Phototherapy Basics - Ray Foundations
- Phototherapy: Utilizes non-ionizing electromagnetic radiation, mainly ultraviolet (UV) light, for therapeutic effects on skin.
- Key UV Bands & Skin Interaction:
- UVA: 320-400 nm. Longest wavelength, penetrates deepest (dermis).
- UVA1: 340-400 nm; UVA2: 320-340 nm.
- UVB: 290-320 nm. Biologically most active for skin diseases; penetrates epidermis.
- NB-UVB (Narrowband): 311-313 nm, highly effective.
- UVC: 200-290 nm. Germicidal; mostly filtered by Earth's ozone layer.
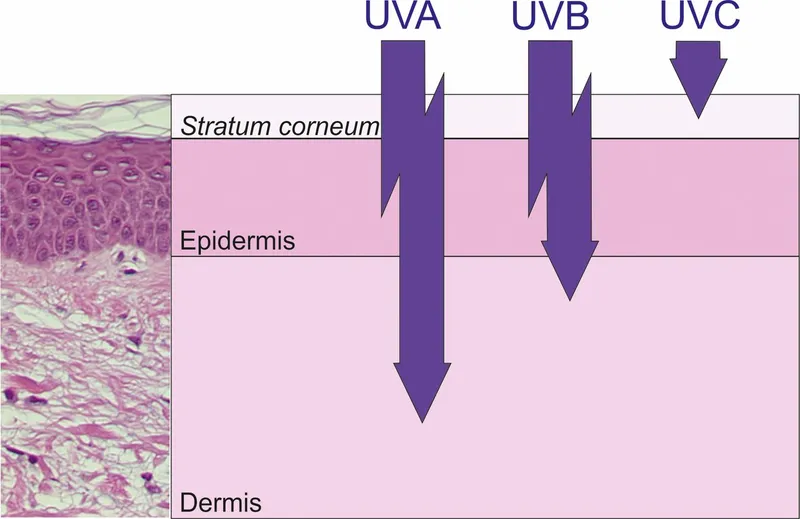
- UVA: 320-400 nm. Longest wavelength, penetrates deepest (dermis).
⭐ Action spectrum for psoriasis treatment is most effective around 311 nm (NB-UVB).
NB-UVB Therapy - Narrow-Beam Power
- Wavelength: 311-313 nm (peak emission).
- Mechanism: Primarily immunomodulatory (affects T-cells, cytokines). Antiproliferative.
- Key Uses: Psoriasis, vitiligo, atopic dermatitis, early mycosis fungoides.
- Starting Dose Strategy:
- Skin type-based: e.g., Type I-II: 0.1-0.2 J/cm²; Type III-IV: 0.2-0.3 J/cm²; Type V-VI: 0.3-0.4 J/cm².
- MED-based: Typically 70% of Minimal Erythema Dose (MED).
- Regimen: 2-3 sessions/week. Dose increment 10-20% per session (guided by erythema).
- Advantages: More effective & safer than broadband UVB. No psoralens required (unlike PUVA).
- Considerations: Erythema, pruritus common. Monitor cumulative exposure for long-term photoaging.

⭐ NB-UVB is a first-line phototherapy for moderate-to-severe psoriasis due to its efficacy and favorable safety profile.
PUVA Therapy - Psoralen Power-Up
Psoralen + UVA (320-400nm). Psoralens (e.g., 8-Methoxypsoralen/8-MOP) are photosensitizers.
- Mechanism: Psoralen intercalates DNA; UVA activation cross-links DNA, inhibiting cell proliferation.

- Key Details:
- Oral 8-MOP: 0.6 mg/kg, 1.5-2 hrs before UVA.
- Delivery: Oral, bath, topical.
- Indications: Severe psoriasis, vitiligo, mycosis fungoides.
- Side Effects:
- Acute: Nausea, phototoxic erythema.
- Chronic: Photoaging, ↑ skin cancer risk (SCC). 📌 PUVA Problems: Pigment changes, UV sensitivity, Vomiting, Aging/Malignancy.
- Protection: UVA-blocking eyewear for 24 hrs post-psoralen.
⭐ Long-term PUVA significantly increases squamous cell carcinoma (SCC) risk.
Targeted Phototherapy & PDT - Precision Beams
- Targeted Phototherapy: Delivers UV to lesions, spares healthy skin.
- Excimer Laser: 308 nm (XeCl).
- Indications: Localized psoriasis, vitiligo, alopecia areata, mycosis fungoides.
- Rapid, high fluence.
- Excimer Lamp: 308 nm. Larger spot.
- Excimer Laser: 308 nm (XeCl).
- Photodynamic Therapy (PDT):
- Mechanism: Photosensitizer + Light + O₂ → ROS → cell death.
- Photosensitizers: Topical 5-ALA, MAL.
- Light: Blue (~417 nm for ALA), Red (~635 nm for MAL).
- Indications: Actinic keratosis (AK), superficial Basal Cell Carcinoma (sBCC), Bowen's disease.
- Pain during illumination.
⭐ Excimer laser allows rapid delivery of high fluences to affected skin, sparing normal skin.
oka
Protocol Pointers & Safety - Charting Choices
| Modality | λ (nm) | Pro | Con | Eye Shield |
|---|---|---|---|---|
| NB-UVB | 311-313 | Good safety, home use option | Slower onset | During Tx |
| PUVA | UVA + Psoralen | High efficacy, deep effect | ↑ Skin Ca risk, nausea | During & 24h post |
| Excimer Laser | 308 | Targeted, rapid for patches | Small areas, costly | During Tx |
High‑Yield Points - ⚡ Biggest Takeaways
- NBUVB (311-313 nm): Preferred for psoriasis, vitiligo due to high efficacy & safety.
- PUVA: Psoralens (oral/topical) followed by UVA (320-400 nm); potent but with risks.
- MED (Minimal Erythema Dose): Essential for determining initial UVB therapy dose.
- Long-term PUVA significantly ↑ risk of photoaging & squamous cell carcinoma (SCC).
- Classic regimens for psoriasis: Goeckerman (crude coal tar + UVB) & Ingram (anthralin + UVB).
- Standard phototherapy frequency is 2-3 sessions per week.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

