Introduction & Epidemiology - Skin's Workplace War
- Occupational Allergic Contact Dermatitis (OACD): Type IV hypersensitivity reaction to workplace allergens.
- A major occupational illness, causing significant morbidity and economic burden, particularly in developing nations like India.
- Accounts for ~20-25% of all occupational skin diseases.
- Impacts quality of life, leading to absenteeism and potential job changes.
- Common in: Construction, healthcare, agriculture, hairdressing, metal industries.
⭐ Cement (chromium) is a primary cause of OACD in Indian construction workers, especially due to potassium dichromate content in cement.
Pathophysiology - Allergy's Sneaky Setup
- Mechanism: Type IV (delayed) hypersensitivity, with two distinct phases.
- Sensitization Phase (Initial contact; 10-14 days):
- Haptens (e.g., nickel, PPD) penetrate epidermis.
- Combine with skin proteins → complete antigen.
- Langerhans cells (APCs) present to naive T-cells → memory T-cells formed.
- No dermatitis at this stage.
- Elicitation Phase (Re-exposure; 12-72 hours):
- Allergen re-encounters activate memory T-cells.
- Rapid cytokine release (e.g., $IFN-\gamma$, $TNF-\alpha$).
- Results in eczematous inflammation.
- Sensitization Phase (Initial contact; 10-14 days):
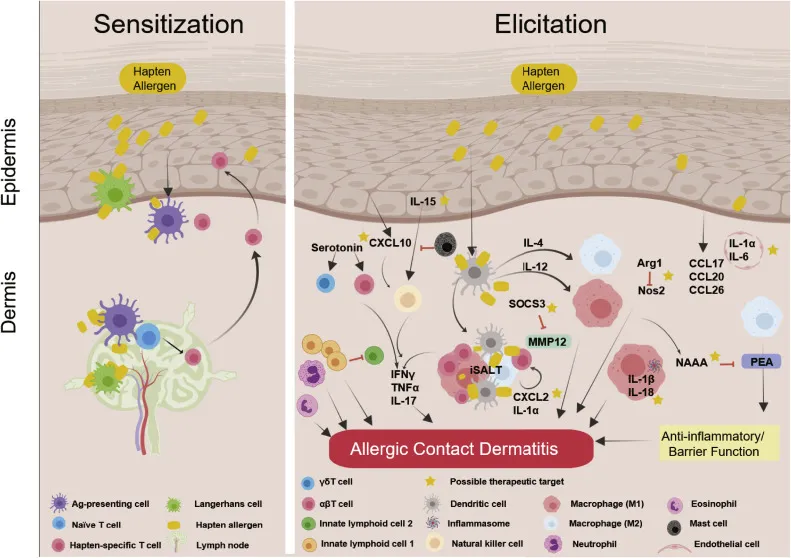
⭐ Langerhans cells (epidermal APCs) are pivotal: they capture haptens, migrate to lymph nodes, and prime naive T-cells, initiating sensitization.
Common Workplace Allergens (India Focus) - India's Itch Triggers
| Allergen | Common Sources (India Focus) | At-Risk Occupations (India) |
|---|---|---|
| Cement (Chromates) | Construction materials, wet cement | Construction workers, masons |
| Parthenium hysterophorus | "Congress Grass" weed 📌 | Farmers, gardeners, field workers |
| PPD (Paraphenylenediamine) | Hair dyes, "black henna", textile dyes | Hairdressers, beauticians, dyers |
| Nickel | Jewellery, coins, buckles, metal tools | Jewellery/metal workers, cashiers |
| Potassium Dichromate | Leather tanning, paints, matches, cement | Tanners, painters, construction |
| Epoxy Resins | Adhesives, paints, plastics, electronics | Painters, construction, electronics |
| Rubber Accelerators (Thiurams, Carbamates) | Gloves, footwear, tyres | Healthcare, industrial, sanitation |
⭐ Cement is the most common occupational allergen in India, primarily due to chromate sensitivity. Parthenium is the leading plant sensitizer.
Clinical Features & Diagnosis - Spotting The Reaction
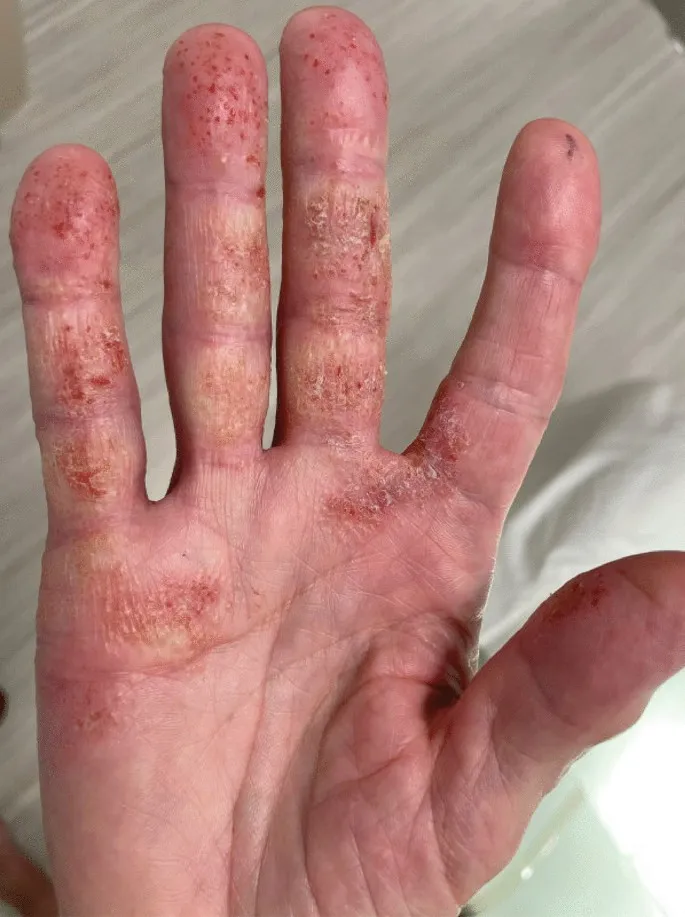
- Morphology:
- Acute: Erythema, edema, papules, vesicles, bullae; intense pruritus.
- Chronic: Scaling, lichenification, fissures.
- Distribution:
- Matches allergen contact area; often well-demarcated.
- Common: Hands, wrists, forearms, face, eyelids.
- Diagnosis:
- Detailed history (occupational exposure).
- Patch Test: Gold standard.
- Allergens applied for 48 hrs.
- Readings at 48 hrs & 72-96 hrs (or later for some allergens like PPD, neomycin).
- Indian Standard Battery (ISB) commonly used.
⭐ Patch testing is the gold standard for diagnosing ACD; positive reactions must correlate clinically with exposure for definitive diagnosis.
Management & Prevention - Worker Skin Shield
-
Management:
- Identify & avoid/substitute allergen (via patch test).
- TCS for flares; TCIs for sensitive areas.
- Systemic steroids (Prednisolone 0.5-1 mg/kg) if severe.
- Antihistamines for itch.
-
Prevention (📌 SKIN):
- Substitute allergens (e.g., ferrous sulfate in cement for $Cr^{6+}$).
- Keep skin clean; use emollients.
- Inform & educate workers (hazards).
- No touch techniques; PPE (gloves, aprons).
-
Barrier Creams: Adjunct to PPE, not replacement.
⭐ Cement is a leading cause of occupational ACD, often from chromium & cobalt sensitizers.
- Legislation: Key acts: Factories Act, Employee's Compensation Act.
High‑Yield Points - ⚡ Biggest Takeaways
- Type IV hypersensitivity; delayed onset (24-72 hours).
- Workplace allergens: Nickel, Potassium dichromate (cement), PPD (dyes), Epoxy resins, Rubber chemicals.
- Patch testing is gold standard for identifying specific allergen.
- Features: Intensely pruritic, eczematous lesions (erythema, vesicles) with sharp demarcation.
- Distribution (hands, face) often clues occupational source; improves away from work.
- Management: Strict allergen avoidance is key; topical corticosteroids for flares.
- Chronic exposure leads to lichenification and fissuring.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

