Introduction & Etiology - The Yeast Beast
- Causative Organisms:
- Candida albicans (most common).
- Non-albicans: C. glabrata, C. tropicalis, C. parapsilosis.
- C. krusei (fluconazole-resistant).
- Nature: Commensal; opportunistic pathogen.
- Virulence: Adherence, dimorphism (yeast→hyphae for invasion), biofilms, enzymes.
- Predisposing Factors: Diabetes, immunosuppression (HIV, steroids), antibiotics, pregnancy, OCPs, obesity, occlusion, maceration, age extremes, catheters, IV drug use.
- 📌 Mnemonic (CANDIDIASIS): Corticosteroids, Antibiotics, Nutrition-poor, Diabetes, Immunosuppression, Age extremes, Skin breakdown, IV lines/devices, Systemic illness.
⭐ Candida albicans is a dimorphic fungus, existing as yeast and hyphal forms; the hyphal form is typically associated with tissue invasion.
Clinical Spectrum - Candida's Canvas
- Mucocutaneous Candidiasis:
- Oral (Thrush): Pseudomembranous (white, scrapes off), Erythematous (red), Angular cheilitis, Median rhomboid glossitis.
- Vulvovaginal (VVC): Itching, burning, 'cottage cheese' discharge. Recurrent VVC: ≥4 episodes/year.
- Balanitis: Penile erythema, papules, pustules.
- Cutaneous Candidiasis:
- Intertrigo: Red, moist plaques in skin folds (axillae, groin). Satellite papules/pustules are key.
- Diaper Dermatitis: Beefy red plaques, satellite lesions.
- Paronychia & Onychomycosis: Nail fold inflammation, nail changes.
- Chronic Mucocutaneous Candidiasis (CMC):
- Persistent infections (skin, nails, mucous membranes).
- Associated with endocrinopathies (APECED) or immune defects (IL-17 pathway).

⭐ Satellite lesions (papules/pustules beyond the main erythematous area) are a hallmark of cutaneous candidiasis, especially intertrigo.
Diagnostic Clues - Spotting Spores
- Clinical presentation often suggestive.
- Microscopy:
- KOH Mount (10-20%): Skin/nail/discharge. Shows budding yeast cells & pseudohyphae.
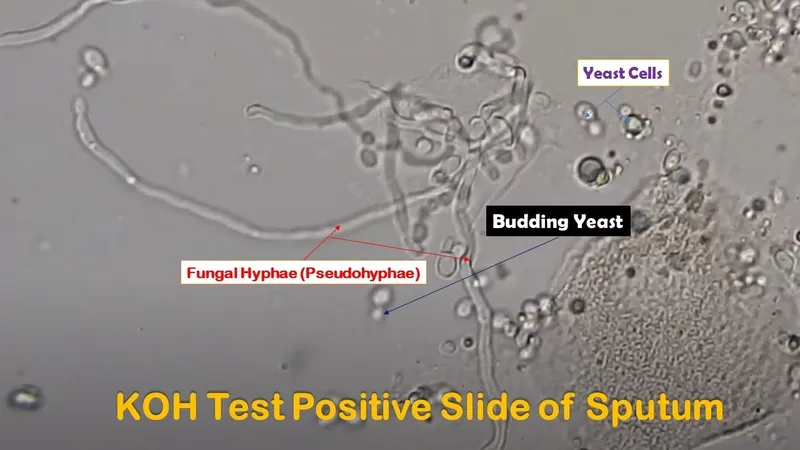
- Gram Stain: Gram-positive budding yeasts & pseudohyphae.
- KOH Mount (10-20%): Skin/nail/discharge. Shows budding yeast cells & pseudohyphae.
- Culture (not routine for uncomplicated cases; useful for recurrent/resistant infections or species ID):
- Sabouraud Dextrose Agar (SDA): Creamy, opaque colonies.
- CHROMagar Candida: Differential growth/color for species identification (e.g., C. albicans - green, C. tropicalis - blue).
- Germ Tube Test: C. albicans forms germ tubes in serum at 37°C (2-3 hrs) - presumptive identification.
- Wood's Lamp: Negative.
- Biopsy (rarely needed): May show yeasts & pseudohyphae in stratum corneum.
⭐ On KOH mount, Candida typically shows budding yeast cells and pseudohyphae, which are chains of budding yeast cells that have failed to detach.
Treatment Toolkit - Fungal Fight Plan
- General Measures: Keep areas dry, weight ↓, glycemic control (diabetics), avoid occlusive clothing.
- Topical Antifungals (Localized):
- Polyenes: Nystatin (cream, powder; oral suspension for thrush - swish & swallow/spit).
- Azoles: Clotrimazole, Miconazole, Ketoconazole, Econazole, Sertaconazole.
- Ciclopirox olamine.
- Duration: 1-4 weeks; continue 1 week post-resolution.
- Systemic Antifungals (Extensive/Recurrent/Nail/Immunocompromised):
- Azoles: Fluconazole (DOC; VVC: 150 mg single dose; Oropharyngeal: 100-200 mg/day for 7-14 days), Itraconazole.
- Echinocandins (IV, severe/invasive): Caspofungin, Micafungin.
- 📌 Mnemonic (Fluconazole resistant): "Krusei and Glabrata Hate Fluconazole" (C. krusei, C. glabrata).
⭐ Fluconazole 150 mg single oral dose is a highly effective and convenient treatment for uncomplicated vulvovaginal candidiasis.
High‑Yield Points - ⚡ Biggest Takeaways
- Causative Agent: Candida albicans (commonest), a dimorphic fungus.
- Hallmark Lesion: Beefy red plaques with satellite lesions (papules/pustules) in intertriginous areas.
- Oral Thrush: White, curd-like plaques on mucosa, easily scraped off, leaving red base.
- Vulvovaginal: Thick, "cottage cheese" discharge; intense pruritus and erythema.
- Diagnosis: KOH mount shows pseudohyphae and budding yeast cells.
- Risk Factors: Diabetes, immunosuppression (HIV, steroids), antibiotics, pregnancy, obesity.
- Treatment: Topical azoles (e.g., clotrimazole) or nystatin; oral fluconazole for severe/recurrent cases.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

