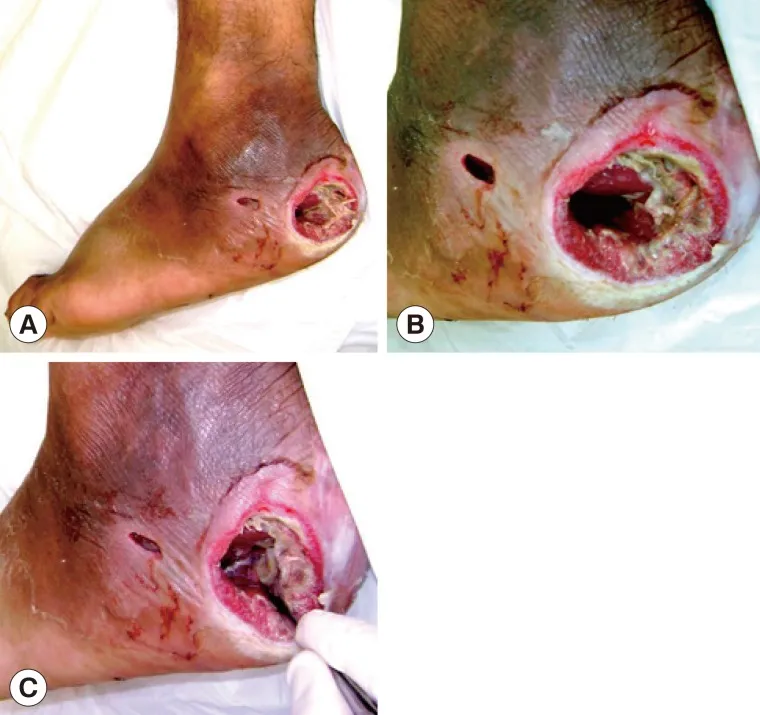
- Core Management Principles:
- Wound hygiene: Daily cleaning, removal of slough & necrotic tissue (debridement).
- Dressings: Non-adherent, moist wound healing.
- Limb rest & elevation to ↓ edema.
- Nutritional support: High protein, vitamins (A, C, Zinc).
- Antimicrobial Therapy:
- Systemic (Key):
- Penicillin (e.g., Procaine Penicillin 600,000 IU IM daily or Benzathine Penicillin 2.4 million units IM once).
- Metronidazole (400-500 mg PO TID for 7-10 days) for anaerobes.
- Topical antibiotics if superficial infection.
- Systemic (Key):
- Surgical Options:
- Extensive debridement for deep/necrotic ulcers.
- Skin grafting for large, persistent defects.
- Prevention Strategies:
- Protective footwear.
- Good personal & foot hygiene.
- Prompt care for skin trauma.
⭐ Vincent's organisms (fusiform bacilli and spirochetes) are classically implicated in the etiology of tropical ulcers.
Tropical Ulcers - Scar Stories
- Complications:
- Chronic ulceration, disfiguring scars, contractures
- Lymphedema
- Secondary bacterial infection, osteomyelitis
- ⚠️ Marjolin's ulcer (SCC in chronic scar/ulcer)
- Prognosis:
- Good if treated early.
- Chronic cases: debilitating, ↑ risk of complications.
⭐ Marjolin's ulcer, a squamous cell carcinoma, can arise in chronic tropical ulcers or burn scars, often after many years (typically 10-25 years latency).
High‑Yield Points - ⚡ Biggest Takeaways
- Tropical ulcers: Polymicrobial infections, often with Fusobacterium ulcerans and spirochetes.
- Risk factors: Minor trauma, poor hygiene, malnutrition in tropical areas.
- Clinical features: Painful, rapidly progressing ulcer; undermined edges, foul discharge; typically on lower limbs.
- Diagnosis: Primarily clinical; microscopy shows mixed organisms.
- Treatment: Systemic antibiotics (e.g., metronidazole + penicillin), wound debridement, improved nutrition.
- Complications: Chronic ulceration, scarring, rare squamous cell carcinoma (Marjolin's ulcer).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

