Tropical Mycoses: Overview - Fungal Heat Wave
Tropical Mycoses: Fungal infections prevalent in hot, humid climates, often with distinct clinical presentations.
- Predisposing Factors: High temperature & humidity, skin trauma (e.g., thorns, splinters), barefoot walking, poor hygiene, malnutrition.
- Classification:
- Superficial: E.g., Tinea versicolor, Piedra.
- Cutaneous: E.g., Dermatophytosis (tropical patterns like Tinea imbricata).
- Subcutaneous: E.g., Mycetoma, Sporotrichosis, Chromoblastomycosis.
- Systemic (with skin signs): E.g., Histoplasmosis, Paracoccidioidomycosis.
⭐ Mycetoma ("Madura foot") classically presents with a triad: painless subcutaneous mass, multiple sinuses, and discharge containing granules (grains).
Subcutaneous Mycoses: Mycetoma & Sporotrichosis - Deep Tissue Terrors
Mycetoma
- Chronic granulomatous infection of skin, subcutaneous tissue, fascia, bone.
- Etiology: Eumycetoma (fungal) vs. Actinomycetoma (bacterial).
- Clinical Triad: Painless firm subcutaneous swelling, multiple discharging sinuses, visible grains (colonies).
- Diagnosis: Grains (color, size, consistency), imaging (X-ray, MRI for bone involvement), culture.
- Management: Medical (antifungals/antibiotics), surgical debridement/amputation for extensive disease.
| Feature | Eumycetoma | Actinomycetoma |
|---|---|---|
| Cause | Fungi (e.g., Madurella mycetomatis) | Bacteria (e.g., Nocardia, Actinomadura) |
| Grains | Large, black/white/yellow | Small, white/yellow/red |
| Bone | Less common, lytic lesions | More common, osteosclerotic |
| Response | Poor to antifungals | Good to antibiotics (e.g., Welsh regimen) |
Sporotrichosis
- Etiology: Sporothrix schenckii (dimorphic fungus), often from trauma with contaminated plants (rose thorns 📌 "Rose gardener's disease").
- Clinical Forms:
- Lymphocutaneous: Most common; nodule at inoculation site → chain of painless nodules along lymphatics.
- Fixed cutaneous: Solitary plaque/ulcer, non-lymphatic spread.
- Disseminated: Rare, in immunocompromised.
- Diagnosis: Culture (gold standard), biopsy (cigar-shaped yeasts, Asteroid bodies - Splendore-Hoeppli phenomenon).
- Management: Itraconazole (DOC for cutaneous/lymphocutaneous), Saturated Solution of Potassium Iodide (SSKI) (alternative).
⭐ Asteroid bodies (Splendore-Hoeppli phenomenon) in sporotrichosis are antigen-antibody complexes surrounding the yeast, not specific to sporotrichosis but highly suggestive in the right clinical context.
Subcutaneous Mycoses: Chromoblastomycosis & Co. - Crusted Calamities
-
Chromoblastomycosis:
- Etiology: Dematiaceous (pigmented) fungi like Fonsecaea pedrosoi, Cladophialophora carrionii.
- Clinical: Chronic verrucous, crusted, "cauliflower-like" plaques, often on feet/legs.
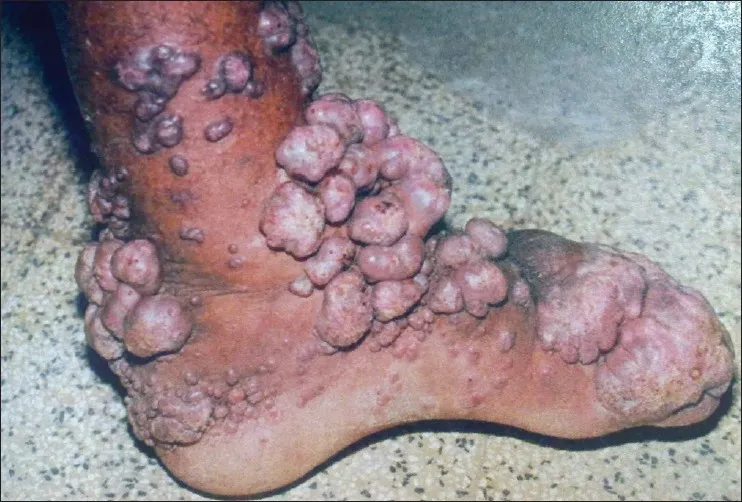
- Diagnosis: Key is finding sclerotic bodies (Medlar bodies, "copper pennies") on microscopy/biopsy.
⭐ Sclerotic bodies (Medlar bodies, copper pennies) are pathognomonic for Chromoblastomycosis.
- Management: Itraconazole (200-400 mg/day), terbinafine. Adjuncts: heat therapy, cryosurgery, surgical excision.
-
Other Subcutaneous Mycoses (Briefly):
- Lobomycosis: Keloidal nodules; Lacazia loboi (yeast chains).
- Subcutaneous Phaeohyphomycosis: Cysts/abscesses; pigmented hyphae in tissue (no grains/sclerotic bodies).
Systemic Mycoses: Dimorphic Threats - Shape‑Shifting Spores
- Histoplasmosis (H. capsulatum):
- var. capsulatum (American): AIDS-associated; disseminated disease presents with skin papules, nodules, ulcers.
- var. duboisii (African): Primarily granulomatous skin & bone lesions; often larger.
- Dx: Biopsy (intracellular yeasts in macrophages), culture, antigen detection.
- Mgmt: Itraconazole (mild-mod); Amphotericin B (severe).
- Paracoccidioidomycosis (P. brasiliensis):
- Geography: Latin America.
- Clinical: Pulmonary involvement; mucocutaneous lesions (painful 'mulberry-like' oral/nasal ulcers).
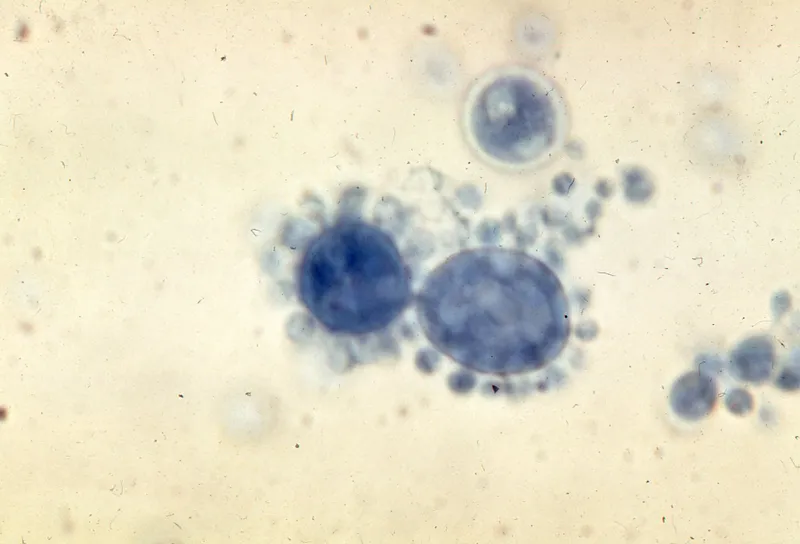
- Dx: Microscopy (yeast with multiple buds: 'mariner’s wheel'). 📌 Pilot's Wheel.
- Mgmt: Itraconazole (DOC, 6-12 months); Amphotericin B (severe).
⭐ In Paracoccidioidomycosis, the characteristic 'mariner's wheel' appearance of P. brasiliensis yeast with multiple budding is a key diagnostic feature.
 oka
oka
High‑Yield Points - ⚡ Biggest Takeaways
- Mycetoma (Madura foot) presents with painless subcutaneous nodules, sinuses, and discharge of grains.
- Chromoblastomycosis shows verrucous plaques and characteristic sclerotic bodies (Medlar bodies, copper pennies) on microscopy.
- Sporotrichosis ("rose gardener's disease") typically has lymphocutaneous spread; microscopy reveals cigar-shaped yeasts.
- Lobomycosis features chronic keloidal lesions with chains of yeast cells (Lacazia loboi).
- Rhinosporidiosis causes friable, polypoidal nasal or ocular lesions with large sporangia containing endospores.
- Phaeohyphomycosis is an infection caused by dematiaceous (pigmented) fungi, presenting with diverse clinical forms depending on the site and host immunity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

