Overview & Epidemiology - Ghostly Patches Puzzle
- Benign, self-limiting hypopigmentary disorder.
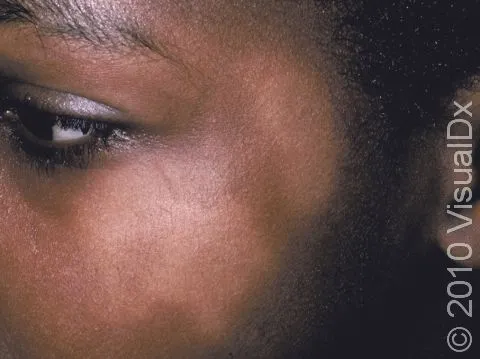
- Presents as ill-defined, round/oval, hypopigmented macules/patches.
- Surface often has fine, adherent scales (powdery).
- Common sites: face (cheeks), neck, upper arms, shoulders.
- More apparent in darker skin, especially after sun exposure (tanning of surrounding skin).
- Associated with atopy, dry skin, sun exposure.
⭐ Most commonly seen in children and adolescents (3-16 years), especially those with a history of atopic dermatitis.
Etiopathogenesis - Sun, Soap, Skin?
- Exact cause remains unknown; considered multifactorial.
- Key proposed factors:
- Sun exposure: Accentuates lesions by tanning perilesional skin.
- Xerosis (dry skin): Frequent washing, harsh soaps may contribute.
- Atopy: Strong association, often co-exists with atopic dermatitis.
- Possible role of Malassezia (Pityrosporum) yeasts (less established).
- Pathophysiology: ↓ melanocyte activity, impaired melanogenesis, and defective melanosome transfer to keratinocytes.
⭐ The exact cause is unknown, but hypopigmentation is attributed to reduced melanocyte activity and defective melanosome transfer, not melanocyte destruction.
Clinical Features - Fading Facework
- Morphology:
- Hypopigmented macules/patches.
- Size: 0.5-5 cm in diameter.
- Borders: Ill-defined, indistinct.
- Surface: Fine, powdery, "branny" or "furfuraceous" scales.
- Common Locations:
- Face (cheeks, perioral area, chin) - hallmark.
- Neck, upper arms, shoulders.
- Symptoms:
- Typically asymptomatic.
- Mild pruritus occasionally reported.
- Evolution:
- More apparent post-sun exposure (surrounding skin tans).
- Early lesions: May show slight erythema/elevation (pityriasis alba papulosa).
- Spontaneous resolution; residual hypopigmentation may persist for months.
⭐ Lesions are typically ill-defined, hypopigmented macules or patches (0.5-5 cm) with fine, often branny or furfuraceous scales, most commonly on the face (cheeks, perioral, chin).
Diagnosis & DDx - Ruling Rivals Out
- Clinical: Ill-defined, hypopigmented macules with fine scales. Often on face/extensors in atopic children.
- Wood's Lamp: Accentuates hypopigmentation; no fluorescence.
⭐ Wood's lamp in Pityriasis Alba shows hypopigmentation accentuation, no fluorescence, differentiating from Tinea versicolor (yellow-green fluorescence).
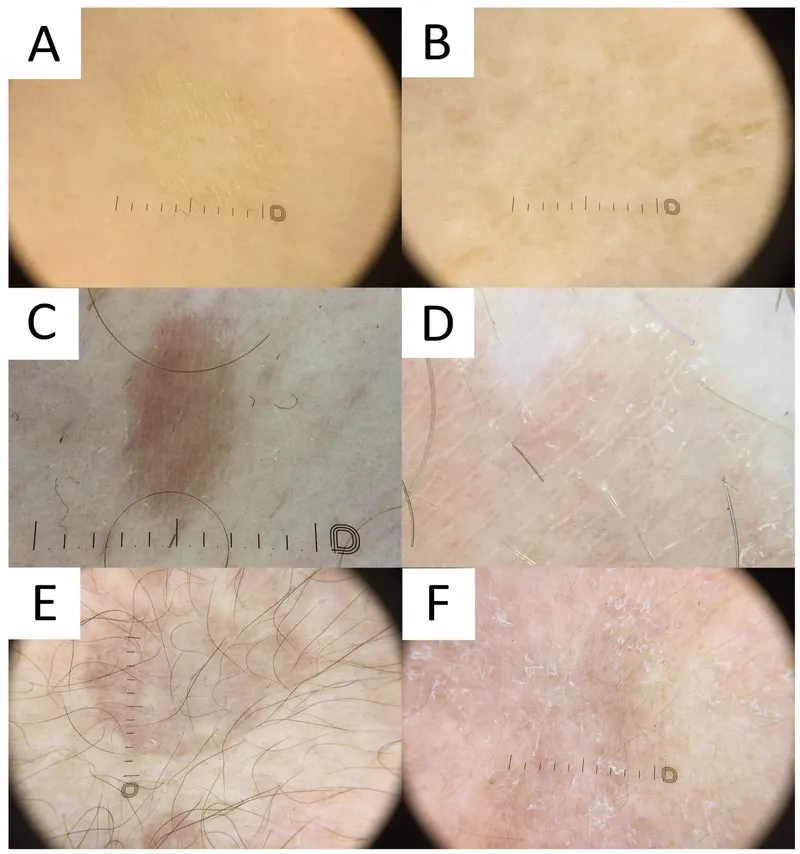
- Differential Diagnosis (DDx):
📌 Mnemonic: 'Very White Patches Need Thorough Looking'
Condition Key Differentiators Vitiligo Depigmented (milk-white), well-defined, Wood's: accentuates P. Versicolor Sharp borders, fine scales, Wood's: yellow-green fluorescence Post-inflam. Hypopig. History of prior rash Nevus Depigmentosus Congenital, stable, no scale Tuberculoid Leprosy Anesthetic/hypoesthetic, nerve thickening
Management & Prognosis - Fading Fixes
- Primary Goal: Reassurance, cosmetic improvement.
- General Measures:
- Emollients: Hydrate skin.
- Sunscreen: Prevent further tanning of surrounding skin, making lesions less apparent.
- Pharmacological (if needed):
- Low-potency topical corticosteroids (e.g., hydrocortisone 1%): Short-term for mild inflammation/scaling.
- Topical Calcineurin Inhibitors (TCIs): Pimecrolimus 1% cream, Tacrolimus 0.03% or 0.1% ointment; preferred for face.
- Prognosis: Generally good; lesions resolve spontaneously over months to years. Hypopigmentation may persist longer.
⭐ Management primarily involves reassurance, emollients, and sun protection. Topical calcineurin inhibitors are preferred for facial lesions to avoid steroid-induced atrophy.
High‑Yield Points - ⚡ Biggest Takeaways
- Common, benign condition with ill-defined, hypopigmented patches and fine scales.
- Primarily affects children and young adults, especially on the face and upper limbs.
- Strong association with atopic dermatitis and xerosis (dry skin).
- Lesions are more noticeable after sun exposure due to surrounding skin tanning.
- Diagnosis is clinical; Wood's lamp is typically negative for fluorescence, differentiating from tinea versicolor.
- Management: reassurance, emollients, sun protection; low-potency topical steroids if inflamed.
- Usually self-resolves, though repigmentation can be slow, taking months to a year.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

