Nevi of Ota and Ito - Blue-Gray Badges
- Definition: Dermal melanocytoses presenting as congenital or acquired blue-gray hyperpigmentation.
- Nevus of Ota:
- Affects skin and mucous membranes innervated by trigeminal nerve branches.
- Common sites: Periocular skin, sclera, conjunctiva, tympanic membrane.
- 📌 Ota: Ocular/Ophthalmic involvement.
⭐ Involves areas of trigeminal nerve branches V1 (ophthalmic) & V2 (maxillary).
- Nevus of Ito:
- Affects shoulder, neck, supraclavicular, and scapular regions.
- Distribution: Posterior supraclavicular and lateral cutaneous brachial nerves.
- Features: Usually unilateral. Monitor for glaucoma and melanoma (rare).
 and Nevus of Ito (shoulder/neck) showing characteristic blue-gray pigmentation) G
and Nevus of Ito (shoulder/neck) showing characteristic blue-gray pigmentation) G
Nevi of Ota and Ito - The Who & Why
- Pathogenesis:
- Arrested migration of melanocytes from neural crest to epidermis during embryogenesis. Melanocytes remain in dermis, causing dermal melanocytosis.
- Epidemiology:
- Prevalence: Higher in Asian populations.
- Gender: Predominantly affects females (F:M ratio ~5:1).
- Age of Onset:
- Congenital: ~50% present at birth or within first year.
- Acquired: Can appear later, often around puberty or during pregnancy.
⭐ Associated with somatic mutations in GNAQ or GNA11 genes. Ocular melanocytosis (in Nevus of Ota) increases uveal melanoma risk.
Nevi of Ota and Ito - Spotting the Spots
- Congenital/early onset dermal melanocytoses; blue-gray, slate-gray, or brownish, mottled macules/patches.
- Nevus of Ota:
- Distribution: Typically unilateral, periorbital (V1/V2 trigeminal dermatomes).
- Involvement: Sclera (ocular melanocytosis), conjunctiva, tympanic membrane, nasal/oral mucosa.
⭐ Ocular melanocytosis (blue or gray scleral discoloration) is a hallmark; can be bilateral in ~10% of cases.
- Nevus of Ito:
- Distribution: Unilateral; supraclavicular, deltoid, scapular regions.
- Differential Diagnosis (DDx):
- Hori’s Nevus (ABNOM): Acquired, bilateral, malar/temple macules; no mucosal/scleral involvement.
- Mongolian Spot: Congenital, lumbosacral, usually fades in childhood.
- Melasma: Acquired, symmetrical facial hyperpigmentation.
- Drug-induced pigmentation.

Nevi of Ota and Ito - Beyond the Blue
- Associated Conditions & Complications:
- Glaucoma: Especially with ocular/palpebral involvement in Nevus of Ota. Annual screening vital.
- Malignant Transformation (Rare, but serious; higher risk in Caucasians with Ota):
- Uveal melanoma (most common ocular malignancy)
- Cutaneous melanoma
- CNS melanoma
- Sensorineural hearing loss (rarely reported).
- Phakomatosis pigmentovascularis (co-occurrence with vascular malformations like Sturge-Weber).
⭐ Patients with Nevus of Ota, particularly Caucasians, have an increased lifetime risk of developing uveal melanoma and glaucoma.

Nevi of Ota and Ito - Clearing the Canvas
- Diagnosis: Primarily clinical. Wood's lamp examination and dermoscopy assist.
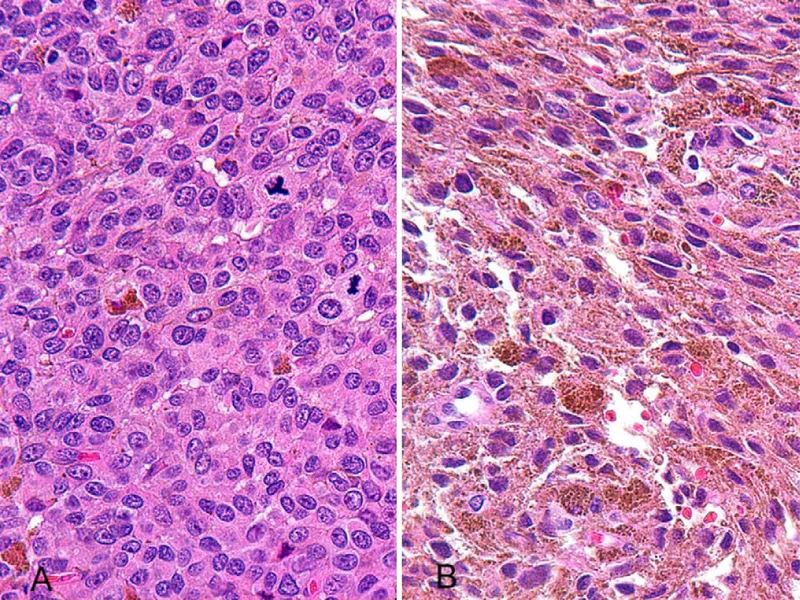
- Biopsy if atypical or malignancy concern: reveals dermal melanocytes without nevus cells.
- Management:
- Observation for stable lesions.
- Cosmetic camouflage for concealment.
- Laser therapy: Q-switched Ruby, Alexandrite, Nd:YAG (e.g., 1064 nm) lasers. Multiple sessions are typically required.
- Follow-up: Regular ophthalmologic (glaucoma risk) and dermatologic (melanoma risk) surveillance is crucial.

⭐ Q-switched lasers (e.g., Nd:YAG, Ruby, Alexandrite) are the treatment of choice for cosmetic improvement, targeting dermal melanocytes.
High‑Yield Points - ⚡ Biggest Takeaways
- Nevus of Ota: Trigeminal (V1/V2) distribution; Nevus of Ito: Shoulder/neck (supraclavicular/deltoid).
- Both are dermal melanocytoses; bluish-grey patches, often congenital/early onset.
- Ocular melanocytosis (sclera) common in Ota, linked to ↑ glaucoma risk.
- Oral mucosal pigmentation possible in Nevus of Ota.
- Rare malignant transformation to melanoma (uveal, cutaneous), higher in Ota.
- Q-switched lasers for cosmetic improvement; regular eye exams for Ota patients monitoring for glaucoma and melanoma development.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

