Excisional Surgery - Cut & Close Basics
- Definition: Surgical procedure involving full-thickness removal of a skin lesion, extending into the subcutaneous fat layer.
- Purpose:
- Diagnostic: To obtain tissue for accurate histopathological examination and diagnosis.
- Therapeutic: For complete removal of various benign or malignant skin lesions.
- Common Indications:
- Malignant lesions: Basal Cell Carcinoma (BCC), Squamous Cell Carcinoma (SCC), Melanoma.
- Benign lesions: Epidermal cysts, Lipomas, symptomatic Nevi.
⭐ For suspected melanoma, excisional biopsy with narrow margins (typically 1-3mm) is the preferred initial approach for accurate staging.
Excisional Surgery - Pre-Op Power Plan
- Patient Evaluation:
- Thorough history (comorbidities, allergies).
- Medication review: Focus on anticoagulants/antiplatelets (target INR < 1.5).
- Informed Consent:
- Essential: Discuss risks, benefits, alternatives; obtain signature.
- Anesthesia Selection:
- Local: Lignocaine (Max: $4.5 \text{mg/kg}$), with Adrenaline (Max: $7 \text{mg/kg}$).
- Consider: Topical, field block based on lesion.
- Site Preparation:
- Antiseptic cleansing (povidone-iodine/chlorhexidine), sterile draping.
- Lesion & Incision Marking:
- Clearly outline lesion margins.
- Plan incision along Langer's lines for optimal cosmesis.
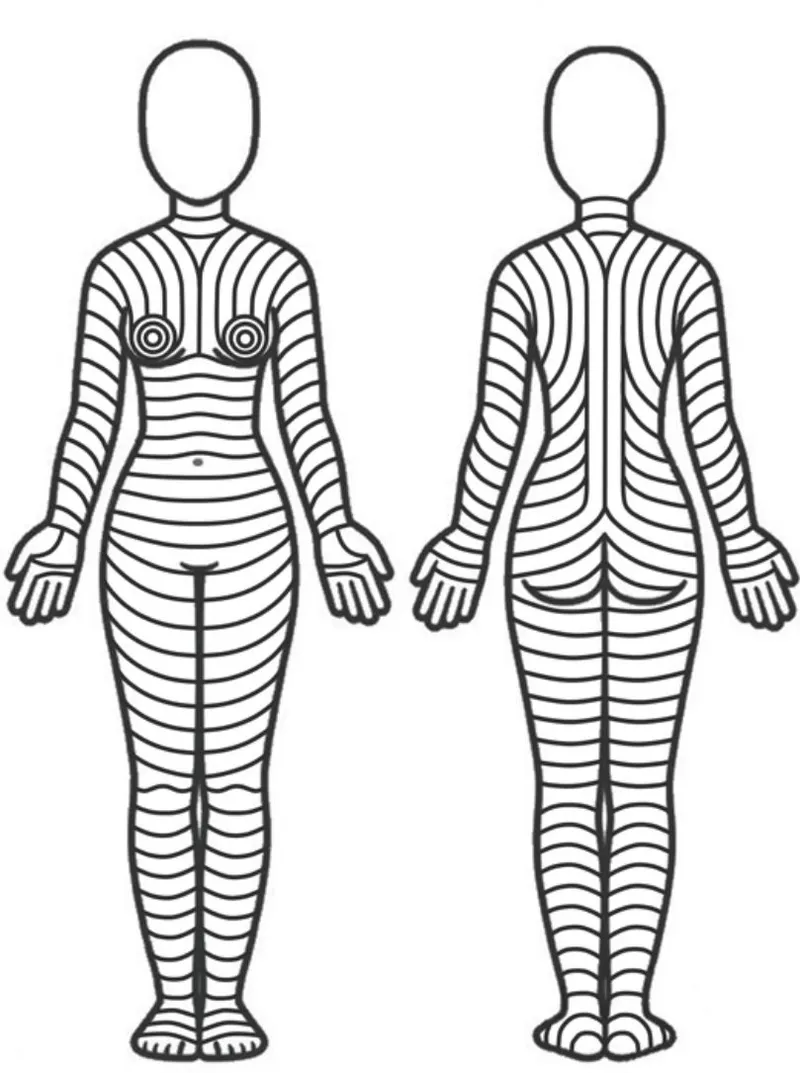
⭐ Adrenaline in local anaesthesia prolongs its duration and provides hemostasis, but must be used with caution in acral areas (fingers, toes, nose, penis) due to risk of vasoconstriction.
Excisional Surgery - Precision Slice Time
- Types:
- Elliptical Excision: Most common. Length:Width ratio 3:1 to 4:1; 30° angle at apices.
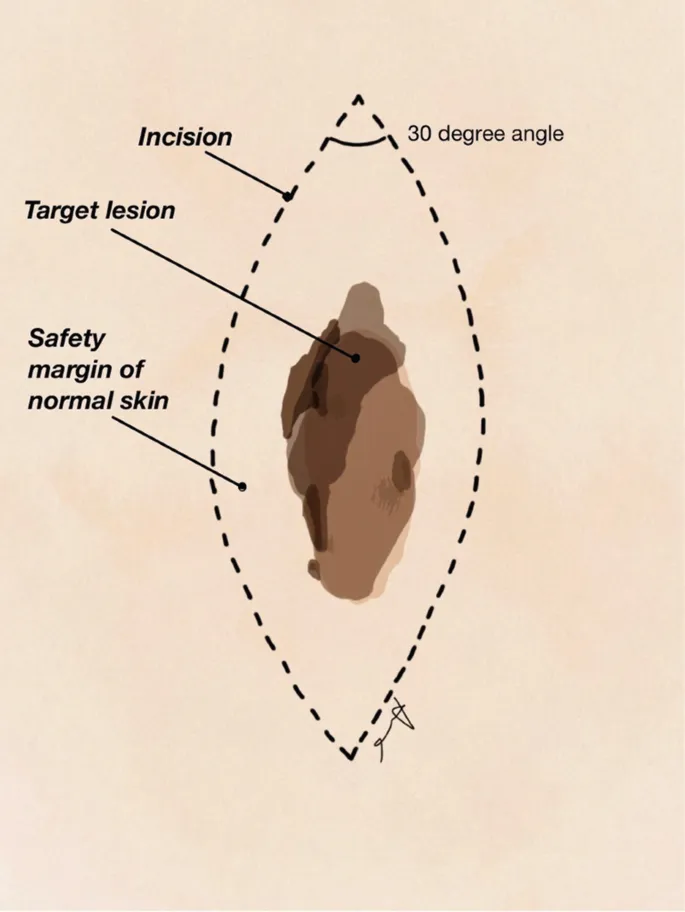
- Wedge Excision: For lip, ear.
- Saucerization/Shave Excision: Superficial lesions (e.g., SKs, superficial BCCs).
- Elliptical Excision: Most common. Length:Width ratio 3:1 to 4:1; 30° angle at apices.
- Surgical Margins (mm): 📌 Mnemonic: "B3-5 S4-6 M-Depth"
- BCC: 3-5mm
- SCC: 4-6mm
- Melanoma: Based on Breslow depth.
- Instruments: Scalpel (#15 blade), forceps, scissors, curette.
- Specimen Handling: Orient & mark for pathologist; appropriate transport medium.
⭐ The long axis of an elliptical excision should ideally be parallel to relaxed skin tension lines (RSTLs) for better cosmetic outcome.
Excisional Surgery - Suture Smartly Now
-
Layered Closure: Essential for healing; uses deep (absorbable), dermal, and epidermal sutures.
-
Suture Materials:
Suture Type Absorbability Tensile Strength (Retention) Common Use Vicryl Absorbable Good (2-3 wks) Deep, Subcuticular Monocryl Absorbable Fair (1-2 wks) Subcuticular Prolene Non-absorbable Excellent Skin, Vascular Nylon Non-absorbable Good Skin -
Suture Techniques: Simple interrupted, continuous (running), mattress (vertical/horizontal), subcuticular.
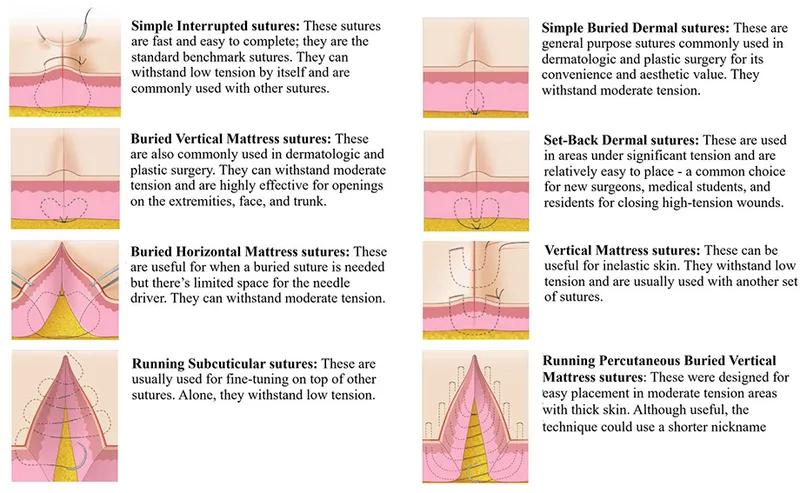
-
Alternatives: Skin staples, adhesive tapes, tissue adhesives (e.g., cyanoacrylates).
-
📌 Suture Removal Times: Face: 3-5d, Scalp: 7-10d, Trunk/Limbs: 7-14d, Joints: 10-14d.
⭐ Eversion of wound edges during skin closure is crucial for minimizing scar depression and achieving a better cosmetic result.
Excisional Surgery - Aftercare Ace
- Post-op Instructions: Keep wound clean & dry initially. Gentle cleansing as advised. Limit activity. Pain relief (e.g., paracetamol). Monitor for infection signs: redness, increasing pain, swelling, pus, fever.
- Suture Removal Times: Face: 3-5 days; Scalp/Trunk: 7-10 days; Limbs: 10-14 days.
- Complications:
- Early: Bleeding, hematoma, infection, wound dehiscence.
- Late: Scarring (hypertrophic, keloid), nerve damage, recurrence.
- Follow-up: Crucial for monitoring healing and detecting late complications; schedule as advised.
⭐ Prophylactic antibiotics are generally not required for routine excisional surgery in healthy individuals but may be considered for high-risk sites or patients.
Table: Common Early Complications & Management
| Complication | Key Signs/Symptoms | Management Approach |
|---|---|---|
| Hematoma | Localized swelling, pain, bruising | Small: observation; Large/Expanding: drainage |
| Wound Infection | Erythema, warmth, pus, ↑pain, fever | Wound care, antibiotics (oral/IV), may need drainage |
| Wound Dehiscence | Separation of wound edges | Assess cause; re-suturing, secondary intention healing |
Flowchart: Managing Suspected Wound Infection
High‑Yield Points - ⚡ Biggest Takeaways
- Indications: Malignant lesions (BCC, SCC, melanoma) and symptomatic/cosmetic benign lesions.
- Surgical margins are crucial for malignancy (e.g., 3-5 mm for BCC).
- Elliptical excision along RSTLs with a 3:1 length-to-width ratio for optimal scarring.
- Layered closure (deep and superficial) minimizes tension for better cosmesis.
- Key complications: infection, bleeding, hematoma, dehiscence, adverse scarring.
- Primarily uses local anesthesia (lidocaine ± epinephrine).
- Adequate hemostasis pre-closure prevents hematoma_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

