Introduction & Classification - Workplace Skin Woes
Occupational physical injuries: Skin damage or alterations resulting from direct exposure to physical agents or forces within the workplace environment. Classified by causative agent:
| Injury Type | Examples & Mechanism | High-Risk Occupations |
|---|---|---|
| Mechanical | Friction (blisters), pressure (calluses), cuts, vibration | Construction, agriculture, manufacturing |
| Thermal | Heat (burns), cold (frostbite) | Chefs, welders, firefighters, cold storage |
| Radiation | UV (sunburn), Ionizing (radiodermatitis) | Outdoor workers, healthcare, nuclear industry |
| Electrical | Burns, tissue necrosis | Electricians, power line workers |
Mechanical Trauma - Friction & Force Fiesta
- Direct Force Injuries:
- Abrasions: Superficial epidermal damage; e.g., construction falls.
- Lacerations: Irregular skin tears; e.g., butcher's knife cuts.
- Punctures: Deep, narrow wounds; e.g., healthcare needlesticks.
⭐ Puncture wounds from contaminated objects (e.g., agricultural tools, waste disposal) pose significant tetanus and deep infection risk.
- Friction & Pressure Injuries:
- Friction Blisters: Epidermal fluid separation from rubbing; common in manual labor.
- Calluses (Tyloma): Diffuse protective hyperkeratosis from chronic friction/pressure. E.g., carpenter hands.
- Corns (Clavus): Painful, localized hyperkeratotic cones on bony points. E.g., workers' ill-fitting shoes.
- Pressure Ulcers: Ischemic necrosis from sustained pressure. 📌 Stages (RBCD):
- Stage 1: Redness (non-blanchable erythema).
- Stage 2: Blister/Break (partial-thickness).
- Stage 3: Crater (full-thickness skin loss, fat visible).
- Stage 4: Deep damage (full-thickness tissue loss, muscle/bone exposed).
Thermal Trauma - Sizzle & Shiver Saga
Heat Burns:
- Types: Thermal, Chemical, Electrical.
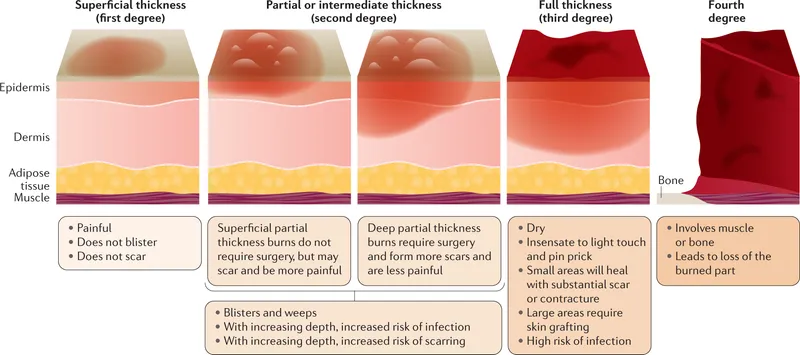
- Depth Classification:
- 1st Degree (Superficial): Epidermis. Red, painful. Heals 3-6 days.
- 2nd Degree (Partial Thickness): Dermis. Blisters.
- Superficial: Painful. Heals 7-21 days.
- Deep: ↓Pain, mottled. Scarring. Heals >21 days.
- 3rd Degree (Full Thickness): Subcutaneous. Leathery, insensate. Grafting.
- 📌 Rule of Nines (BSA estimation).
Cold Injuries:
- Frostnip: Superficial, reversible numbness, pallor. No tissue loss.
- Frostbite: Tissue freezing. Degrees vary: depth, blistering (clear→hemorrhagic), necrosis.
- Raynaud's Phenomenon: Episodic vasospasm (digits). Triggers: cold, vibration tools.
Initial Workplace Burn Management: Stop burn (cool water 10-20 min for thermal, not ice; irrigate chemical), ABCs, remove constrictions, clean dry dressing, medical aid.
⭐ Electrical burns: "Iceberg effect" - deep damage exceeds surface injury. Current prefers nerves/vessels.
Radiation & Other Agents - Invisible Impactors
- Non-Ionizing Radiation:
- UV Radiation (UVR):
- Sources: Solar exposure, welding arcs, lasers.
- Skin Effects: Sunburn (erythema), photoaging (wrinkles, lentigines), photocarcinogenesis (BCC, SCC, melanoma).
⭐ Welder's flash (arc eye/photokeratitis) is a common UV radiation injury to eyes; skin burns also occur.
- Infrared Radiation (IR):
- Sources: Furnaces, molten glass/metal, heat lamps.
- Skin Effects: Erythema ab igne (reticulated hyperpigmentation), thermal burns, accelerates photoaging.
- UV Radiation (UVR):
- Ionizing Radiation (X-rays, Gamma rays):
- Acute Radiodermatitis: Dose-dependent. Erythema (threshold ~2-5 Gy), epilation (~3 Gy), dry/moist desquamation (>10-12 Gy), necrosis (>20 Gy).
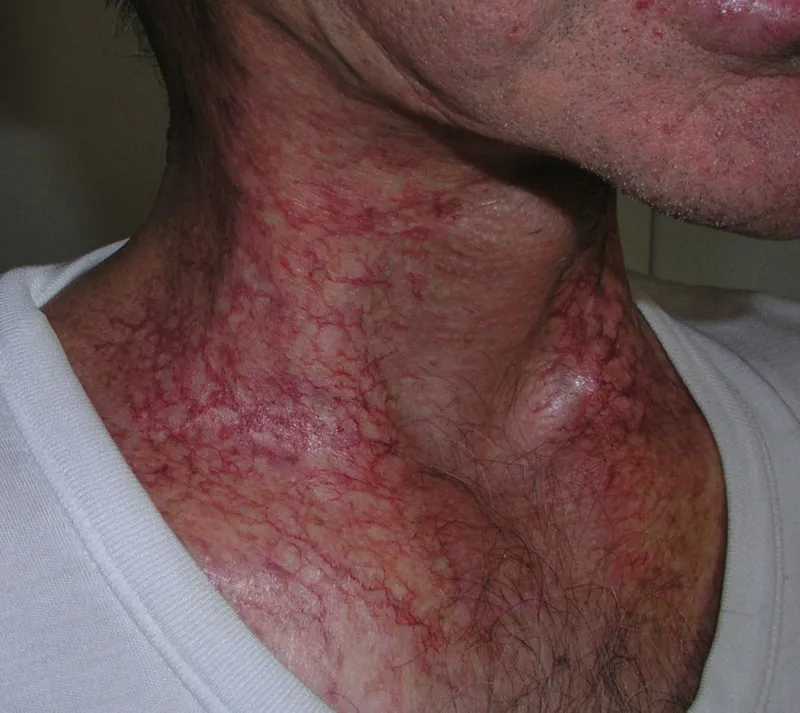
- Chronic Radiodermatitis: Develops months/years later. Atrophy, telangiectasias, hyper/hypopigmentation, fibrosis, chronic ulceration, ↑ risk of SCC.
- Vibration:
- Hand-Arm Vibration Syndrome (HAVS): From vibrating tools. Skin signs: Vibration white finger (Raynaud's phenomenon), numbness, tingling.
High-Yield Points - ⚡ Biggest Takeaways
- Friction & Pressure: Cause callosities, blisters, and pressure ulcers (decubitus).
- Vibration (HAVS): Leads to Raynaud's phenomenon, digital blanching, and neuropathy.
- Thermal Injuries: Include burns (heat, chemical, electrical) and heat rash (miliaria).
- Cold Exposure: Results in frostbite (tissue freezing) and chilblains (pernio).
- UV Radiation (Solar): Key risk for sunburn, actinic keratosis, and skin malignancies.
- Ionizing Radiation: Can cause acute, chronic, or recall radiation dermatitis.
- Physical Trauma: Cuts/abrasions may lead to keloids, hypertrophic scars, and infections.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

