Cutaneous Amebiasis: Intro - Amebic Invader Alert
- What: A rare, aggressive parasitic infection of the skin.
- Invader: Caused by the protozoan Entamoeba histolytica, primarily its trophozoite form.
- Invasion Routes:
- Direct skin inoculation (e.g., trauma, surgery).
- Extension from deeper amebic foci (e.g., liver abscess, intestinal disease).
- Hematogenous spread (less common).
- Red Flag: Its presence often indicates severe underlying visceral amebiasis or compromised immunity.
- Typically presents as painful, rapidly destructive ulcers.
⭐ Cutaneous amebiasis is a rare but severe extraintestinal manifestation of Entamoeba histolytica infection, often indicating underlying visceral involvement or direct inoculation.
Cutaneous Amebiasis: Clinical Signs - Skin's Sore Story
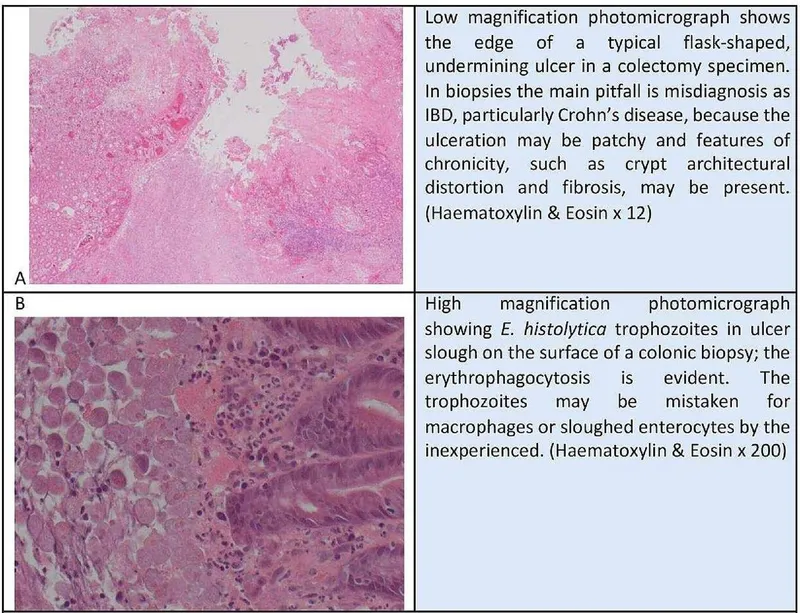
- Onset: Often a painful papule/pustule.
- Evolution: Rapid progression to ulcer with significant tissue destruction.
- Ulcer Features:
- Edges: Sharply defined, raised, violaceous, undermined ("cliff-edge").
- Base: Necrotic debris, pus, or blood-tinged, foul-smelling exudate.
- Shape: Irregular, serpiginous, or amoeboid.
- Surrounding: Erythema, edema.
- Hallmark Symptom: Severe, persistent pain, often disproportionate to lesion size.
- Predilection Sites:
- Perianal, perineal, genital (most common; direct extension/autoinoculation).
- Abdominal wall (post-surgery for amoebic liver abscess, colostomies).
- Less common: Buttocks, legs, face.
- Systemic: Fever, malaise, weight loss possible with extensive disease.
- Rare: Amebiasis cutis anserina (follicular papules like gooseflesh).
⭐ The characteristic lesion is a rapidly progressive, painful ulcer with undermined, ragged edges and a necrotic, often blood-tinged, base.
Cutaneous Amebiasis: Diagnosis - Spotting the Culprit
- Primary Goal: Identify Entamoeba histolytica trophozoites.
- Key Samples: Scrapings/aspirates from ulcer edge; Biopsy from active ulcer margin.
- Microscopy:
- Wet mount (saline/iodine): Look for motile trophozoites, often with ingested RBCs (erythrophagocytosis).
- Histopathology (Biopsy):
- Key for demonstrating tissue invasion.
- Shows characteristic flask-shaped ulcers, necrosis, inflammation.
- Trophozoites found at the junction of necrotic & viable tissue; PAS stain can highlight them.
⭐ Definitive diagnosis relies on demonstrating E. histolytica trophozoites (often containing ingested RBCs) in tissue biopsy or scrapings from the ulcer edge.
- Culture:
- Specialized media (e.g., Robinson's medium). Generally low sensitivity.
- PCR (Polymerase Chain Reaction):
- Highly sensitive & specific for E. histolytica DNA.
- Differentiates pathogenic E. histolytica from non-pathogenic E. dispar.
- Serology:
- Detects anti-amebic antibodies (IgG).
- More reliable for systemic amebiasis (e.g., liver abscess); supportive in cutaneous cases.
Cutaneous Amebiasis: Management - Kicking Out Amebae
- Goal: Eradicate Entamoeba histolytica & promote healing.
- Systemic Therapy:
⭐ Systemic metronidazole (e.g., 750 mg TID for 7-10 days) is the mainstay of treatment, combined with management of any underlying intestinal or hepatic amebiasis.
- Alternatives: Tinidazole (2g OD for 3 days).
- Luminal Amebicides (Post-Systemic Therapy):
- Purpose: Eliminate intestinal carriage, prevent relapse.
- Agents: Paromomycin, iodoquinol, diloxanide furoate.
- Surgical Intervention (Adjunctive):
- Debridement: For extensive necrotic tissue.
- Drainage: For associated abscesses.
- Supportive Care:
- Wound management.
- Nutritional support.
- Pain relief.
- Prevention: Improve personal hygiene; screen & treat asymptomatic carriers/contacts.
High‑Yield Points - ⚡ Biggest Takeaways
- Caused by Entamoeba histolytica, often secondary to intestinal/hepatic amebiasis.
- Presents as painful, rapidly progressive ulcers with undermined edges and necrotic, "gun-metal gray" base.
- Flask-shaped ulcers are characteristic on biopsy.
- Common sites include perianal, genital regions, and abdominal wall (e.g., post-surgery).
- Diagnosis via trophozoites in biopsy or exudate.
- Treatment: Systemic metronidazole is key; surgical debridement may be required.
- Can lead to fistulae and secondary bacterial infections.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

