Corticosteroids - Skin's Mighty Mutes
- Mechanism (MoA): Anti-inflammatory, immunosuppressive, anti-proliferative, vasoconstrictive. Bind cytoplasmic Glucocorticoid Receptors (GR) → modulate gene expression; Inhibit Phospholipase A2 (PLA2) via lipocortin-1 → ↓ Prostaglandins (PGs) & Leukotrienes (LTs).
- Topical Steroid Potency Classification:
Class Potency Examples (0.05% unless stated) I Superpotent Clobetasol propionate, Halobetasol prop. II Potent Betamethasone dipropionate, Mometasone furoate (0.1% oint) III Upper Mid Fluticasone propionate, Triamcinolone acetonide (0.1%) IV Mid-Strength Mometasone furoate (0.1% cream) V Lower Mid Desonide, Fluocinolone acetonide (0.01%) VI Mild Hydrocortisone (1%) VII Least Potent Hydrocortisone (0.5%) - Key Indications: Eczema (dermatitis), psoriasis, lichen planus, pemphigoid.
- Topical Side Effects: Skin atrophy, striae, telangiectasias, acneiform eruptions, perioral dermatitis, hypopigmentation. Risk of systemic absorption (↑ with high potency, large area, occlusion).
- Systemic Side Effects: 📌 Cushingoid features (moon facies, buffalo hump), HPA axis suppression, osteoporosis, hyperglycemia, immunosuppression, mood changes.
⭐ Tachyphylaxis (acute tolerance) can occur with continuous prolonged topical steroid use, leading to ↓ efficacy.
TCIs & Methotrexate - Steroid Sparing Stars
- Topical Calcineurin Inhibitors (TCIs)
- Examples: Tacrolimus, Pimecrolimus.
- Mechanism: Inhibit calcineurin → ↓ T-cell activation & cytokine release (e.g., IL-2).
- Uses: Atopic dermatitis (especially face, intertriginous areas), vitiligo.
- Advantage: No skin atrophy, unlike topical steroids.
- Side effects: Initial burning/stinging (common, transient), flushing with alcohol.
⭐ Black box warning for TCIs: Rare reports of lymphoma and skin malignancies.
- Methotrexate (MTX)
- Mechanism: Folic acid antagonist; inhibits dihydrofolate reductase → ↓ purine/pyrimidine synthesis.
- Uses: Psoriasis, psoriatic arthritis, pemphigus vulgaris, mycosis fungoides.
- Dosing: Weekly (oral, IM, SC). 📌 Mnemonic: MTX = Must Take Xtra (folate).
- Supplementation: Folic acid (e.g., 5 mg weekly, 24h after MTX) to ↓ toxicity (stomatitis, myelosuppression).
- Monitoring: CBC, LFTs, renal function tests.
- Contraindications: Pregnancy (teratogenic), severe liver/kidney disease, active infection.
Azathioprine & MMF - Purine Pathway Players
-
Azathioprine (AZA)
- Prodrug of 6-mercaptopurine (6-MP); inhibits purine synthesis.
- TPMT testing mandatory. 📌 AZA: "Always Test Purine Metabolism".
- Dose: 1-3 mg/kg/day.
- SE: Myelosuppression (esp. low TPMT), hepatotoxicity, GI upset.
- DDI: Allopurinol (↓ AZA dose 60-75%).
⭐ Azathioprine: risk of myelosuppression, especially with low TPMT activity.
-
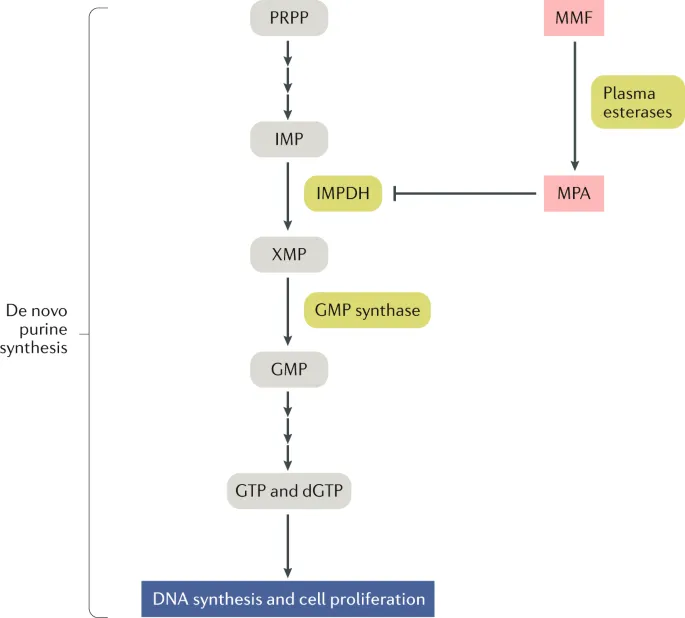
Mycophenolate Mofetil (MMF) / Mycophenolic Acid (MPA)
- MMF (prodrug) → MPA (active).
- MOA: Selective IMPDH inhibitor; blocks de novo purine synthesis in lymphocytes. 📌 MMF "Muffles" IMPDH.
- Dose: MMF 1-2 g/day; EC-MPA 720 mg BID.
- SE: GI intolerance (diarrhea), leukopenia, teratogenic ⚠️.
- Adv: More selective than AZA, no TPMT testing required routinely.
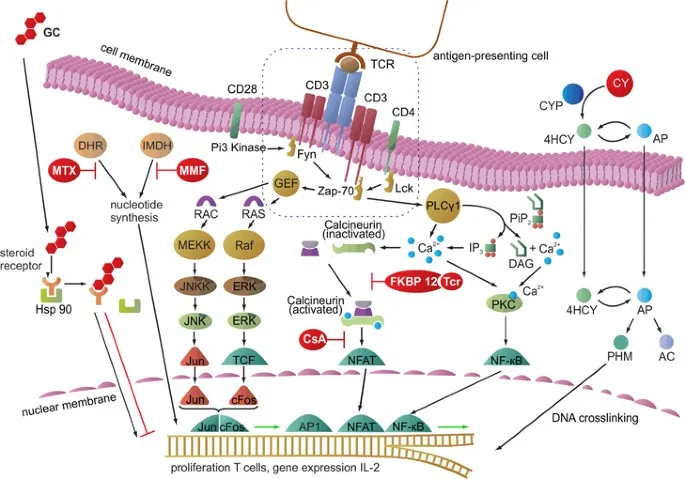
Cyclosporine & Biologics - Precision Power
- Cyclosporine: Calcineurin inhibitor; ↓ IL-2, ↓ T-cell activation.
- Uses: Severe psoriasis, atopic dermatitis, pyoderma gangrenosum.
- Dose: 2.5-5 mg/kg/day.
- Side Effects: 📌 "Hairy Gum Bleeder with Bad Kidneys & BP" (Nephrotoxicity, HTN, Hypertrichosis, Gingival hyperplasia). Monitor renal function (Sr. Cr), BP, K+, Mg2+.
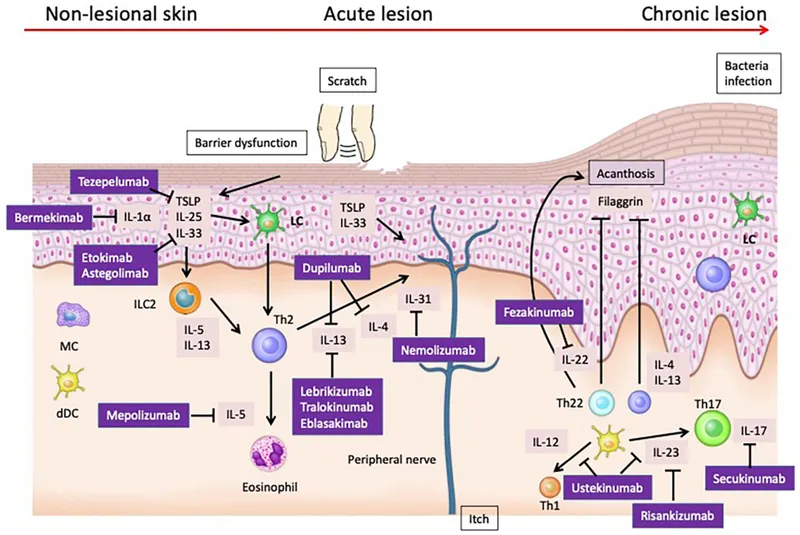
- Biologics: Targeted monoclonal antibodies (mAbs) or fusion proteins.
- Targets: TNF-α (e.g., Infliximab, Adalimumab), IL-17 (e.g., Secukinumab), IL-12/23 (e.g., Ustekinumab), IL-4/13 (e.g., Dupilumab).
- Screening: Latent TB, Hepatitis B/C before initiation.
⭐ Cyclosporine is highly effective for rapid control of severe psoriasis or atopic dermatitis.
High‑Yield Points - ⚡ Biggest Takeaways
- Topical corticosteroids: Potency guides use; watch for skin atrophy and tachyphylaxis.
- Tacrolimus/Pimecrolimus: Steroid-sparing for atopic dermatitis (face/folds); BBW for lymphoma.
- Methotrexate: For psoriasis/eczema; needs folic acid, monitor LFTs/CBC. Highly teratogenic.
- Azathioprine: TPMT enzyme testing vital before use; risk of myelosuppression. For bullous diseases.
- Cyclosporine: Rapid for severe psoriasis/atopic dermatitis; monitor blood pressure and kidney function.
- Biologics: Targeted for psoriasis; TB screening mandatory pre-treatment_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

