Melanocytic Nevi - Spotting the Dots
- Benign proliferations of melanocytes (nevus cells), neural crest origin. "Moles."
- Classified by nevus cell location within skin layers:
- Junctional Nevi: At dermo-epidermal junction. Macular, uniformly pigmented.
- Compound Nevi: In epidermis & dermis. Papular, pigmented.
- Intradermal Nevi: Entirely within dermis. Papular/dome-shaped, often flesh-colored or lightly pigmented, may have hairs.

⭐ Congenital melanocytic nevi (CMN): Present at birth/within first few weeks. Risk of melanoma development is proportional to size, especially giant CMN (>20 cm).
Melanocytic Nevi - The Mole Lineup
Melanocytic nevi, or moles, are common benign proliferations of melanocytes (nevus cells). They are classified based on the histological location of nevus cells within the skin layers and distinct clinical presentations.

| Type | Nevus Cell Location | Key Clinical Features | Malignant Potential / Notes |
|---|---|---|---|
| Junctional | Dermoepidermal (DE) jct. | Flat/macular, uniform brown-black | Low; common in children/young adults |
| Compound | DE jct. & Dermis | Raised, pigmented papule, smooth/warty | Low |
| Intradermal | Dermis | Dome-shaped, skin-colored/light brown, +/- hair | Very Low; common in adults |
| Congenital | Dermis (often deep) | At birth. Small <1.5cm, Med 1.5-19.9cm, Giant >20cm | ↑ with size (esp. Giant) |
| Dysplastic | Usually Compound/Junctional | >5mm, irregular border/pigment ("ugly duckling") | ↑ melanoma risk marker; may be multiple |
| Spitz | Epidermis/Dermis | Children; pink/red papule; rapid growth | Benign; "benign juvenile melanoma" (misnomer) |
| Blue | Dermis (dendritic) | Blue/grey/black firm papule/nodule | Low (cellular blue nevus higher risk) |
| Halo | Any (lymphocytic infiltrate) | Central nevus, peripheral depigmented halo | Usually benign; immune response |
Melanocytic Nevi - Moles Gone Wild
- Benign proliferations of melanocytes (nevus cells); types: junctional, compound, intradermal.
- Monitor for changes. 📌 ABCDE criteria for melanoma suspicion:
- Asymmetry
- Border irregularity
- Color variegation
- Diameter >6mm
- Evolving (change in size, shape, color, symptoms)
- Other signs: "Ugly duckling" sign (mole looks different from patient's other moles).
- Dermoscopy: Aids diagnosis. Look for atypical pigment networks, irregular globules, regression structures, blue-white veil.
- Risk of melanoma: Low overall. Higher in dysplastic nevi, numerous nevi (>50-100), or large/giant congenital nevi.
⭐ Giant congenital melanocytic nevi (CMN), especially those >20cm ("bathing trunk nevi"), carry a 4-10% lifetime risk of developing melanoma, often within the first decade.
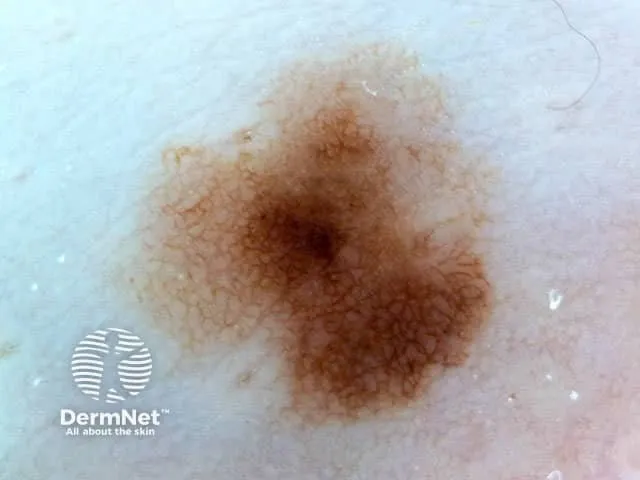
Melanocytic Nevi - Act or Observe?
- Evaluation: Asymmetry, Border, Color, Diameter >6mm, Evolving (ABCDE); "ugly duckling" sign; new/changing lesion; symptoms (itch, pain, bleeding); dermoscopy.
- Management:
- Low suspicion: Observe, educate on self-exams. Serial photography for high-risk.
- High suspicion/changes: Biopsy for histopathology.
- Biopsy Choice:
- Excisional: Preferred for suspicious nevi; 1-3mm clinical margins.
- Incisional (punch/shave): Large lesions or diagnostic query. ⚠️ Risk of sampling error/misstaging.
- Post-Biopsy Action (Histology-Guided):
- Benign: Routine skin surveillance.
- Dysplastic: Close observation or re-excision (margins 2-5mm for moderate/severe atypia).
- Melanoma: Full staging & melanoma management.
⭐ The "ugly duckling" sign-a nevus differing from a patient's other nevi-is a strong indicator for biopsy.
High-Yield Points - ⚡ Biggest Takeaways
- Melanocytic nevi are benign proliferations of melanocytes (nevus cells).
- Junctional nevi: flat, located at the dermo-epidermal junction.
- Compound nevi: raised, with melanocytes in epidermis and dermis.
- Intradermal nevi: dome-shaped, melanocytes confined to the dermis.
- Use ABCDE criteria for melanoma suspicion in any pigmented lesion.
- Large congenital nevi (e.g., giant hairy nevus) have a significant melanoma risk.
- Dysplastic nevi (atypical moles) are melanoma precursors and risk markers.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

