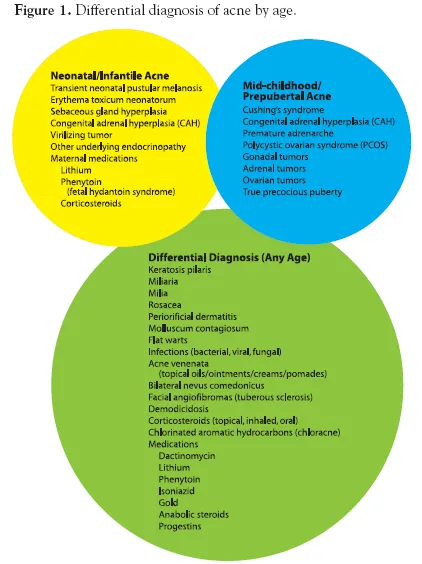
Acne Ages - Tiny Pimples, Big Stages
- Neonatal (Birth-8 wks): Transient facial papules/pustules, few comedones. Maternal/neonatal androgens. Usually resolves spontaneously.
⭐ Neonatal acne is typically transient and benign, often resolving spontaneously.
- Infantile (6 wks-1 yr): More inflammatory lesions, comedones prominent. ↑DHEAS, LH-driven androgens. Risk of scarring.
- Mid-Childhood (1-<7 yrs): RARE. Comedones, papules. Always investigate for hyperandrogenism (e.g., premature adrenarche, CAH).
- Pre-Adolescent/Adolescent (≥7 yrs): Common. Comedones, inflammatory lesions. Due to pubertal androgens, P. acnes.
Pimple Genesis - Acne's Core Four
📌 'FOIL' for Pathogenesis: Follicular hyperkeratinization, Oil (Sebum overproduction), Inflammation, 'Libacter' (Cutibacterium acnes).
- Follicular hyperkeratinization: Accelerated shedding & cohesion of keratinocytes obstructs the pilosebaceous duct, forming the initial microcomedone.
- Oil (Sebum) overproduction: Androgenic hormones (especially during puberty) stimulate sebaceous glands, leading to increased sebum secretion.
- Inflammation: Triggered by C. acnes and sebum-derived lipids, involving innate and adaptive immune responses, leading to papules, pustules, nodules.
- Libacter (Cutibacterium acnes): This anaerobic bacterium colonizes the lipid-rich environment of the follicle, metabolizing sebum and releasing pro-inflammatory mediators.

⭐ Androgens are key drivers, stimulating sebaceous glands to produce more sebum, a critical factor in acne development.
Acne Detectives - Lesions & Lineup
Key Lesion Types & Characteristics:
| Type | Description |
|---|---|
| Non-Inflammatory | |
| Open Comedone | Blackhead: dilated follicle, oxidized keratin. |
| Closed Comedone | Whitehead: clogged follicle, inflammation precursor. |
| Inflammatory | |
| Papule | <5mm, solid, erythematous, raised. |
| Pustule | Pus-filled papule. |
| Nodule | >5mm, deep, firm, painful. |
| Cyst | Suppurative, fluctuant nodule; scarring risk. |
⭐ The presence of comedones is pathognomonic for acne vulgaris.
- Look For: Polymorphic lesions (comedones, papules, pustules often coexist), distribution (face, chest, back), presence of scarring, and signs of endocrinopathy (e.g., hirsutism, irregular menses - consider hyperandrogenism).
Acne Arsenal - Clearing the Coast
- Goal: ↓ lesions, scarring, psychosocial impact via tailored therapy.
- Topical Agents (First-line for mild-moderate):
- Retinoids (Tretinoin, Adapalene): Normalize keratinization.
- Benzoyl Peroxide (BPO): Antibacterial, comedolytic.
- Topical Antibiotics (Clindamycin): Use with BPO (↓ resistance).
- Azelaic Acid: Antibacterial, anti-inflammatory, comedolytic.
- Systemic Agents (Moderate-severe, or resistant):
- Oral Antibiotics (Doxycycline, Azithromycin): Min. 6-8 weeks.
- Oral Isotretinoin: For severe, nodulocystic/scarring acne. Dose: 0.5-1 mg/kg/day. ⚠️ Teratogenic.
- Hormonal (OCPs, Spironolactone): For females with PCOD signs/late acne.
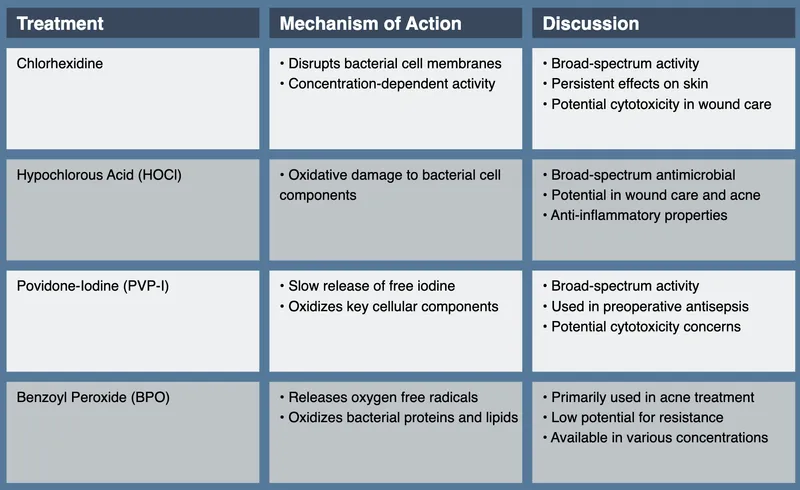
⭐ Systemic isotretinoin is highly effective for severe, nodulocystic acne but is a potent teratogen requiring strict contraception (e.g., two reliable methods) in females of childbearing potential.
High‑Yield Points - ⚡ Biggest Takeaways
- Neonatal acne: Self-limiting, no comedones. Infantile acne: Comedones present, may scar, consider endocrinopathy if severe.
- Mid-childhood acne (1-7 years): Rare, mandates endocrine evaluation (e.g., CAH, precocious puberty).
- Adolescent acne pathogenesis: Cutibacterium acnes, ↑sebum, follicular hyperkeratinization, inflammation.
- First-line therapy: Topical retinoids (e.g., adapalene) and benzoyl peroxide.
- Severe/nodulocystic acne: Oral isotretinoin is key; monitor side effects (teratogenicity, LFTs, lipids).
- PCOS: Suspect in adolescent females with acne, hirsutism, and menstrual irregularities.
- Tetracyclines (Doxycycline, Minocycline): Contraindicated in children <8 years due to teeth staining and bone effects.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

