Overview & Classification - Pustule Parade
- Characterized by widespread or localized sterile pustules on erythematous base; distinct from plaque psoriasis.
- Can be life-threatening (e.g., GPP).
Classification:
- Generalized Pustular Psoriasis (GPP)
- Von Zumbusch variant (acute, febrile)
- Impetigo herpetiformis (psoriasis of pregnancy)
- Annular/circinate variant
- Infantile/juvenile GPP
- Localized Pustular Psoriasis
- Palmoplantar Pustulosis (PPP)
- Acrodermatitis Continua of Hallopeau (ACH)
⭐ Generalized Pustular Psoriasis (GPP) can be triggered by rapid withdrawal of systemic corticosteroids or potent topical steroids, infections, or certain medications (e.g., lithium, antimalarials).
Generalized Pustular Psoriasis (GPP) - Fiery Outbreak
- Acute, severe, potentially life-threatening; widespread sterile pustules coalescing into "lakes of pus" on erythematous skin.
- Systemic: high fever, chills, arthralgia, ↑leukocytosis.
- Triggers:
- Corticosteroid withdrawal (most common).
- Infections, hypocalcemia, pregnancy (impetigo herpetiformis), drugs (lithium, antimalarials).
- Skin: fiery red, tender, burning. Nail changes common.
- Management: Hospitalization. First-line: Acitretin. Alternatives: Cyclosporine, Methotrexate, Biologics (e.g., infliximab). Avoid systemic steroids (rebound risk).
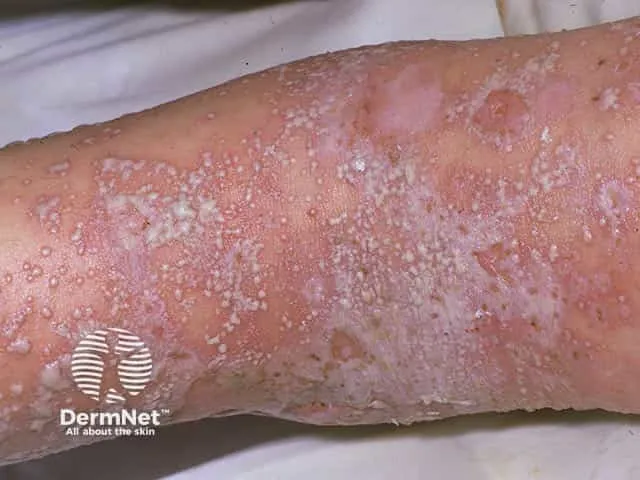
⭐ Impetigo herpetiformis is GPP of pregnancy, often linked to hypocalcemia and typically occurs in the third trimester.
Localized Pustular Psoriasis - Sticky Spots
- Chronic, relapsing sterile pustules on specific sites.
- Palmoplantar Pustulosis (PPP):
- Palms & soles; often symmetrical.
- Yellow pustules, erythema, scaling, fissures.
- Strongly associated with smoking (up to 95%).
- Nail involvement common.
- Acrodermatitis Continua of Hallopeau (ACH):
- Rare; affects distal digits (fingers/toes), periungual.
- Painful pustules, nail dystrophy, onycholysis, anonychia.
- May lead to osteolysis.
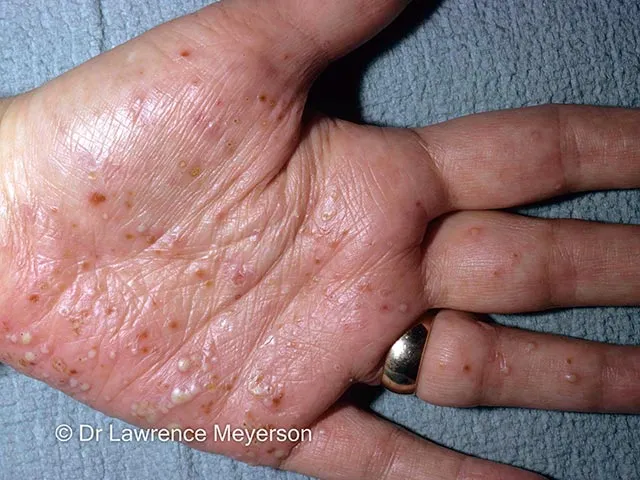
⭐ ACH can cause irreversible bone resorption (osteolysis) of the distal phalanx an_d nail loss (anonychia).
Pathogenesis & Histology - Microscopic Mayhem
- Pathogenesis:
- Genetic: IL36RN mutations (DITRA - Deficiency of IL-36 Receptor Antagonist).
- Triggers: Infections, stress, rapid steroid withdrawal, hypocalcemia, pregnancy.
- Key Cytokines: ↑ IL-36, IL-1, IL-17, IL-23, TNF-α → massive neutrophil chemotaxis.
- Histology:
- Kogoj's spongiform pustules: Hallmark; intraepidermal neutrophil collections.
- Munro's microabscesses: Neutrophils in stratum corneum.
- Epidermis: Acanthosis, parakeratosis.
- Dermis: Papillary edema, perivascular infiltrate (neutrophils, lymphocytes).
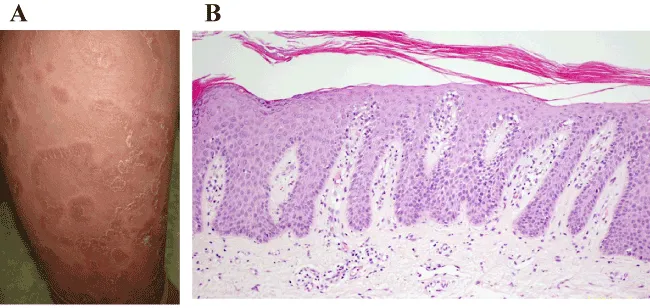
⭐ IL36RN gene mutations are strongly linked to Generalized Pustular Psoriasis (GPP), resulting in DITRA syndrome and uncontrolled IL-36 inflammation.
Diagnosis & Management - Calming the Storm
- Diagnosis:
- Clinical: Sudden widespread sterile pustules, erythema, fever, pain.
- Biopsy: Kogoj's spongiform pustules (key).
- Labs: Leukocytosis (neutrophilia), ↑ESR/CRP, hypocalcemia.
- Management:
- Goals: Rapid pustule clearance, systemic symptom control.
- Supportive: Hydration, electrolyte correction (esp. Ca), emollients.
- GPP (Generalized Pustular Psoriasis): Hospitalize.
- Systemic 1st line: Acitretin (0.5-1 mg/kg/d), Cyclosporine (2.5-5 mg/kg/d), Biologics (e.g., Infliximab, Spesolimab).
- Alternatives: Methotrexate (slower), other biologics (IL-17, IL-23 inhibitors).
- Localized (e.g., Palmoplantar Pustulosis - PPP): Potent topical steroids + Vit D analogs. Refractory: Acitretin.
- ⚠️ Avoid abrupt systemic steroid withdrawal (risk of severe rebound).
⭐ Spesolimab, an IL-36 receptor antibody, is a targeted therapy for GPP flares.
High‑Yield Points - ⚡ Biggest Takeaways
- Generalized Pustular Psoriasis (GPP/von Zumbusch) is an acute, febrile, life-threatening systemic illness.
- Pustules in GPP are widespread, sterile, and develop rapidly on an erythematous base.
- Key GPP triggers: systemic steroid withdrawal, infections, hypocalcemia, pregnancy (impetigo herpetiformis).
- Palmoplantar Pustulosis (PPP) presents with chronic, sterile pustules on palms and soles; strong smoking association.
- Acrodermatitis Continua of Hallopeau (ACH) affects distal digits and nails, potentially leading to onychodystrophy and osteolysis.
- Histopathology classically shows Kogoj's spongiform pustules (subcorneal/intraepidermal neutrophilic aggregates).
- GPP management often requires systemic therapy: acitretin (first-line), cyclosporine, methotrexate, or biologics (e.g., IL-36R inhibitors).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

