Definition & Etiology - Raindrop Eruption
- Definition: An acute, eruptive variant of psoriasis. Presents as multiple, small (0.5-1.5 cm diameter), discrete, erythematous papules and plaques with fine scale. Often described as having a "raindrop" or "dewdrop" appearance. Predominantly affects the trunk and proximal extremities.
- Etiology:
- Primary Trigger:
⭐ Strong association with preceding Group A beta-hemolytic streptococcal (GABHS) infection (e.g., pharyngitis, tonsillitis), typically 2-3 weeks prior.
- Pathomechanism: Likely T-cell mediated immune response; molecular mimicry between streptococcal M proteins and skin keratins is implicated.
- Genetic Predisposition: Strong association with HLA-Cw6.
- Other Factors: Upper respiratory tract viral infections, stress, and rarely, medications can also trigger episodes.
- Primary Trigger:
 erythematous 'raindrop' papules with fine scale on trunk)
erythematous 'raindrop' papules with fine scale on trunk)
Clinical Presentation - Spotting the Shower
- Trigger: Often 1-3 weeks post-streptococcal infection (e.g., pharyngitis).
- Lesions:
- Small, discrete, erythematous papules (0.5-1.5 cm).
- Classic "tear-drop" or "rain-drop" appearance (📌 Gutta = Drop).
- Fine, silvery scales; often thinner than plaque psoriasis.
- Auspitz sign may be positive.
- Distribution:
- Widespread, primarily on trunk & proximal extremities.
- Face, scalp, ears less common; palms/soles usually spared.
- Symptoms: Pruritus common, variable intensity.
- Koebner Phenomenon: Can occur (new lesions at trauma sites).
- Nails/Joints: Typically unaffected.
⭐ Characterized by sudden onset of multiple, small (0.5-1.5 cm), erythematous, scaly papules and plaques resembling "raindrops" (gutta = drop in Latin), primarily on trunk and proximal extremities.
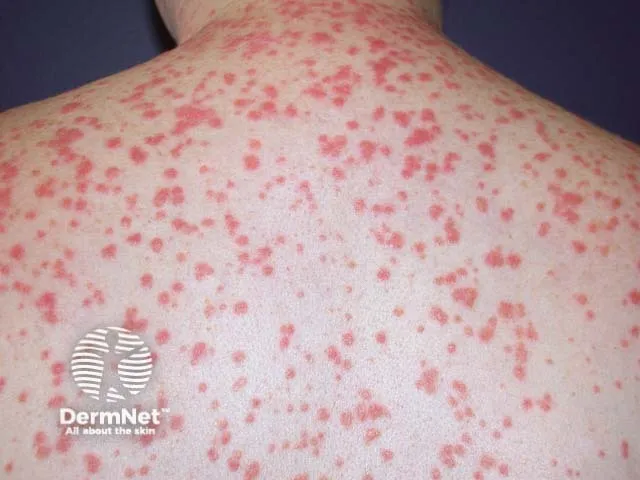
Diagnosis & DDx - Pinpointing Psoriasis
- Clinical Diagnosis: Primarily based on characteristic history (sudden onset, often post-streptococcal infection) and morphology (small, erythematous, scaly papules - "dewdrop" or "raindrop" appearance).
- Investigations:
- Throat swab: For Group A β-hemolytic Streptococcus (GAS).
- ASO titer: ↑ Anti-Streptolysin O titer suggests recent streptococcal infection.
- Biopsy (rarely needed): Shows parakeratosis, Munro's microabscesses, acanthosis, suprapapillary thinning.
⭐ Elevated Anti-Streptolysin O (ASO) titer or positive throat culture for Streptococcus pyogenes supports the diagnosis.
- Differential Diagnosis (DDx):
- Pityriasis rosea: Herald patch, "Christmas tree" pattern, collarette of scale.
- Lichen planus: Purple, polygonal, pruritic papules/plaques (4 P's).
- Secondary syphilis: Papulosquamous lesions, often on palms/soles, serology positive.
- Nummular eczema: Coin-shaped, intensely pruritic plaques.
- Tinea corporis: Annular lesions with central clearing, KOH positive for fungi.
- Drug eruptions: Variable morphology, history of new medication. 📌 Remember DRUGS (Drug Reaction with Eosinophilia and Systemic Symptoms).
Management & Prognosis - Calming the Cascade
- Goals: ↓inflammation, ↓scaling, induce remission.
- Initial/Mild Cases:
- Emollients: Hydration is key.
- Topical corticosteroids: Mild to moderate potency (e.g., fluticasone, triamcinolone) for 2-4 weeks.
- Vitamin D analogues: (e.g., calcipotriol) alone or with steroids.
- Widespread/Severe Cases:
- Phototherapy:
⭐ Narrow-band UVB (NB-UVB) is first-line for widespread guttate psoriasis; often leads to rapid resolution.
- Broad-band UVB (BB-UVB) also effective.
- Systemic therapy (rarely needed, if persistent/severe):
- Methotrexate, cyclosporine, acitretin.
- Biologics (e.g., TNF-α inhibitors) if refractory.
- Phototherapy:
- Prognosis:
- Often self-limiting; resolves in weeks to months (typically 3-4 months).
- ~1/3 develop chronic plaque psoriasis.
- Recurrences possible, especially with new streptococcal infections.
High-Yield Points - ⚡ Biggest Takeaways
- Acute onset of small, "drop-like" (guttate) papules and plaques.
- Commonly triggered by Group A β-hemolytic streptococcal infection, especially pharyngitis, 2-3 weeks prior.
- Predominantly affects the trunk and proximal extremities.
- More frequent in children and young adults.
- Elevated ASO titres are often found.
- Auspitz sign and Koebner phenomenon may be present.
- Often self-limiting, but can precede or coexist with chronic plaque psoriasis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

