Genodermatoses Overview - Gene Skin Basics
- Genodermatoses: Group of inherited skin conditions, primarily monogenic (single gene defects), affecting skin structure/function.
- Key Inheritance Patterns:
- Autosomal Dominant (AD): Vertical transmission, 50% offspring risk. E.g., Ichthyosis vulgaris.
- Autosomal Recessive (AR): Horizontal, 25% risk; consanguinity ↑ risk. E.g., Xeroderma pigmentosum.
- X-linked Recessive (XLR): Males affected, carrier females. E.g., Anhidrotic ectodermal dysplasia.
- X-linked Dominant (XLD): Rare. E.g., Incontinentia pigmenti.
- Broad Categories: Disorders of keratinization (e.g., Ichthyoses), epidermolysis bullosa group, pigmentation disorders (e.g., Albinism), DNA repair defects (e.g., Xeroderma Pigmentosum), neurocutaneous syndromes (e.g., Neurofibromatosis).
⭐ Most genodermatoses manifest at birth or in early childhood, aiding early diagnosis.
Ichthyoses & Keratinopaths - Scaly Skin Tales
- Ichthyoses: Genetic disorders of keratinization causing "fish-scale skin".
- Common Types:
- Ichthyosis Vulgaris (IV): Most common, AD. Fine, white scales; spares flexures. Filaggrin (FLG) gene. Atopy link.
- X-Linked Ichthyosis (XLI): Steroid sulfatase (STS) deficiency. Dark, adherent scales (neck, trunk).
- Lamellar Ichthyosis (LI): AR. Collodion baby. Large, dark, plate-like scales. TGM1 gene. Ectropion.
- Epidermolytic Ichthyosis (EI): AD. Keratin 1/10 (KRT1/KRT10) defects. Neonatal blistering → hyperkeratosis.
⭐ "Collodion baby" at birth is highly suggestive of Autosomal Recessive Congenital Ichthyosis (ARCI), like Lamellar Ichthyosis (LI) or Congenital Ichthyosiform Erythroderma (CIE).
Epidermolysis Bullosa - Fragile Skin Saga
- Group of inherited mechanobullous disorders characterized by skin fragility and blister formation with minimal trauma.
- Classified by the level of skin cleavage within or below the dermo-epidermal junction:
- EB Simplex (EBS): Intraepidermal cleavage (e.g., Keratin 5, 14 defects). Blisters typically heal without scarring.
- Junctionional EB (JEB): Cleavage within lamina lucida (e.g., Laminin-332 defects). Severe forms (e.g., Herlitz) can be lethal.
- Dystrophic EB (DEB): Cleavage in sublamina densa (Collagen VII defects). Leads to scarring, milia, and nail dystrophy.
- Kindler Syndrome: Mixed/variable cleavage planes (Kindlin-1 defect). Features blistering, poikiloderma, photosensitivity.
- Management focuses on gentle skin care, wound management, and preventing infection and trauma.

⭐ Recessive Dystrophic Epidermolysis Bullosa (RDEB) is notorious for causing severe scarring, leading to pseudosyndactyly ("mitten" deformities of hands and feet) and an increased risk of aggressive squamous cell carcinoma by early adulthood due to COL7A1 gene mutations affecting Type VII collagen production and anchoring fibril formation.
Neurocutaneous Syndromes - Brain & Skin Links
Also known as phakomatoses; genetic disorders affecting skin, CNS, and other organs.
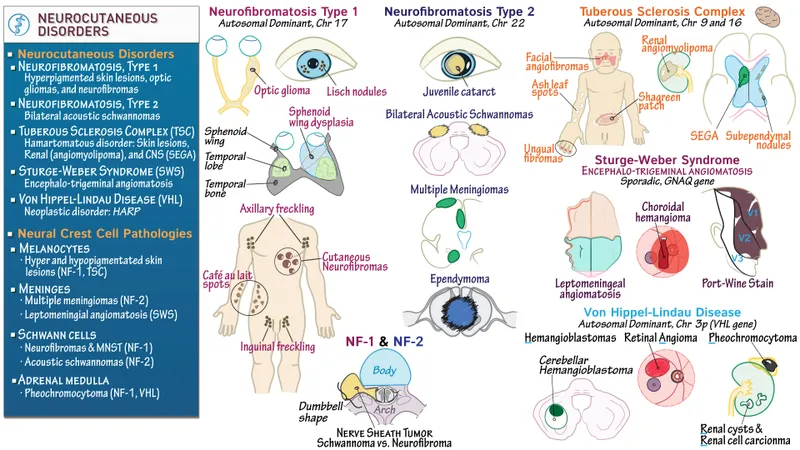
- Neurofibromatosis Type 1 (NF1)
- Skin: ≥6 Café-au-lait macules (CALMs), axillary/inguinal freckling (Crowe sign), neurofibromas, Lisch nodules (iris hamartomas).
- Neuro: Optic pathway gliomas, learning disabilities.
- Gene: NF1 (Chr 17).
- Tuberous Sclerosis Complex (TSC)
- Skin: Ash-leaf spots (hypopigmented macules), facial angiofibromas (adenoma sebaceum), shagreen patch, periungual fibromas (Koenen tumors).
- Neuro: Cortical tubers, subependymal nodules (SEN), subependymal giant cell astrocytomas (SEGA), seizures (infantile spasms).
- Genes: TSC1 (hamartin) / TSC2 (tuberin).
- Sturge-Weber Syndrome (SWS)
- Skin: Port-wine stain (nevus flammeus) typically in V1 trigeminal nerve distribution.
- Neuro: Leptomeningeal angiomatosis, seizures, intellectual disability, glaucoma.
⭐ Classic "tram-track" calcifications on skull imaging are characteristic of Sturge-Weber Syndrome due to cortical atrophy and dystrophic calcification along gyri adjacent to the leptomeningeal angioma.
High‑Yield Points - ⚡ Biggest Takeaways
- Ichthyosis vulgaris: Most common; AD, filaggrin defect; dry, scaly skin.
- Epidermolysis bullosa: Blistering on minor trauma; multiple types.
- Neurofibromatosis-1: Café-au-lait macules, neurofibromas, Lisch nodules; AD.
- Tuberous Sclerosis: Ash-leaf spots, shagreen patch, facial angiofibromas; AD.
- Oculocutaneous Albinism: Often tyrosinase deficiency; ↑ skin cancer risk.
- Xeroderma Pigmentosum: AR; defective DNA repair; extreme sun sensitivity & malignancy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

