Etiopathogenesis & Classification - Foe & Its Forms
-
Etiopathogenesis:
- Agent: Mycobacterium leprae (acid-fast bacillus).
- Optimal Temp: 30-33°C (favours cooler body parts: skin, peripheral nerves).
- Transmission: Primarily respiratory droplets from untreated MB cases; prolonged close contact.
- Incubation Period: Long, average 2-5 years (can range from months to 20 years).
⭐ M. leprae is an obligate intracellular parasite and cannot be cultured on standard artificial media.
-
Classification Systems:
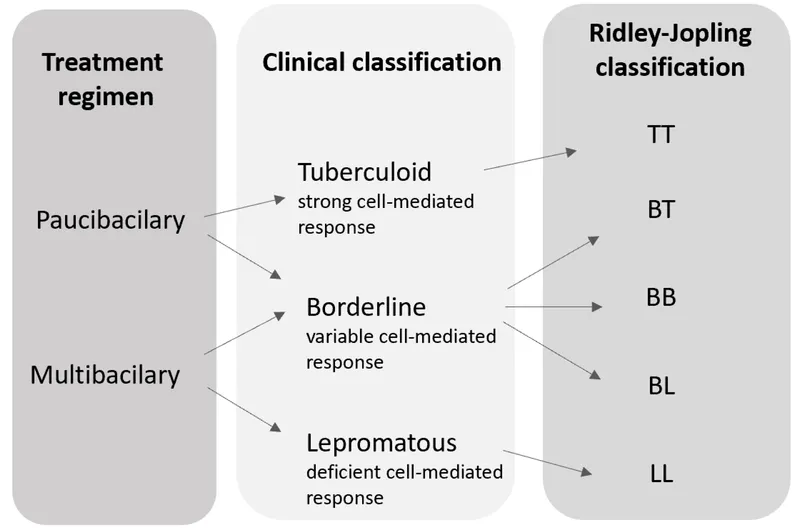
- Ridley-Jopling (R-J) Spectrum: Based on cellular immunity.
- Tuberculoid (TT), Borderline Tuberculoid (BT), Mid-Borderline (BB), Borderline Lepromatous (BL), Lepromatous (LL).
- 📌 Mnemonic: Tuberculoid Tough, Lepromatous Lousy, Borderlines Bad.
- WHO Classification (for treatment): Based on number of skin lesions & Bacteriological Index (BI).
- Paucibacillary (PB): ≤5 skin lesions AND skin smear negative (or BI < 2+).
- Multibacillary (MB): >5 skin lesions OR nerve involvement (neuritis) OR skin smear positive (BI ≥ 2+).
- Ridley-Jopling (R-J) Spectrum: Based on cellular immunity.
Clinical Manifestations - The Disease Unmasked
-
Skin & Nerve (Ridley-Jopling Spectrum):
Type Skin Lesions Sensory Loss Nerve Involvement TT 1-few, defined, anaesthetic macules/plaques Early, marked Early, severe BT Few-mod, asymmetric, varied plaques Moderate Prominent BB Num, polymorphic, annular/punched Moderate Common, severe BL Many, ill-defined, shiny lesions Patchy, less severe Moderate, many LL Diffuse infiltration, nodules, madarosis Late, glove-stocking Widespread, late -
Nerve Damage:
- Affected Nerves: Ulnar, Median, Radial, Common Peroneal, Posterior Tibial, Facial, Great Auricular.
- Signs: Thickened nerves, tenderness; motor loss (e.g., claw hand, foot drop); sensory loss; trophic ulcers; deformities (e.g., lagophthalmos).
-
Other: Eye (corneal ulcers, blindness), Testicular atrophy (LL).
⭐ Leonine facies is a characteristic feature of lepromatous leprosy.
Diagnosis & Management - Spotting & Stopping
- Cardinal Signs:
- Skin patches (hypopigmented/erythematous) + definite sensory loss.
- Thickened peripheral nerve(s).
- AFB in SSS/biopsy.
- Slit-Skin Smear (SSS):
- Sites: Earlobes, lesions.
- Bacteriological Index (BI): Bacillary load (0-6+).
- Morphological Index (MI): Viable bacilli %.
- Skin Biopsy: Histopathology for classification (TT/BT: granulomas; LL/BL: Virchow cells, globi).

- Lepromin Test: Assesses CMI; not diagnostic. Mitsuda (+ve in TT/BT): >5mm induration at 4 wks.
- Management (WHO MDT):
Type Regimen Duration PB RIF (600mg monthly) + DAP (100mg daily) 6 months MB RIF (600mg monthly) + CLO (300mg monthly, 50mg daily) + DAP (100mg daily) (📌 RDC) 12 months
⭐ SLPB: Single dose Rifampicin (600mg) + Ofloxacin (400mg) + Minocycline (100mg) (ROM).
Lepra Reactions & Prevention - Fiery Flare-ups & Control
| Feature | Type 1 (Reversal Reaction, RR) | Type 2 (Erythema Nodosum Leprosum, ENL) |
|---|---|---|
| Mechanism | ↑ CMI (Type IV). | Immune complex (Type III). |
| Clinical | Inflamed lesions, neuritis. | Tender nodules, fever, systemic. |
| Onset | During/after MDT. | LL/BL; during/after MDT. |
| Management | Prednisolone 40-60mg; NSAIDs. | Clofazimine, Thalidomide 100-400mg; Steroids. |
- NLEP Key Strategies:
- Early case detection & prompt MDT.
- High MDT coverage.
- Disability Prevention & Medical Rehabilitation (DPMR).
- IEC activities.
- ASHA's role: awareness, case finding, referral.
⭐ Thalidomide: DOC for severe or recurrent ENL. ⚠️ Teratogenic; contraindicated in pregnancy.
High‑Yield Points - ⚡ Biggest Takeaways
- Caused by M. leprae (acid-fast); affects skin & peripheral nerves.
- Key signs: anesthetic skin lesions, thickened nerves, positive slit-skin smear (SSS).
- Spectrum: Tuberculoid (TT) (PB, strong CMI) to Lepromatous (LL) (MB, weak CMI).
- Lepra reactions: Type 1 (Reversal) & Type 2 (ENL) are acute immune events.
- Multidrug Therapy (MDT) is crucial for both Paucibacillary (PB) & Multibacillary (MB).
- Nerve damage leads to characteristic deformities and disability.
- SSS for Bacteriological Index (BI) aids diagnosis and monitors treatment_response_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

