Mycetoma - Madura's Foot Mess
- Chronic, suppurative, granulomatous infection of subcutaneous tissue, fascia, and bone.
- Classic Triad:
- Painless subcutaneous mass (tumefaction).
- Multiple sinuses.
- Discharge containing grains (microcolonies).
- Types & Causative Agents (Grain Color):
- Eumycetoma (Fungal):
- Madurella mycetomatis (Most common in India; Black grains).
- Acremonium falciforme, Fusarium spp. (White grains).
- Actinomycetoma (Bacterial - Filamentous):
- Nocardia brasiliensis (Most common worldwide; Yellow/White grains).
- Actinomadura madurae (White/Yellow grains).
- Streptomyces somaliensis (Yellow/Brown grains).
- Eumycetoma (Fungal):
⭐ Madurella mycetomatis is the most common cause of eumycetoma in India, producing black grains, while Nocardia brasiliensis is the most common cause of actinomycetoma globally.
- 📌 Remember: Grain color is a crucial diagnostic clue!
Mycetoma - Spotting Grainy Trouble
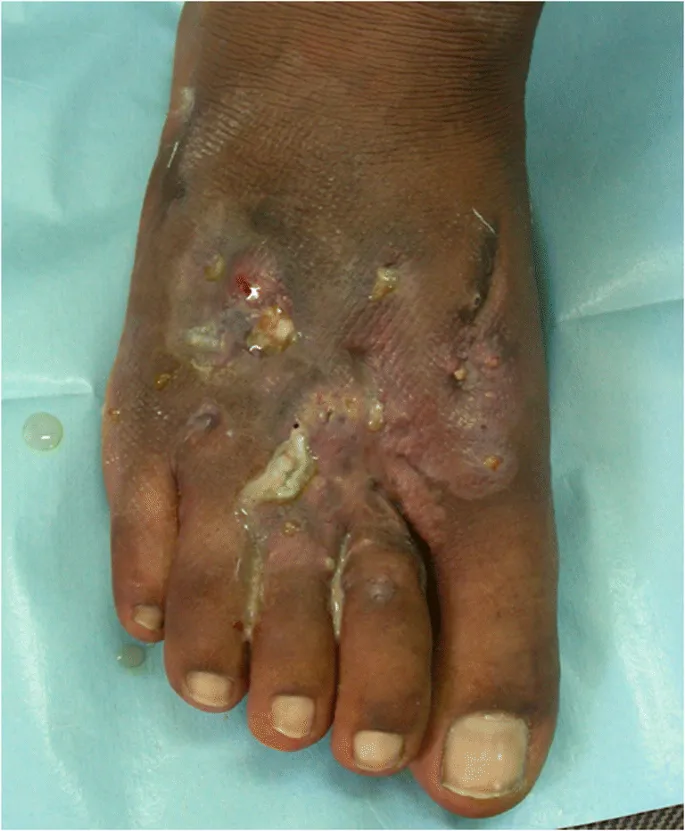
- Chronic, progressive granulomatous infection of skin, subcutaneous tissue, fascia, and bone.
- Clinical Triad:
- Painless subcutaneous mass (tumefaction)
- Multiple sinuses
- Discharge containing grains (colonies of causative agent)
- Types & Grains:
- Eumycetoma (Fungal):
- Causative agents: Madurella mycetomatis (most common, black grains), Aspergillus spp., Fusarium spp.
- Large, pigmented (black, yellow, white) grains.
- Lesions: Well-defined, hard; bone involvement late, lytic lesions.
- Actinomycetoma (Bacterial):
- Causative agents: Nocardia brasiliensis (most common), Actinomadura madurae, Streptomyces somaliensis.
- Small, fine, white, yellow, or red grains.
- Lesions: Ill-defined, soft, more inflammatory; bone involvement early, extensive, osteosclerotic with periosteal reaction.
- Eumycetoma (Fungal):
⭐ Dot-in-circle sign on MRI/USG is highly suggestive of mycetoma, representing central hypointense dot (grain) surrounded by hyperintense inflammatory granuloma.
- 📌 Mnemonic: MADura (Eumycetoma - Madurella) vs NOt MAD (Actinomycetoma - Nocardia).
Mycetoma - Nailing the Culprit

- Clinical Triad: Painless subcutaneous swelling (tumefaction), multiple discharging sinuses, visible grains/granules.
- Grains - Key to Diagnosis:
- Actinomycetoma (Bacterial): Fine (<1 mm), yellowish/whitish/reddish. Common: Nocardia spp., Actinomadura madurae.
- Eumycetoma (Fungal): Coarse (>1 mm), black/dark or white/pale. Common: Madurella mycetomatis (black), Scedosporium apiospermum (white).
- Diagnostic Toolkit:
- Microscopy: Grains (KOH, Gram stain).
- Culture: Sabouraud Dextrose Agar (SDA) for fungi; Lowenstein-Jensen (LJ) or Blood-Cysteine-Glucose Agar (BCGA) for aerobic actinomycetes.
- Histopathology: H&E, PAS, GMS.
- Imaging:
- X-ray: Bone involvement (cavities, osteolysis).
- USG/MRI: Extent, "dot-in-circle" sign (MRI).
⭐ The "dot-in-circle" sign on T2-weighted MRI is highly characteristic of mycetoma, representing a central grain surrounded by inflammatory granulation tissue.
Mycetoma - Kicking Out Invaders
- Chronic granulomatous infection: skin, subcutaneous tissue, fascia, bone.
- Triad: Painless swelling, multiple sinuses, discharge with grains (color varies).
- Types:
- Actinomycetoma (bacterial): Nocardia, Actinomadura. Grains: yellow, white, red. Responds to antibiotics.
- Eumycetoma (fungal): Madurella mycetomatis (commonest). Grains: black, dark. Antifungals + surgery.
- Diagnosis: Clinical, grain microscopy (KOH, Gram), culture, imaging (X-ray, USG, MRI).
⭐ "Dot-in-circle" sign on MRI/USG is characteristic of eumycetoma.
- 📌 Mnemonic (Actinomycetoma): "Welsh ACTINg" (Welsh regimen for ACTINomycetoma).
High‑Yield Points - ⚡ Biggest Takeaways
- Mycetoma: Chronic granulomatous infection of skin, subcutaneous tissue, and bone.
- Key triad: Painless subcutaneous mass, multiple sinuses, and discharging grains.
- Two types: Eumycetoma (fungal) and Actinomycetoma (bacterial); latter commoner in India.
- "Madura foot" is the classic presentation.
- Grains (color, consistency) are diagnostic; sulphur granules in Actinomycetoma.
- Actinomycetoma treatment: long-term antibiotics (e.g., Welsh regimen).
- Eumycetoma treatment: antifungals and often surgery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

