Mohs Micrographic Surgery - Precision Skin Saver
- Microscopically controlled excision for skin cancers, ensuring complete margin analysis.
- Goal: Highest cure rates (e.g., ~99% for primary BCCs), maximal tissue preservation.
- Key Indications:
- High-risk Basal Cell Carcinoma (BCC), Squamous Cell Carcinoma (SCC).
- Critical anatomical sites (H-zone of face, hands, feet, genitals).
- Recurrent tumors or aggressive histologic subtypes.
- Tumors with poorly defined clinical borders.
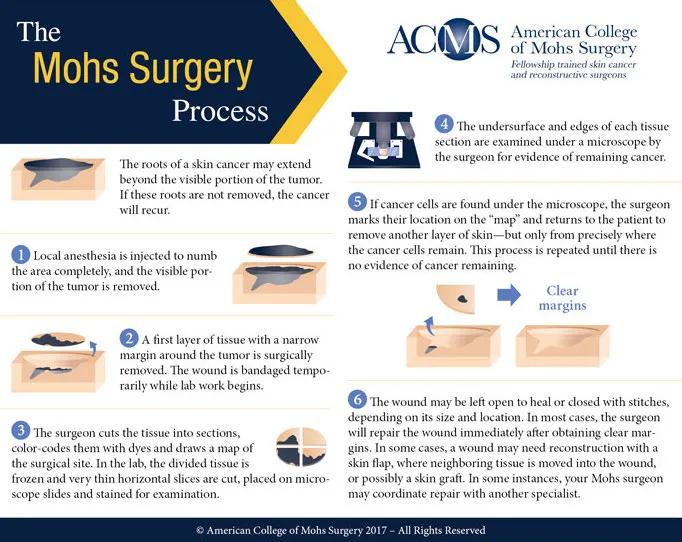
- Procedure:
- Tumor debulked, then thin layer of tissue excised.
- Tissue mapped, color-coded, and processed for frozen section histology.
- Microscopic examination of 100% of peripheral and deep surgical margins.
- If residual tumor found, further tissue excised only from positive areas.
- Advantages: Highest cure rate, maximum conservation of healthy tissue, best cosmetic outcome.
⭐ Mohs surgery is the treatment of choice for dermatofibrosarcoma protuberans (DFSP) and offers the highest cure rate for high-risk BCCs and SCCs, especially on the head and neck.
Mohs Micrographic Surgery - The 'Yes' List
- Goal: Highest cure rate (~99% for primary BCC), maximal tissue sparing.
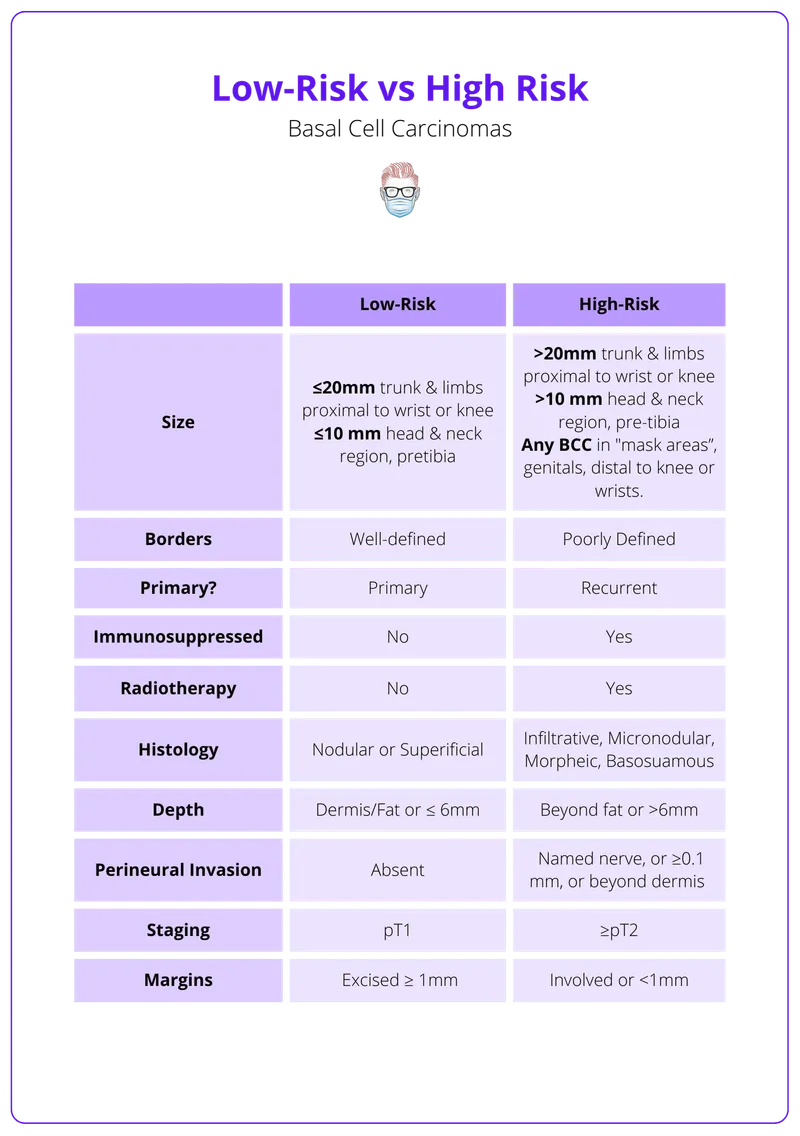
- High-Risk Non-Melanoma Skin Cancers (NMSC):
- Location (H-Zone): Central face, eyelids, nose, lips, ears, periorbital.
- Location (Other critical sites): Genitalia, hands, feet, nails.
- Size: >2cm (trunk/extremities), >1cm (cheeks/forehead/scalp/neck), >0.6cm (H-zone).
- Histology (Aggressive): Morpheaform, infiltrative, micronodular BCC; poorly differentiated SCC.
- Clinical Features: Recurrent tumors, ill-defined borders, perineural invasion (PNI).
- Patient Factor: Immunosuppressed individuals.
- Other Indicated Tumors:
- Dermatofibrosarcoma protuberans (DFSP).
- Microcystic adnexal carcinoma.
- Sebaceous carcinoma.
- Extramammary Paget's disease.
- Merkel cell carcinoma (select cases).
- Atypical fibroxanthoma.
⭐ Mohs is the gold standard for recurrent basal cell carcinoma, offering the highest cure rates and maximal tissue preservation.
Mohs Micrographic Surgery - Step-by-Step Slice
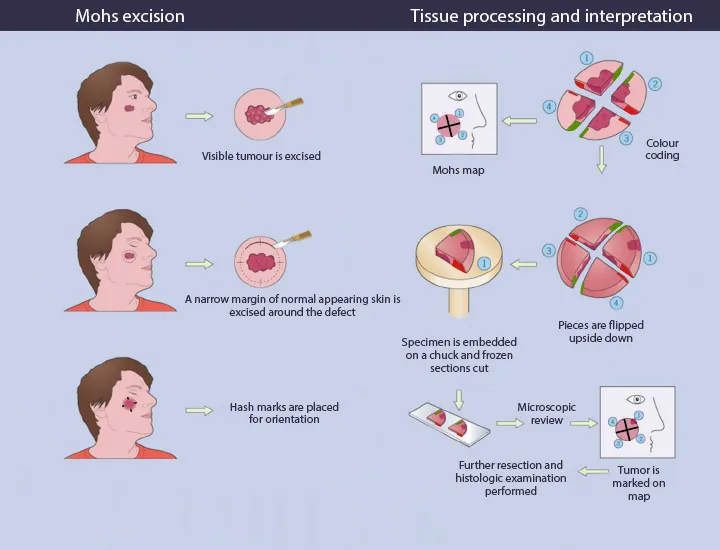
- 1. Excision & Mapping:
- Surgical removal of visible tumor plus a thin, saucerized tissue layer.
- Specimen carefully oriented, edges inked for identification, Mohs map drawn.
- 2. Tissue Processing (Frozen):
- Layer divided, meticulously frozen horizontally for 100% margin assessment.
- Slides prepared and stained (e.g., H&E).
- 3. Microscopic Review:
- Surgeon (as pathologist) examines entire margin on slides.
- Any remaining tumor precisely located on the map.
- 4. Iterative Excision (Staged):
- If tumor present, re-excise ONLY mapped positive areas.
- Repeat processing & review (stages) until margins are completely clear.
- 5. Reconstruction:
- Surgical defect repaired after confirmed tumor eradication.
⭐ Mohs examines 100% of surgical margins (peripheral & deep), unlike traditional methods (<2% sampling), maximizing cure and tissue sparing.
Mohs Micrographic Surgery - Merits & Minuses
-
Merits (Advantages)
- Highest cure rates (esp. Basal Cell Carcinoma - BCC, Squamous Cell Carcinoma - SCC)
⭐ Offers ~99% cure rate for primary BCC & ~95% for recurrent BCC.
- Maximal tissue sparing, superior cosmesis
- Complete peripheral & deep margin assessment (100%)
- Indicated for:
- High-risk tumors (e.g., aggressive, large, ill-defined borders)
- Critical anatomical sites (e.g., face, hands, feet, genitals)
- Recurrent tumors
- Tumors in immunosuppressed patients
- Highest cure rates (esp. Basal Cell Carcinoma - BCC, Squamous Cell Carcinoma - SCC)
-
Minuses (Disadvantages)
- Time-intensive procedure (multiple stages)
- Higher upfront cost
- Requires specialized team (surgeon, pathologist, technician) & lab
- Limited availability geographically
- Less suitable for certain melanomas or very bulky tumors
High‑Yield Points - ⚡ Biggest Takeaways
- Gold standard for high-risk Basal Cell Carcinoma (BCC) and Squamous Cell Carcinoma (SCC), especially in cosmetically sensitive areas (e.g., H-zone of face).
- Offers the highest cure rates (up to 99%) and maximal tissue conservation by sparing healthy tissue.
- Involves staged excisions with 100% microscopic margin control using horizontal frozen sections (en face technique).
- Key indications: recurrent tumors, aggressive histological subtypes (e.g., morpheaform, infiltrative), large size, ill-defined borders, and immunocompromised patients.
- Ensures complete tumor eradication before wound reconstruction, thereby minimizing recurrence risk significantly.
- Particularly valuable for tumors in areas where tissue preservation is paramount, like eyelids, nose, lips, and ears.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

