Seb Derm 101 - The Greasy Itch
- Chronic, relapsing inflammatory dermatitis presenting with greasy yellow scales and underlying erythema.
- Common sites: scalp (dandruff), face (nasolabial folds, eyebrows, glabella, retroauricular), chest, intertriginous areas.
- Infants ("cradle cap") & adults (peak 30-60 yrs, M > F).
⭐ Seborrheic dermatitis has a biphasic age distribution, peaking in infancy (first 3 months) and again in puberty/adulthood (30-60 years).
Etiopathogenesis - Yeast's Party Foul
- Key Culprit: Malassezia species (e.g., M. globosa, M. restricta), a lipophilic commensal yeast.
- Pathophysiology:
- Malassezia metabolizes sebum triglycerides.
- Produces irritating free fatty acids (e.g., oleic acid).
- Disrupts skin barrier integrity.
- Induces inflammation & keratinocyte hyperproliferation.
- Contributing Factors:
- Genetic predisposition.
- Sebum quantity & composition.
- Immune system status (critical in HIV).
- Neurological conditions (e.g., Parkinson's disease).
- Environmental factors (stress, humidity).

⭐ Association with HIV/AIDS is strong; severe or refractory seborrheic dermatitis can be an early cutaneous marker of HIV infection, often seen with CD4 counts < 400 cells/µL.
Clinical Features - Flakes & Red Faces
- Primary Lesions: Erythematous patches with overlying greasy, yellowish scales ("flakes").
- Scalp Involvement:
- Mild: Diffuse scaling (dandruff).
- Severe: Inflamed, thick, adherent, yellowish crusts; potential hair loss.
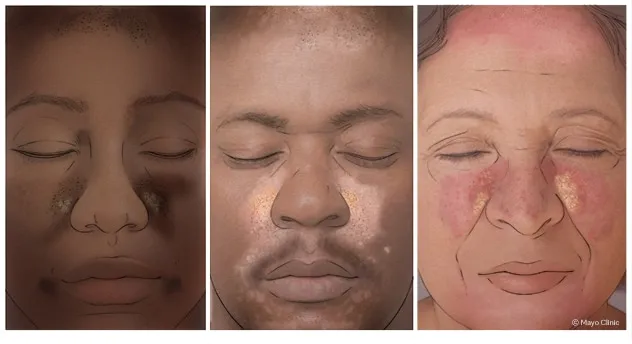
- Facial Involvement ("Red Faces"): Eyebrows, glabella, nasolabial folds, retroauricular. Blepharitis common.
- Other Affected Areas:
- Presternal chest: "Petaloid" or annular configuration.
- Intertriginous zones (axillae, groin, inframammary): Erythema, moist scaling.
- Symptoms: Pruritus (variable, often mild), burning sensation.
⭐ In infants, seborrheic dermatitis often presents as “cradle cap” (adherent, greasy scales on the scalp) but can also affect the face, diaper area, and intertriginous zones.
Diagnosis & DDx - Spotting the Impostors
- Clinical diagnosis usually sufficient.
- Biopsy (rare): Parakeratosis, acanthosis, spongiosis.
- Key DDx:
Condition Key Differentiators Psoriasis Dry, silvery, thick scales; extensor; nail pitting Atopic Dermatitis Intense pruritus; flexural; atopic history Tinea Capitis Alopecia, broken hairs; +KOH/culture Rosacea Redness, telangiectasia, papules/pustules; no scales Discoid Lupus Adherent scale, follicular plugging, atrophy, scarring
⭐ A key differentiator from psoriasis is that seborrheic dermatitis scales are typically greasy and yellowish, while psoriasis scales are dry, silvery, and thicker.
Treatment Toolkit - Taming the Flare-ups
- Goals: ↓ Malassezia, ↓ Inflammation, Remove scales.
- First-line Therapy:
- Topical Antifungals (Ketoconazole, ciclopirox, selenium sulfide, Zn pyrithione).
- Topical Corticosteroids (Low-potency, short-term; e.g., hydrocortisone).
- Scalp Specifics:
- Medicated Shampoos (Ketoconazole 2%, SeS 2.5%).
- Severe: Add topical steroid solution.
- Face/Body Specifics:
- Antifungal Creams (Ketoconazole 2%, ciclopirox 1%).
- Severe: Add low-potency steroid cream (hydrocortisone 1%).
- Adjuncts:
- Keratolytics (Salicylic acid) for thick scales.
- Maintenance:
- Reduced frequency; TCIs (Pimecrolimus, Tacrolimus) for face.
- Refractory Cases:
- Oral antifungals, Isotretinoin, Phototherapy.
⭐ Topical ketoconazole 2% shampoo or cream is a cornerstone of treatment due to its antifungal activity against Malassezia species and its anti-inflammatory effects.
High-Yield Points - ⚡ Biggest Takeaways
- Common sites include the scalp (dandruff), face (nasolabial folds, eyebrows, glabella), chest, and flexures.
- Strongly associated with the yeast Malassezia furfur (Pityrosporum ovale).
- Infantile form is known as cradle cap; adult form is chronic and relapsing.
- Presents with greasy, yellowish scales on an erythematous base.
- Exacerbated by stress, cold/dry weather, immunosuppression (e.g., HIV), and Parkinson's disease.
- Severe or widespread seborrheic dermatitis can be a marker for HIV infection.
- Management includes topical antifungals (e.g., ketoconazole), mild topical corticosteroids, and keratolytics for scales.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

