Introduction & Causative Agents - Skin's Chemical Foes
Chemical burns are tissue injuries from corrosive agents, prevalent in Indian industries like construction (cement), agriculture (fertilizers), textiles, and cleaning.
- Common Causative Agents:
- Acids: e.g., $H_2SO_4$ (batteries, fertilizers), $HCl$ (metal cleaning). Cause coagulation necrosis.
- Alkalis: e.g., $NaOH$ (soaps, drain cleaners), $Ca(OH)_2$ (cement, lime). Cause liquefactive necrosis.
- Organic Solvents: e.g., Phenol (disinfectants), petroleum products (degreasers).
- Oxidizers: e.g., Bleaches ($NaOCl$), $KMnO_4$.
- Reducing Agents: e.g., Chromates.
⭐ Alkalis (like cement, drain cleaners) generally cause deeper and more severe burns than acids due to liquefactive necrosis, allowing progressive penetration.
Pathophysiology - How Chemicals Scorch
Chemicals inflict damage via distinct mechanisms:
| Agent Type | Necrosis Type | Key Mechanism & Penetration |
|---|---|---|
| Acids | Coagulative | Protein denaturation forms a firm eschar, limiting deeper penetration. (e.g., $H_2SO_4$, $HCl$) |
| Alkalis | Liquefactive | Saponification of fats (Fat + Alkali $\rightarrow$ Soap + Glycerol), cell lysis; deep, ongoing destruction. (e.g., $NaOH$, $KOH$) 📌 Alkali eats All the way through. |
⭐ Hydrofluoric acid (HF) uniquely causes liquefactive necrosis and binds $Ca^{2+}$ and $Mg^{2+}$, leading to severe pain, bone decalcification, and systemic hypocalcemia/hypomagnesemia.
- Other Notable Agents:
- White Phosphorus: Combined thermal & chemical injury; ignites with air.
- Phenols (Carbolic Acid): Coagulative necrosis; potent systemic absorption (CNS, cardiac toxicity).
Clinical Presentation & Diagnosis - Burn Clues & Grades
- General Signs: Pain, erythema, blistering, necrosis.
- Specific Clues (Agent-Dependent):
- Acids (Coagulative Necrosis):
- Sulphuric ($H_2SO_4$): Black/brown eschar.
- Nitric ($HNO_3$): Yellow eschar.
- Hydrofluoric (HF): Intense pain (often delayed, out of proportion to visible injury), erythema, blistering; risk of systemic hypocalcemia.
- Phenol (Carbolic Acid): White, then brown eschar; initially painless (local anaesthetic effect).
- Alkalis (Liquefactive Necrosis): Soapy feel, deep penetration, often more severe than acid burns.
- Acids (Coagulative Necrosis):
- Burn Depth & TBSA:
- Classification:
- Superficial (Epidermal): Erythema, pain, no blisters.
- Partial-thickness (Dermal): Blisters. Superficial dermal is painful, moist, red, blanches. Deep dermal is less painful, mottled white/pink, may not blanch.
- Full-thickness: Leathery, dry, insensate; white, charred, or brown.
- TBSA Estimation (Adult Rule of Nines): Head & Neck 9%, Each Upper Limb 9%, Each Lower Limb 18%, Anterior Trunk 18%, Posterior Trunk 18%, Perineum 1%.
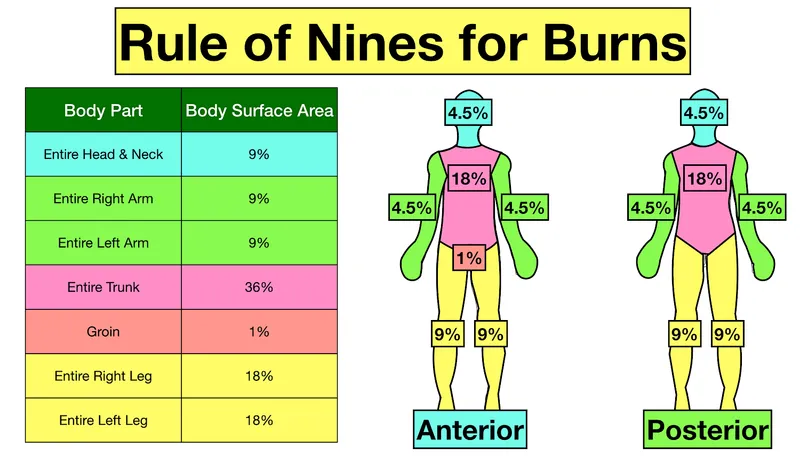
- Classification:
- Diagnosis:
- History: Identify agent, concentration, volume, duration of contact, irrigation performed.
- Physical Examination: Assess burn depth, TBSA, signs of systemic toxicity.
- pH testing (skin/eye): Crucial for unknown agents or alkalis. Irrigate until pH 7.0-7.4.
⭐ Chromic acid burns can cause delayed renal and hepatic failure due to systemic absorption of hexavalent chromium.
Management & Prevention - Dousing the Damage
- Immediate First Aid (ABCDE):
- Remove contaminated clothing/jewelry.
- Copious irrigation (water/saline) for at least 30-60 minutes.
- 📌 DRIP: Decontaminate, Irrigate, Protect, Pain relief.

- Specific Antidotes:
- Hydrofluoric (HF) Acid: Calcium gluconate.
- Phenol: Polyethylene glycol (PEG) / Isopropyl alcohol.
- White Phosphorus: Copper sulfate (1% solution, cautious use, remove particles).
- General Burn Care: Analgesia, non-adherent dressings, tetanus prophylaxis, topical antimicrobials.
- Referral to Burn Unit: Burns >10% TBSA (adults), >5% (children); Full-thickness >2%; Face, hands, feet, genitalia, major joints.
- Prevention: PPE (gloves, goggles), safety protocols, emergency eyewash/shower stations.
⭐ Copious water irrigation is the cornerstone of immediate management for most chemical burns; neutralization attempts without prior copious irrigation can sometimes worsen injury by generating heat.
High‑Yield Points - ⚡ Biggest Takeaways
Error: Failed to generate content for this concept group.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

