Skin Biopsy: Fundamentals - Skin Sleuthing Starts
- Purpose: Crucial diagnostic tool for skin lesions; aids in definitive diagnosis and guiding treatment. Sometimes therapeutic.
- Core Principle: Obtain adequate, representative tissue from the most active part of a lesion. Include normal skin for comparison if needed.
- Key Steps:
- Patient counselling & informed consent.
- Local anaesthesia (e.g., 1-2% lignocaine; adrenaline for vasoconstriction).
- Aseptic site preparation.
⭐ Always send biopsy in 10% buffered formalin; for immunofluorescence (IMF), use Michel's medium or normal saline.

Skin Biopsy: Types & Selection - Choosing Your Weapon
-
Goal: Obtain diagnostic tissue with minimal scarring and optimal cosmetic outcome.
-
Types & Key Uses:
- Shave: Superficial (epidermis/upper dermis). E.g., Seborrheic keratosis, warts, superficial BCC. Avoid for most melanoma. Uses No. 15 blade.
- Punch: Full-thickness sample (epidermis to subcutis). Sizes 2-8 mm (common 3-4 mm). For inflammatory dermatoses, small tumors, alopecia. Suture if >4 mm.
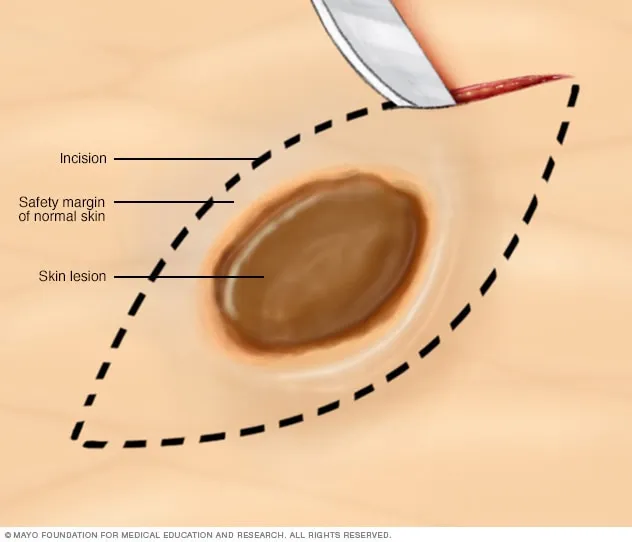
- Incisional: Partial removal of a larger lesion or deep process. Primarily diagnostic. E.g., Large tumors, panniculitis, some bullous disorders.
- Excisional: Complete removal of lesion with a margin. Diagnostic & therapeutic. E.g., Melanoma, SCC, BCC, atypical nevi. Length:width 3:1 for closure.
-
Selection Flowchart:

⭐ For suspected melanoma, excisional biopsy with 1-3 mm clinical margins is the gold standard if feasible. Punch biopsy is generally discouraged if it might transect the lesion base, potentially affecting staging.
- 📌 Mnemonic (Punch Suturing): "Punch 4 More, Suture Galore!" (punches >4mm often benefit from suturing for better healing).
Skin Biopsy: Procedure Essentials - The How-To Handbook
- Pre-Procedure:
- Informed consent.
- Site selection: Representative lesion; consider Langer's lines for cosmesis.
- Anesthesia: Lignocaine 1-2% (± adrenaline). 📌 Max dose: 4.5 mg/kg (plain), 7 mg/kg (with adrenaline).
- Procedure Steps:
- Aseptic skin preparation.
- Incision: Perpendicular to skin, ensuring adequate depth.
- Specimen handling: Gentle, avoid crush artifact; orient with suture if needed.
- Hemostasis: Pressure, electrocautery, or suture.
- Closure: Sutures or adhesive strips, appropriate to defect.
- Post-Procedure:
- Fixation: 10% neutral buffered formalin (NBF); formalin:tissue volume ~20:1.
- Dressing applied; provide clear wound care instructions.
⭐ For suspected immunobullous disorders, send specimen in Michel's medium or normal saline for direct immunofluorescence (DIF).
Skin Biopsy: Post-Op & Specimen - Seal, Send, Solve
- Post-Operative Care:
- Apply sterile, non-adherent dressing. Keep wound dry for 24-48h.
- Suture removal: Face 3-5 days; Trunk/Extremities 7-14 days.
- Analgesia (e.g., Paracetamol). Advise on infection signs (erythema, discharge).
- Specimen Management: 📌 Seal, Send, Solve
- Fixation: 10% buffered formalin (standard, prevents autolysis). Volume: 10-20x specimen.
- Special media:
- Immunofluorescence (DIF): Michel's medium / Zeus fixative (NOT formalin).
- Microbiology (culture): Saline / transport medium.
- Electron Microscopy: Glutaraldehyde.
- Crucial: Accurate labelling, detailed clinical info on requisition form.
- Prompt dispatch to lab.
⭐ For suspected immunobullous disorders (e.g., pemphigus), biopsy perilesional (normal-appearing skin adjacent to blister) for Direct Immunofluorescence (DIF).
High‑Yield Points - ⚡ Biggest Takeaways
- Shave biopsy: for superficial lesions (e.g., warts, SKs); avoid for suspected melanoma.
- Punch biopsy: provides a full-thickness sample, ideal for inflammatory dermatoses and small tumors (e.g., 3-4 mm punch).
- Excisional biopsy: removes the entire lesion with a margin; it's both diagnostic and therapeutic, especially for melanoma.
- Incisional biopsy: takes a portion of a large lesion for diagnosis when complete removal is difficult.
- Optimal biopsy site: active edge for rashes, thickest portion for suspected malignancies.
- Standard fixative for skin biopsies is 10% neutral buffered formalin.
- Anesthesia: Lignocaine 1-2% is commonly used, often with adrenaline for hemostasis and prolonged effect.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

