Myiasis Overview - Maggot Mayhem
- Definition: Tissue infestation by dipterous larvae (maggots) of flies.
- Causative Flies (Order: Diptera):
- Families: Calliphoridae (e.g., Chrysomya), Sarcophagidae (e.g., Sarcophaga), Oestridae (e.g., Hypoderma, Dermatobia).
- Key Indian Example: Chrysomya bezziana (Old World screwworm).
- Mode of Infestation:
- Accidental: Larvae ingested/enter orifices (e.g., intestinal from Musca domestica).
- Facultative: Larvae develop in decaying tissue or existing wounds.
- Obligatory: Larvae require living tissue for development (most pathogenic).
⭐ Chrysomya bezziana is a significant cause of obligatory wound myiasis in India, where larvae invade living tissue.
Myiasis Classification - Invasion Sites
| Type | Common Sites | Key Larvae Examples | Clinical Hint |
|---|---|---|---|
| Cutaneous | Skin | ||
| - Furuncular | Exposed areas | Dermatobia hominis, Cordylobia anthropophaga | Boil-like lesion, central punctum, movement |
| - Creeping/Migratory | Epidermis/Dermis | Gasterophilus spp., Hypoderma spp. | Serpiginous, erythematous tracts |
| - Wound/Traumatic | Neglected wounds, ulcers | Cochliomyia hominivorax, Wohlfahrtia spp., Chrysomya bezziana | Larvae in wound, tissue destruction |
| Cavity | Nasopharynx, Orbit, Ear, Urogenital, Intestinal | Oestrus ovis, Fannia spp., Musca domestica | Site-specific (e.g., epistaxis, otorrhea, dysuria) |
| Systemic (Rare) | Internal organs | Hypoderma spp. (visceral migration) | Vague, severe systemic illness; often incidental |
⭐ Wound myiasis, often caused by screwworm flies like Cochliomyia hominivorax, critically signals neglected wounds and can cause rapid tissue destruction.
Myiasis Clinicals - Spotting Squatters
-
Furuncular (e.g., Dermatobia hominis):
- Painful, itchy, erythematous nodule.
- Central pore (punctum) with serosanguinous discharge.
- Sensation of movement; larva sometimes visible.
-
Creeping / Migratory (e.g., Gasterophilus, Hypoderma):
- Serpiginous, erythematous, intensely pruritic linear tracts.
- Larva migrates within epidermis.
-
Wound / Traumatic (e.g., Cochliomyia hominivorax):
- Larvae infest pre-existing wounds or necrotic tissue.
- Foul smell, pain, significant tissue destruction.
-
Cavitary (e.g., Oestrus ovis - nasal):
- Site-specific symptoms:
- Nasal: Obstruction, epistaxis, pain, foreign body sensation.
- Auricular: Otalgia, discharge, sensation of crawling, tinnitus.
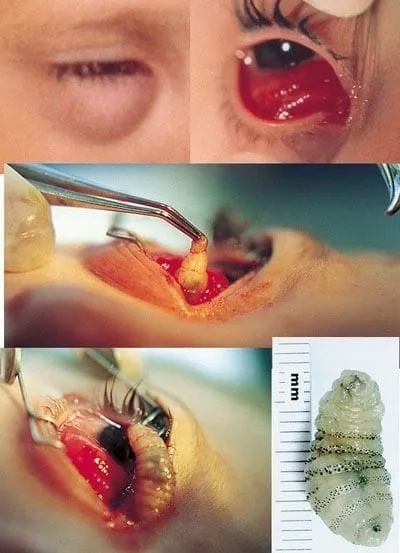
- Ophthalmomyiasis: Interna (visual disturbance, pain) or Externa (foreign body sensation, redness, chemosis).
- Site-specific symptoms:
⭐ The characteristic central punctum in furuncular myiasis often intermittently extrudes serosanguinous fluid or the posterior end of the larva (the "breathing spiracles").
Myiasis Dx & Rx - Eviction Notice
- Dx: Clinical (travel Hx, visualize larvae); larval ID (entomologist).
- Rx: 📌 'Suffocate, Sedate, Snatch'
- Occlusion (petroleum jelly) → Manual/Surgical extraction.
- Wound care; antibiotics for secondary infection.
- Oral Ivermectin (200 mcg/kg) for extensive/cavitary/difficult cases.
- Prevention: Fly control, wound hygiene, protective clothing.
⭐ Occlusive therapy works by depriving the larva of oxygen, forcing it to migrate towards the surface for easier removal.
High‑Yield Points - ⚡ Biggest Takeaways
- Myiasis: Infestation of live human/animal tissue by dipterous larvae (maggots).
- Furuncular myiasis (e.g., Dermatobia hominis, Tumbu fly): Boil-like lesion with a central punctum for larval respiration.
- Wound myiasis (e.g., Screwworms like Cochliomyia): Larvae infest open wounds/cavities, causing aggressive tissue destruction.
- Creeping myiasis (e.g., Gasterophilus): Characterized by migratory serpiginous erythematous tracts.
- Diagnosis: Clinical by visualizing larvae (movement, bubbles at punctum); dermoscopy aids.
- Treatment: Occlusion (petroleum jelly), surgical extraction, or oral ivermectin for extensive cases.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

