Myiasis Basics - Buggy Intruders
- Infestation of live human/animal tissue by dipterous (fly) larvae (maggots).
- Causative agents: Various fly species; common ones include Dermatobia hominis (human botfly), Cordylobia anthropophaga (tumbu fly), Cochliomyia hominivorax (New World screwworm).
- Classification based on larval behavior:
- Obligatory: Larvae require living tissue for development (e.g., D. hominis).
- Facultative: Larvae can develop in living or dead tissue (e.g., some Sarcophagidae).
- Accidental: Larvae ingested/enter via orifices, typically don't complete development.
⭐ Cochliomyia hominivorax (New World screwworm) causes obligatory myiasis and is a reportable disease due to its aggressive tissue destruction and potential for severe economic impact on livestock.
- Clinical forms: Furuncular, wound/traumatic, cavitary, migratory, intestinal, urogenital myiasis based on site of infestation and larval behavior.
Culprit Flies - The Buzzing Baddies
-
Obligatory Parasites (Need Living Tissue):
- Dermatobia hominis (Human Botfly): Furuncular lesions. Phoresis via mosquitoes.
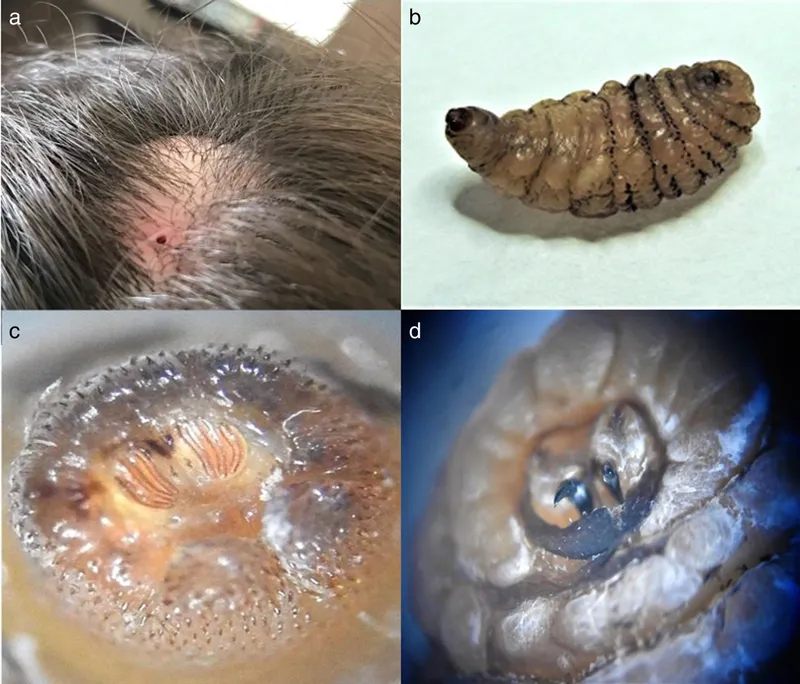
- Cordylobia anthropophaga (Tumbu Fly): African furuncular myiasis; eggs on soil/clothes.
- Cochliomyia hominivorax (New World Screwworm): Destructive wound myiasis.
- Chrysomya bezziana (Old World Screwworm): Old World screwworm; wound myiasis.
⭐ Dermatobia hominis larvae possess backward-pointing spines, aiding firm anchorage within the host's skin.
- Dermatobia hominis (Human Botfly): Furuncular lesions. Phoresis via mosquitoes.
-
Facultative Parasites (Usually Dead Tissue; Can Invade Wounds):
- Lucilia spp. (Greenbottle), Calliphora spp. (Bluebottle), Sarcophaga spp. (Flesh fly).
-
Specific Presentations:
- Gasterophilus intestinalis: Creeping eruption (larva migrans cutanea).
- Oestrus ovis (Sheep Botfly): Ophthalmomyiasis, nasopharyngeal myiasis.
Clinical Picture - Skin's Squirmy Story
- Furuncular Myiasis: Most common.
- Boil-like, erythematous nodule.
- Central punctum (breathing pore); serosanguinous discharge.
- Movement sensation, pain, itching.
- Agents: Dermatobia hominis (botfly), Cordylobia anthropophaga (tumbu fly).
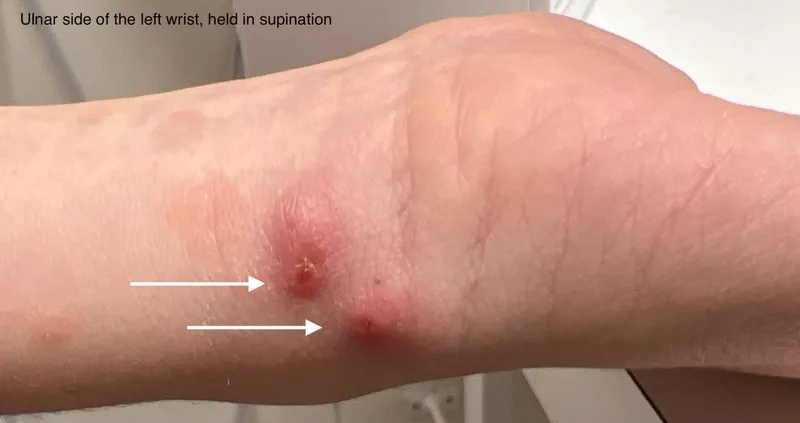
- Wound (Traumatic) Myiasis: Larvae infest open wounds, ulcers, necrotic tissue.
- Creeping (Migratory) Myiasis:
- Larva burrows; serpiginous, erythematous tracts.
- Itchy, raised linear lesions.
- Agents: Gasterophilus spp. (horse botfly), Hypoderma spp. (cattle botfly).
- Cavitary Myiasis: Infests body cavities (nasal, aural, oral, ocular, urogenital).
- Destructive; site-specific symptoms.
- Sanguinivorous Myiasis: Larvae feed on blood (e.g., Auchmeromyia luteola - Congo floor maggot). Rare.
⭐ Furuncular myiasis often presents with a characteristic central punctum from which the larva's posterior spiracles may be visible, aiding diagnosis.
Spotting & Nabbing - Larva Eviction Plan
- Spotting:
- Look for: Central punctum, visible larva/movement, serosanguinous discharge.
- Tools: Dermoscopy, Ultrasound (confirms depth/viability).
- Nabbing (Eviction):
- Occlusion: Apply petroleum jelly/liquid paraffin to block spiracles; larva surfaces.
- Extraction: Gentle pressure, forceps. Surgical removal if needed.
- Systemic: Oral Ivermectin (200 µg/kg) for extensive/cavitary myiasis.
- Post-Op: Wound care, antibiotics if infected, tetanus prophylaxis. 📌 Mnemonic: "SOS" - Suffocate (Occlude), Operate (Extract), Systemic (Ivermectin if severe).
⭐ Dermatobia hominis larvae often require several hours of occlusion before emerging; patience is key during this step for successful non-invasive removal.
Prevention & Control - Fly-Free Zone Tactics
- Environmental hygiene:
- Proper waste/carcass disposal.
- Eliminate fly breeding sites (decaying matter).
- Personal protection:
- Insect repellents (DEET).
- Protective clothing in endemic areas.
- Window/door screens.
- Animal husbandry:
- Prompt wound care in animals.
- Controlled insecticide use on livestock.
- Community measures:
- Fly traps, baits.
⭐ Human botfly (Dermatobia hominis) uses mosquitoes as phoretic vectors for egg delivery to hosts.
High‑Yield Points - ⚡ Biggest Takeaways
- Myiasis: Infestation of live vertebrate tissue by dipterous larvae (maggots).
- Key types: Furuncular (boil-like, central punctum), wound/traumatic, and cavitary (nasal, aural).
- Caused by larvae of Dermatobia hominis (human botfly) and Cordylobia anthropophaga (tumbu fly).
- Screwworm myiasis (Cochliomyia, Chrysomya) is highly destructive, often in wounds.
- Diagnosis: Direct visualization of larvae; occlusion (e.g., petroleum jelly) aids emergence.
- Management: Mechanical removal of larvae is primary; oral ivermectin as adjunct_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

