Etiology & Transmission - Worm's Wanderings
- Causative Agent: Onchocerca volvulus (filarial nematode).
- Vector: Female Simulium blackflies.
- Transmit infective L3 larvae during a blood meal.
- Transmission Cycle:
- Blackfly ingests microfilariae from an infected human.
- Larvae develop to L3 stage in the fly (1-3 weeks).
- Infective L3 larvae are deposited on human skin during a subsequent bite, entering via the bite wound.
- Worm's Wanderings:
- Adult worms reside in subcutaneous nodules (onchocercomata).
- They release millions of microfilariae (mf) that migrate throughout the skin and eyes, causing pathology.
⭐ Vector (Simulium blackfly) breeds in fast-flowing, oxygen-rich rivers, linking the disease to riverine areas.
Skin Manifestations - Itch, Lumps, Leopard Spots

- Pruritus (Itch): Intense, often earliest symptom; leads to excoriations.
- May have "crawling sensation".
- Onchocercomata (Nodules): Firm, non-tender subcutaneous lumps with adult worms.
- Typically over bony prominences (e.g., iliac crests, ribs).
- Depigmentation ("Leopard Skin"): Characteristic spotted loss of pigment, common on shins.
- Chronic Changes:
- "Lizard skin": Thin, dry, atrophic, wrinkled skin.
- "Hanging groin": Loss of skin elasticity.
- Sowda: Localized, hyperpigmented, lichenified, intensely itchy dermatitis. (Hyper-reactive form)
⭐ "Sowda" is a chronic, hyperpigmented, lichenified onchodermatitis, representing a hyper-reactive immune response, typically seen in Yemen and Sudan.
Ocular & Systemic Impact - The Blinding Path
- Ocular Manifestations ("River Blindness"):
- Microfilariae (mf) invade all eye structures.
- Anterior Segment:
- Live/dead mf in anterior chamber (AC).
- "Snowflake" (punctate) keratitis → progresses to sclerosing keratitis (corneal opacity).
- Iridocyclitis, secondary glaucoma, complicated cataracts.
- Posterior Segment:
- Chorioretinitis (retinal pigment epithelium [RPE] changes, "leopard skin" fundus).
- Optic neuritis & subsequent optic atrophy.
- Outcome: Progressive, often irreversible blindness.
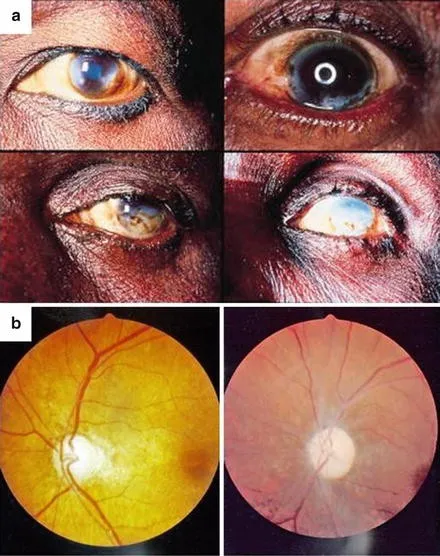
- Systemic Involvement:
- Severe Dermatological: Chronic onchodermatitis; Sowda (hyper-reactive onchodermatitis in hypoendemic areas).
- Lymphatic System: Lymphadenopathy (e.g., "hanging groin"), chronic lymphedema.
- General Debilitation: Musculoskeletal pain, weight loss/cachexia.
- Neurological Links: Potential association with Nodding syndrome & other forms of epilepsy.
⭐ Onchocerciasis is the second leading infectious cause of blindness worldwide.
Diagnosis & Management - Spot & Stop the Worm
- Diagnosis:
- Clinical: Chronic pruritus, "Sowda" (papular dermatitis), "leopard skin" (atrophy), onchocercomata (nodules), ocular signs ("river blindness").
- Gold Standard: Skin snips (2-3mg, bloodless) for microfilariae.
- Supportive: PCR on skin (↑sensitivity); slit-lamp for eye microfilariae; nodule exam (adult worms).
- Management:
- Ivermectin: (📌 Dose: 150 mcg/kg) PO, single dose, repeat q 6-12 months. Potent microfilaricidal.
- Doxycycline: 100-200 mg/day PO x 4-6 wks. Targets Wolbachia, sterilizes adults, slow macrofilaricidal, ↓Mazzotti.
- Nodulectomy: Reduces worm burden, esp. head/neck.
⭐ Mazzotti reaction (post-DEC: fever, rash, pruritus) is diagnostic but severe. Ivermectin causes milder reactions. DEC is contraindicated.
High‑Yield Points - ⚡ Biggest Takeaways
- Caused by Onchocerca volvulus, transmitted by Simulium blackfly bites near fast-flowing rivers.
- Leads to river blindness from ocular microfilarial invasion and chronic inflammation.
- Skin signs: intense itching, papular dermatitis, lichenification (Sowda), leopard skin, onchocercomata (nodules).
- Diagnosis: skin snip microscopy for microfilariae is gold standard.
- Treatment: Ivermectin (microfilaricidal); Doxycycline targets Wolbachia symbionts, reducing adult worm fertility.
- Mazzotti reaction: post-treatment hypersensitivity (fever, rash), historically with DEC, less with Ivermectin_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

