Leishmaniasis Basics - Sandfly's Sting
- Protozoan disease by Leishmania spp.; transmitted by female Phlebotomus sandfly bite.
- Key Indian Species:
- L. donovani (Visceral Leishmaniasis/Kala-azar)
- L. tropica (Cutaneous Leishmaniasis)
- Vector: Phlebotomus argentipes (main vector for VL in India).
- Life Cycle:
- Sandfly: Ingests amastigotes → develop to promastigotes (infective).
- Human: Promastigotes injected → transform to amastigotes in macrophages (diagnostic).
- Endemic (India): Bihar, Jharkhand, West Bengal, E. Uttar Pradesh.

⭐ Diagnostic stage: Amastigotes (Leishman-Donovan bodies) within human macrophages.
Disease Spectrum - Skin & Spleen Saga
-
Visceral Leishmaniasis (Kala-azar / Black Fever)
- Agent: L. donovani (India).
- Incubation: 2-6 months (variable).
- Classic Triad:
- Prolonged fever (>2 weeks).
- Massive splenomegaly (± hepatomegaly).
- Progressive weight loss, cachexia.
- Lab: Pancytopenia (↓Hb, ↓WBC, ↓Platelets), polyclonal hypergammaglobulinemia (↑IgG).
- Post-Kala-azar Dermal Leishmaniasis (PKDL):
- Hypopigmented macules, papules, nodules, plaques.
- Appears 6 months - 2 years (or more) post-VL treatment.
- Important reservoir of infection.
-
Cutaneous Leishmaniasis (CL)
- Agents: L. tropica, L. major.
- Forms:
- Localized (LCL): "Oriental Sore", "Delhi Boil". Most common.
- Diffuse (DCL): Anergic, widespread nodules.
- Recidivans (LR): Chronic, relapsing at scar edge.
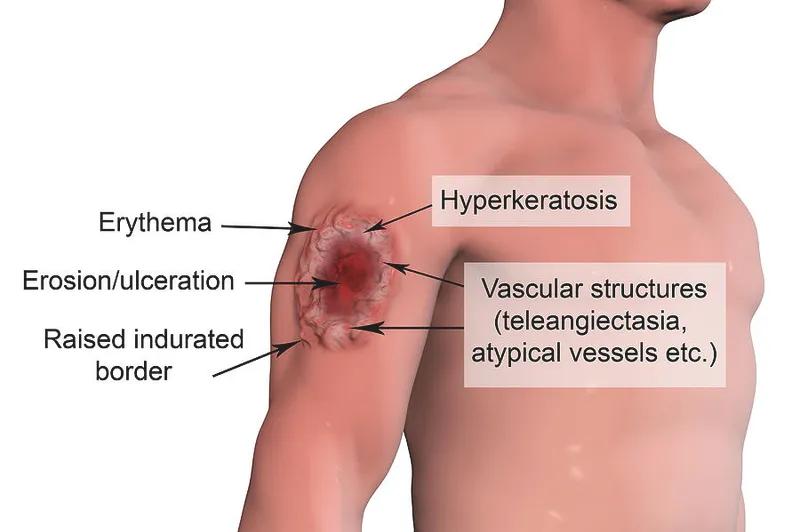
- Lesion: Starts as papule → nodule → painless ulcer with raised, indurated "volcano-like" border; may be dry or crusted.
- Sites: Exposed areas (face, limbs).
-
Mucocutaneous Leishmaniasis (MCL)
- Rare in India (primarily New World: L. braziliensis).
- If occurs with L. donovani, involves destructive lesions of nasal, oral, pharyngeal mucosa.
⭐ > Amastigotes (Leishman-Donovan bodies) are found within macrophages in tissue samples (spleen, bone marrow, skin).
Spotting the Parasite - Detective Work

- Visceral Leishmaniasis (VL):
- Definitive Dx: LD bodies (Giemsa stain) in aspirates (spleen - highest yield, bone marrow, lymph node).
- Serology: rK39 strip test (rapid), DAT, ELISA.
- Molecular: PCR (high sensitivity, species ID).
- Cutaneous/Mucocutaneous (CL/MCL):
- Microscopy: LD bodies in slit-skin smear/tissue imprint (Giemsa).
- Biopsy for:
- Histopathology (LD bodies).
- Culture (NNN medium).
- Molecular: PCR (species ID).
- Montenegro Skin Test (Leishmanin):
- Measures CMI; induration ≥5mm = positive.
- Positive: Most CL (not DCL), cured VL. Negative: Active VL, DCL.
⭐ The rK39 antigen-based immunochromatographic test is a highly sensitive and specific rapid diagnostic for Visceral Leishmaniasis, crucial in resource-limited settings.
Fighting Back - Drugs & Defense
Treatment:
- Visceral Leishmaniasis (VL / Kala-azar):
- First-line: Liposomal Amphotericin B (LAmB) (e.g., 10 mg/kg single IV dose - India); Miltefosine (2.5 mg/kg/day PO, 28 days, ⚠️ Teratogenic); Paromomycin IM.
- Combination therapy (LAmB + Miltefosine or LAmB + Paromomycin) for ↑efficacy, ↓resistance, esp. in endemic areas.
- Sodium Stibogluconate (SSG): Marked resistance in Indian subcontinent.
- Cutaneous Leishmaniasis (CL):
- Local: Paromomycin ointment, intralesional SSG, cryotherapy, heat therapy.
- Systemic (severe/unresponsive): Miltefosine, SSG (if sensitive), azoles (e.g., Ketoconazole).
- Post-Kala-azar Dermal Leishmaniasis (PKDL):
- Miltefosine or LAmB (often prolonged course, e.g., 12 weeks for Miltefosine).
⭐ Miltefosine: First effective and exclusively oral drug for visceral leishmaniasis.
Prevention & Control:
- Vector (Sandfly) Control: Indoor Residual Spraying (IRS) (e.g., DDT, synthetic pyrethroids), environmental hygiene.
- Personal Protection: Insecticide-treated nets (ITNs), repellents (e.g., DEET).
- Early case detection & complete treatment.
- Health education on disease transmission & personal protection measures.
High‑Yield Points - ⚡ Biggest Takeaways
Error: Failed to generate content for this concept group.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

