Scarring Alopecias - Follicle Fallout
- Irreversible hair loss due to destruction of hair follicle stem cells & replacement by fibrous tissue.
- Also known as cicatricial alopecias.
- Classification based on predominant inflammatory infiltrate:
- Lymphocytic
- Lichen Planopilaris (LPP)
- Frontal Fibrosing Alopecia (FFA)
- Chronic Cutaneous Lupus Erythematosus (CCLE) / Discoid Lupus Erythematosus (DLE)
- Central Centrifugal Cicatricial Alopecia (CCCA)
- Neutrophilic
- Folliculitis Decalvans
- Dissecting Cellulitis (Perifolliculitis Capitis Abscedens et Suffodiens)
- Mixed
- Acne Keloidalis Nuchae
- Lymphocytic
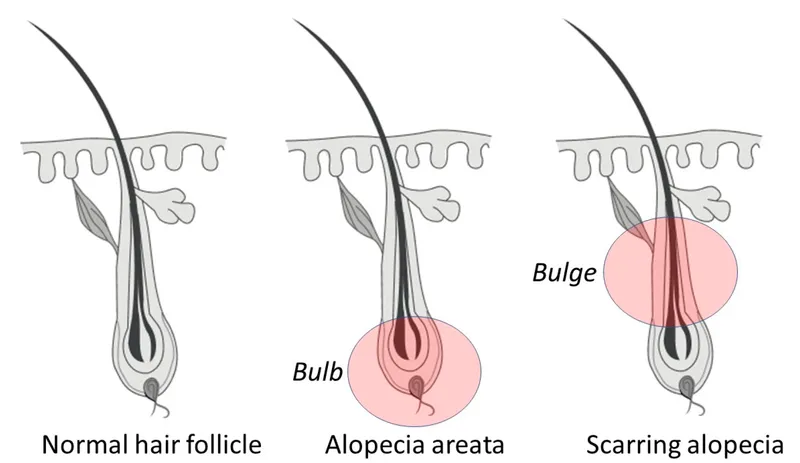
⭐ Scarring alopecias involve destruction of hair follicle stem cells, leading to irreversible hair loss and permanent scarring of the affected scalp areas, distinguishing them from non-scarring forms where the follicle remains intact and regrowth is possible.
Lymphocytic Types - Immune Invasion

- Mechanism: Lymphocytic inflammation targets hair follicles, leading to permanent destruction and scarring.
- Key Types Compared:
| Feature | Lichen Planopilaris (LPP) | Frontal Fibrosing Alopecia (FFA) | Discoid Lupus Erythematosus (DLE) - Scalp |
|---|---|---|---|
| Target | Middle-aged women | Postmenopausal women | Women > Men (20-40 yrs) |
| Clinical | Perifollicular erythema/scaling, pruritus; patchy loss. | Symmetric frontotemporal recession, eyebrow loss. | Erythematous plaques, adherent scale, follicular plugs, atrophy. |
| Sites | Vertex, parietal scalp. | Frontal hairline, eyebrows. | Sun-exposed scalp, ears. |
| Histo | Lymphocytic infiltrate (bulge), perifollicular fibrosis. | LPP-like, often paucicellular. | Interface dermatitis, follicular plugging, ↑mucin. |
| Assoc. | Oral/cutaneous LP. | Often none. | SLE (~5-10%). |
| ⭐ Highlight | > Perifollicular erythema & scaling. | > "Lonely hair" sign; band-like recession. | > "Carpet tack" sign; dyspigmentation. |
Neutrophilic & Mixed Types - Pustule Problems
- Primarily neutrophilic (Folliculitis Decalvans, Dissecting Cellulitis) or mixed (CCCA with pustules).
- Features: Follicular pustules, inflammation leading to irreversible follicle destruction and scarring alopecia.
- Symptoms: Pain, pruritus, tenderness, purulent discharge are common.
| Feature | Folliculitis Decalvans (FD) | Dissecting Cellulitis (DSC/PCAS) | Central Centrifugal Cicatricial Alopecia (CCCA) |
|---|---|---|---|
| Key Clinical | Chronic pustules, erosions, crusts; Tufted hairs | Painful, boggy nodules; Interconnecting sinus tracts; Discharge | Progressive central scarring; Pruritus, breakage; ±Pustules |
| Primary Cells | Neutrophils (dominant) | Neutrophils (early), then Mixed inflammation | Lymphocytes (predominant); Neutrophils if 2° infection |
| Common Site | Vertex, occiput | Vertex, occiput; can be diffuse | Crown, vertex; spreads centrifugally |
| Assoc. (📌) | - | 📌 Follicular Occlusion Tetrad (acne conglobata, HS) | Common in women of African descent; Familial link |
| Rx Highlights | Systemic antibiotics (Clinda+Rifa), Oral Isotretinoin | Oral Isotretinoin (1st line), Antibiotics, TNF-α inhibitors | Potent topical/IL steroids, Tetracyclines (anti-inflam.) |
⭐ Tufted hairs (multiple hairs from one follicle) are characteristic of Folliculitis Decalvans.
Diagnosis & Management - Scalp Savers
- Diagnosis:
- History (itch, pain), exam (erythema, scaling, ↓follicular openings).
- Trichoscopy: Essential. Shows perifollicular scaling/erythema, absent ostia, tufting.

- Scalp Biopsy: Gold standard. 4mm punch from active edge; horizontal & vertical sections.
⭐ Scalp biopsy with both horizontal and vertical sections is crucial for accurate diagnosis of scarring alopecias.
- Management:
- Goal: Arrest progression, control inflammation, relieve symptoms.
- Early, aggressive therapy vital.
- Medical: Potent topical/intralesional corticosteroids. Systemic: Hydroxychloroquine, methotrexate, cyclosporine. Antibiotics for neutrophilic types.
- Surgical: Hair transplant if stable for >1-2 years.
- Diagnostic Algorithm:
High‑Yield Points - ⚡ Biggest Takeaways
- Scarring alopecias cause irreversible hair loss due to follicular destruction and fibrosis.
- Lichen Planopilaris (LPP) presents with perifollicular erythema and scaling; Frontal Fibrosing Alopecia (FFA) is a key variant.
- Discoid Lupus Erythematosus (DLE) on the scalp shows erythematous plaques, follicular plugging, and atrophic scarring.
- Central Centrifugal Cicatricial Alopecia (CCCA) typically affects Black women, starting at the vertex/crown.
- Folliculitis Decalvans is characterized by chronic neutrophilic inflammation, pustules, and tufted hairs.
- Dissecting cellulitis of the scalp involves deep, interconnecting abscesses and sinus tracts.
- Scalp biopsy is crucial for diagnosis, often revealing loss of sebaceous glands and specific inflammatory patterns.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

