Occupational Dermatoses & Comp.: Intro - Skin at Work Comp
- Occupational Dermatoses (OD): Skin diseases primarily caused or significantly exacerbated by workplace exposures (chemical, physical, biological agents).
- Constitute a major group of occupational illnesses.
- Worker's Compensation (WC) in India:
- Regulated by Employees' Compensation Act, 1923.
- Offers financial aid & medical care for work-linked diseases/injuries.
- ODs are compensable if work causation is established.
- Schedule III of the Act details compensable diseases.
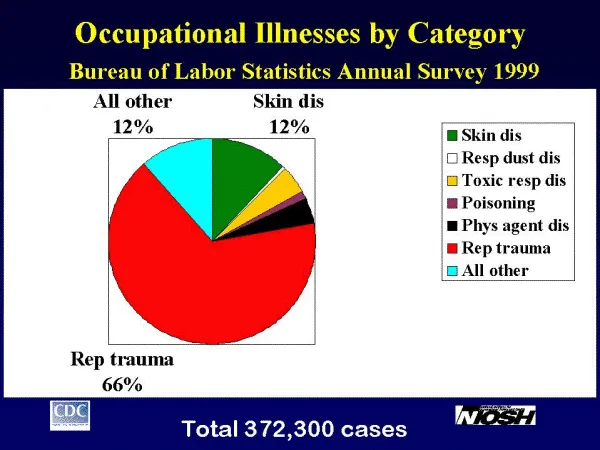
⭐ Irritant Contact Dermatitis (ICD) and Allergic Contact Dermatitis (ACD) are the most prevalent ODs, accounting for the majority of cases globally and in India.
Occupational Dermatoses & Comp.: Causation - Causation Conundrum
The "causation conundrum": definitively linking skin disease to specific work tasks/exposures. Essential for compensation. Key Criteria for Establishing Work-Relatedness (modified Mathias):
- Clinical Picture: Matches known occupational dermatoses (e.g., Irritant Contact Dermatitis (ICD), Allergic Contact Dermatitis (ACD)).
- Workplace Exposure: Confirmed contact with specific irritants or allergens.
- Anatomic Site: Consistent with occupational contact and exposure route.
- Temporal Relationship: Symptoms flare with work exposure, improve when away.
- Non-Occupational Factors: Ruled out or less significant contributors.
- Diagnostic Tests: Positive patch test for suspected Allergic Contact Dermatitis (ACD); provocation tests.
- Cessation Effect: Clear improvement upon removal from exposure.

⭐ For worker's compensation, meticulous documentation of exposure history and fulfillment of multiple causation criteria are critical for a successful claim.
Occupational Dermatoses & Comp.: Types & Agents - Rash Decisions
| Type | Common Agents | Key Industries/Tasks |
|---|---|---|
| Irritant Contact Derm. (ICD) | Soaps, detergents, acids, alkalis, solvents, wet cement | Healthcare, cleaning, construction, mechanics, hairdressing |
| Allergic Contact Derm. (ACD) | Nickel, chromates (cement), PPD (hair dyes), epoxy resins, Parthenium | Construction, hairdressing, beauty, healthcare (gloves), manufacturing |
| Occupational Acne | Mineral oils, greases, coal tar, chlorinated hydrocarbons | Mechanics, oil refinery, road workers |
| Photocontact Dermatitis | Tar, psoralens (plants), dyes, drugs (NSAIDs) | Road construction, agriculture, pharma |
| Contact Urticaria | Latex, foods, animal dander, formaldehyde, acrylics | Healthcare (gloves), food processing, animal handling |
⭐ Cement is a major cause of both ICD (due to alkalinity, hygroscopic nature) & ACD (due to dichromate content) in Indian construction workers, making patch testing crucial for differentiation and management in these cases of "cement dermatitis".
Occupational Dermatoses & Comp.: Claims Process - Paper Trail Payday
- Key Acts (India):
- Employees' State Insurance (ESI) Act, 1948
- Employee's Compensation Act, 1923 (formerly Workmen's Compensation Act)
- Claim Steps:
- Worker notifies employer of suspected Occupational Dermatosis (OD).
- Employer notifies ESI/insurer.
- Medical examination & certification (e.g., ESI Form 16 - First Certificate, Form 17 - Final Certificate).
- Claim form submission with supporting documents (medical records, employment proof).
- Adjudication by relevant authority (ESI Corp/Commissioner).
- Compensation if claim is accepted.
- 📌 Remember: Prompt reporting is key!
⭐ Medical board assessment is often required for determining the extent of permanent disablement and corresponding benefits under ESI Act.
High-Yield Points - ⚡ Biggest Takeaways
- Causality establishment is paramount for worker's compensation in occupational dermatoses.
- Patch testing is key for identifying allergens in Allergic Contact Dermatitis (ACD).
- Compensation depends on temporary or permanent disability and loss of earning capacity.
- Timely reporting to relevant authorities (e.g., ESIC in India) is mandatory.
- Aggravation of pre-existing dermatoses by occupational exposure can be compensable.
- Preventive measures and their adherence can impact claim outcomes.
- Comprehensive medical records and expert opinion are vital evidence for claims.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

